What Causes Melasma?
Read About Melasma Causes, Along With Treatment & Prevention
Melasma is a common pigmentation disorder that causes dark, uneven patches on the skin, most often on the face. Many people seek treatment because the discoloration can be difficult to cover with makeup and frustrating to manage over time. Although melasma is not medically harmful, it can significantly affect confidence and self-image, especially because it often affects highly visible areas such as the cheeks, forehead, nose, and upper lip. Understanding what causes melasma is an important first step toward improving its appearance, as treatment success often depends on identifying the factors that influence pigment production in the skin. With the right guidance, patients can take a more informed approach to managing this condition and preventing it from worsening. An experienced cosmetic dermatologist, such as Dr. Michele Green, can help patients understand why melasma develops and how to address it effectively.
Melasma develops when the skin has trouble regulating melanin production and distribution, the pigment that gives skin its color. Rather than being caused by a single issue, melasma is influenced by a mix of internal changes and external factors that cause pigment-producing cells to be distributed unevenly. This helps explain why melasma looks and behaves differently from typical dark spots that form from sun damage alone. The depth of the pigment, the type of skin, and how sensitive the skin is can vary widely from one person to another, which means the same treatment does not work equally well for everyone. A thorough skin evaluation helps clarify how melasma is affecting the skin and which treatment options are most appropriate. A board-certified dermatologist like Dr. Michele Green carefully reviews these details to create a treatment plan tailored to each patient.
Dr. Michele Green is an internationally recognized, board-certified cosmetic dermatologist with over 25 years of experience treating melasma and other forms of hyperpigmentation. She is known for her holistic, less-is-more skincare approach, creating customized treatment plans that address each patient’s unique skin concerns, tone, and goals. Dr. Green has consistently been named among New York City’s top dermatologists by Castle Connolly, New York Magazine, and Super Doctors for her expertise and dedication to patient care. At her private dermatology practice on Manhattan’s Upper East Side, Dr. Green combines advanced in-office treatments with carefully selected topical skincare to help patients achieve clearer, more even-toned skin.
What is melasma?
Melasma is a common, benign skin condition that causes dark patches of discoloration on the face and chest. It results from the overproduction of melanin by melanocytes, the skin cells that produce the pigment that gives skin its color. When various factors stimulate melanocytes, they produce excess pigment, which can lead to melasma. Melasma primarily affects the upper lip, the bridge of the nose, the forehead, and the cheeks, often appearing symmetrically on both sides of the face. While it typically occurs on the face, melasma can also appear on the forearms, neck, and shoulders, particularly if they have been exposed to excessive sun or UV radiation.
There are three main types of melasma: epidermal, dermal, and mixed. In epidermal melasma, pigmentation occurs in the skin’s top layer (the epidermis), resulting in dark brown patches with well-defined borders. In dermal melasma, pigmentation appears as light brown or blue-gray, with a blurry border, and is more challenging to treat because it affects the dermal, or middle, layer of the skin. Mixed melasma is the most common form, featuring bluish and brown patches of discoloration in both the epidermal and dermal layers of the skin.
Although melasma is not a harmful skin condition and does not necessarily increase patients’ risk of skin cancer, it can make individuals feel self-conscious about their skin tone, significantly affecting their quality of life. While melasma cannot be cured, it can be effectively treated and managed with in-office treatments, topical medications, skincare products, and lifestyle modifications. Melasma can be a challenging condition to treat, as some pigmentation treatments may worsen its appearance. It’s essential to have your melasma thoroughly evaluated by a board-certified dermatologist, such as Dr. Michele Green, to determine the best treatment plan for your skin.
Who gets melasma?
Melasma can occur in any patient, but it is most common in women aged 20 to 40. Although men can experience melasma, the American Academy of Dermatology reports that only 10% of individuals who develop this skin condition are men. Patients with darker skin, such as those of Latin/Hispanic, African, Mediterranean, or Middle Eastern descent, are statistically more likely to develop melasma. Although patients with lighter skin may develop melasma, it is often less noticeable than in those with darker skin, especially brown skin. This is due to the higher concentration of melanocytes in darker skin.
What causes melasma?
Melasma develops when pigment-producing skin cells, called melanocytes, become overactive and produce excess melanin that settles unevenly in the skin. The exact reason this process begins is not fully understood. In many patients, melasma appears when melanocytes become more sensitive to internal signals and external influences, leading to pigment accumulation in certain areas rather than an even distribution. This increased pigment activity helps explain why melasma differs from common sunspots and other forms of discoloration. The condition often develops when the skin is more prone to discoloration and when changes disrupt normal pigment control, resulting in visible dark patches. Understanding what contributes to this imbalance is an important part of managing melasma, which is why a careful evaluation with an experienced dermatologist, such as Dr. Michele Green, is essential for creating an effective, individualized treatment plan.
How is melasma different from other types of hyperpigmentation?
Melasma differs from other forms of hyperpigmentation in both its formation and its behavior over time. Dark spots, such as sunspots or post-inflammatory pigmentation, usually develop after specific skin damage or long-term sun exposure and often fade once the cause is addressed. Melasma, on the other hand, arises from changes in the skin’s regulation of pigment production. The discoloration is often more widespread, appears on both sides of the face, and can extend deeper into the skin, making it harder to predict and manage. Unlike many other dark spots, which fade and remain lighter after treatment, the pigment-producing cells in melasma-prone skin remain more easily triggered even after the discoloration improves. This helps explain why melasma often returns and why treatments that work well for other types of pigmentation may not be effective or may worsen melasma.
Is melasma genetic?
Genetics can play an important role in the development of melasma, although a genetic predisposition does not guarantee that the condition will appear. Many patients with melasma report a family history of similar pigmentation, suggesting that inherited traits can influence how melanocytes respond to internal and external signals. Genetic factors may affect pigment activity, skin sensitivity, and the strength of melanocyte responses to light, hormones, or inflammation. This helps explain why melasma is more common in certain families and why it occurs more frequently in individuals with naturally darker skin tones, who often have more active pigment-producing cells. However, genetics alone is not responsible for melasma; other internal and environmental factors typically trigger it.
What hormone causes melasma?
Hormonal changes, particularly involving the female sex hormones estrogen and progesterone, are closely linked to the development of melasma. Research indicates that birth control pills, pregnancy, and hormone replacement therapy can all trigger melasma flare-ups. Estrogen may increase melanin receptors in skin cells, making them more sensitive to sunlight and inflammation. Estrogen and progesterone are present in many birth control pills and hormone replacement therapies, and they also surge during pregnancy. This is why melasma is often referred to as chloasma or the mask of pregnancy, due to the increased melanin and hyperpigmentation on the faces of pregnant women. In many cases, hormone-induced melasma diminishes once hormone levels stabilize. However, if it persists for more than three to six months postpartum or after discontinuing birth control, cosmetic treatments may be necessary.
Recent studies suggest that thyroid disease may be associated with the development of melasma. Hypothyroidism, a disorder characterized by an underactive thyroid, prevents the body from receiving normal thyroid hormone levels. This can result in hormonal imbalances, potentially leading to the development of melasma. Additionally, hyperthyroidism, a disorder marked by an overactive thyroid, also seems to influence melasma development. Although the exact mechanism of melasma formation is unclear, these hormones can alter the production of inflammatory cytokines, contributing to skin pigmentation.
What medication causes melasma?
Certain medications have been shown to increase patients’ risk of developing melasma. Antiseizure medications such as Clobazam and Phenytoin are known to trigger or worsen melasma. Birth control pills containing estrogen and progesterone have been shown to elevate the risk of melasma. Other medications, including oral antibiotics, certain blood pressure drugs, and retinoids, heighten skin photosensitivity, increasing the likelihood of sun damage and melasma. If you notice the onset of melasma while taking any of these medications, consult your prescribing doctor to explore alternative treatments that can help prevent the progression of melasma.
What deficiency causes melasma?
Nutritional deficiencies are not considered a direct cause of melasma, but certain deficiencies may be associated with an increased likelihood of developing or worsening pigmentation in some individuals. Research has suggested a possible link between melasma and lower levels of iron, vitamin D, and vitamin B12, all of which play important roles in overall skin health and cellular function. When these nutrients are lacking, normal skin function can be disrupted, potentially affecting pigment production. In some patients, correcting an underlying deficiency has been associated with improved skin tone and a better response to melasma treatment. However, this alone is rarely sufficient to resolve the condition. For this reason, a comprehensive evaluation may include a discussion of dietary habits, medical history, and recent blood work to determine whether nutritional factors could be contributing to pigmentation changes.
What foods cause melasma?
Melasma is not directly caused by food, but certain dietary choices can influence its severity. High-glycemic index foods, such as sugar, white bread, and pastries, may worsen melasma by spiking insulin and disrupting hormone levels. Dairy products and soy-based foods can affect estrogen and progesterone levels, potentially worsening melasma in hormone-sensitive individuals. On the other hand, a diet rich in antioxidants, including berries, leafy greens, and citrus fruits, along with foods high in vitamins C and E, omega-3 fatty acids (such as fish and flaxseed), and minerals such as zinc and selenium, can support skin health and may help reduce the appearance of melasma.
Which cosmetic procedures are best for the treatment of melasma?
There is no single cosmetic procedure that is best for treating melasma, as the condition affects each patient differently and responds uniquely to skin type, skin tone, pigment depth, and individual triggers. Some patients may see improvement with gentle chemical peels, while others require a more targeted approach with treatments designed to regulate pigment activity over time. Melasma also varies in how deeply pigment sits within the skin, which plays an important role in determining which treatments are most appropriate and how aggressive therapy should be. For this reason, effective treatment begins with a thorough evaluation rather than a one-size-fits-all solution. During a consultation, Dr. Michele Green carefully assesses the pattern, depth, and behavior of the pigmentation, along with the patient’s medical history and skincare routine, to determine which in-office procedures are most suitable. In many cases, a combination of treatments and topical skincare provides the best results.
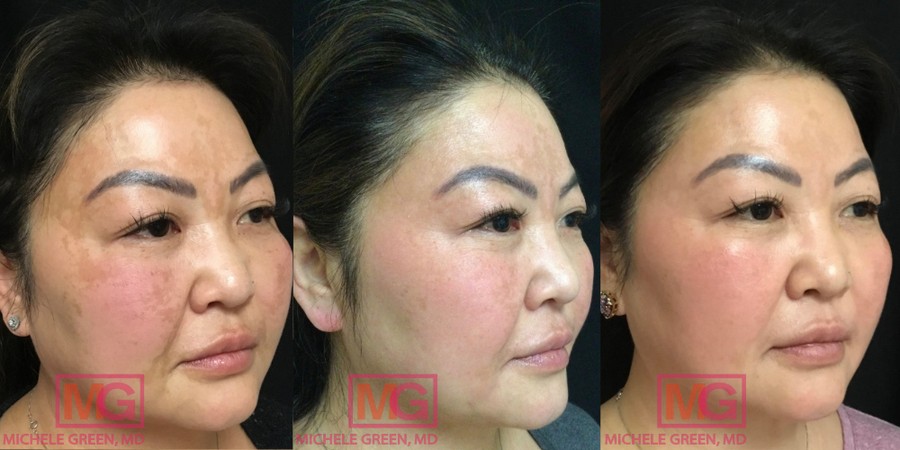
Cosmelan Peels to remove melasma
The Cosmelan peel is Dr. Green’s gold standard for treating melasma and hyperpigmentation. It is a professional-grade mask containing key tyrosinase inhibitors that block melanin production in the skin, along with other lightening agents to restore beautiful, clear skin. The mask is applied and left on for several hours, depending on your skin type and the extent of your hyperpigmentation or melasma. Patients are then instructed to remove the mask with a gentle cleanser and use specially formulated creams to enhance the treatment results and continue lightening the pigmentation. Patients return to Dr. Green’s office four weeks later, where another application of the mask may be performed. The Cosmelan peel is an excellent treatment option for melasma, safe and effective for all skin types and tones, including darker tones. Many patients have achieved significant results with the Cosmelan peel; for many, Cosmelan is the only treatment that has been effective in addressing melasma.
Chemical Peels to treat melasma
Chemical peels are an excellent method for rejuvenating the skin and reducing hyperpigmentation and melasma. They use a chemical exfoliant to gently remove dead, pigmented skin cells, revealing healthy, bright skin beneath. Chemical peels come in various strengths and formulations, allowing for tailored treatment based on your skin type and the degree of pigmentation. In addition to treating melasma and hyperpigmentation, chemical peels can also improve acne scars, fine lines, and wrinkles. Patients with darker skin tones may not be ideal candidates for chemical peels, depending on the strength and ingredients used, as adverse side effects can occur. Often, multiple treatment sessions spaced three to four weeks apart are needed to achieve the best cosmetic results.
Mesopeels for facial hyperpigmentation
Mesopeels are specially formulated chemical peels designed to address a wide range of discoloration, hyperpigmentation, and melasma while helping regulate melanocyte activity. They use chemo-exfoliation that not only revitalizes the skin’s surface like a traditional chemical peel but also stimulates the production of new collagen and elastin. Mesopeels are safe and gentle, suitable for application on various areas of the body, including the face. Unlike other chemical peels, Mesopeels can be used on patients with all skin types and tones, including darker tones. Generally, a series of four to six treatment sessions is necessary to improve facial hyperpigmentation.
Microneedling for melasma
Microneedling, also known as collagen induction therapy, uses micro-needles to create tiny micro-channels in the skin’s surface. By stimulating the body’s natural wound-healing process, microneedling can promote collagen production, diminishing the appearance of fine lines, wrinkles, and uneven skin texture. Additionally, these micro-channels improve the absorption of topical serums and gels. To treat melasma and other forms of hyperpigmentation, Dr. Green applies a depigmentation serum during the microneedling treatment. This serum is rich in skin-lightening ingredients, including tranexamic acid and vitamin C, which help reduce discoloration and create a more even skin tone. Multiple treatment sessions are necessary to address melasma and hyperpigmentation with microneedling.
Microdermabrasion for melasma
Microdermabrasion is a non-invasive exfoliating treatment that helps improve the appearance of dull skin, uneven texture, and superficial discoloration by gently removing the outermost layer of dead skin cells. During the procedure, a handheld device resurfaces the skin while suction lifts away debris and buildup, leaving the skin looking smoother. By clearing away the top layer of rough, pigmented cells, microdermabrasion can help brighten the complexion and support a more even skin tone over time. It can also soften the appearance of enlarged pores, mild congestion, blackheads, and fine lines. Many patients appreciate that the treatment is quick and has little to no downtime.
Hydrafacials to treat facial melasma
A HydraFacial is a three-step, 30-minute procedure that includes deep cleansing, gentle exfoliation, and the removal of impurities from your skin. The HydraFacial uses patented vortex technology to deeply penetrate pores, enhancing cleansing and delivering targeted ingredients into the skin. The first step cleanses the skin, removing superficial impurities. The second step exfoliates the pores, removing dead skin cells, dirt, excess oil, and other impurities. The final step delivers a high concentration of nourishing vitamins and nutrients to hydrate and replenish the skin.
Additionally, the HydraFacial can be enhanced with skin boosters designed to address concerns such as melasma, rosacea, acne, and dehydration. Two excellent boosters for melasma are Britenol and Murad’s Vita-C Serum. Britenol contains alpha-arbutin and vitamin C to brighten the skin while protecting it from free-radical damage and oxidative stress. Murad’s Vita-C includes vitamin C, glycolic acid, tranexamic acid, and RepleniCell, a proprietary Murad molecule that further reduces hyperpigmentation, hydrates the skin, and creates a more even skin tone.
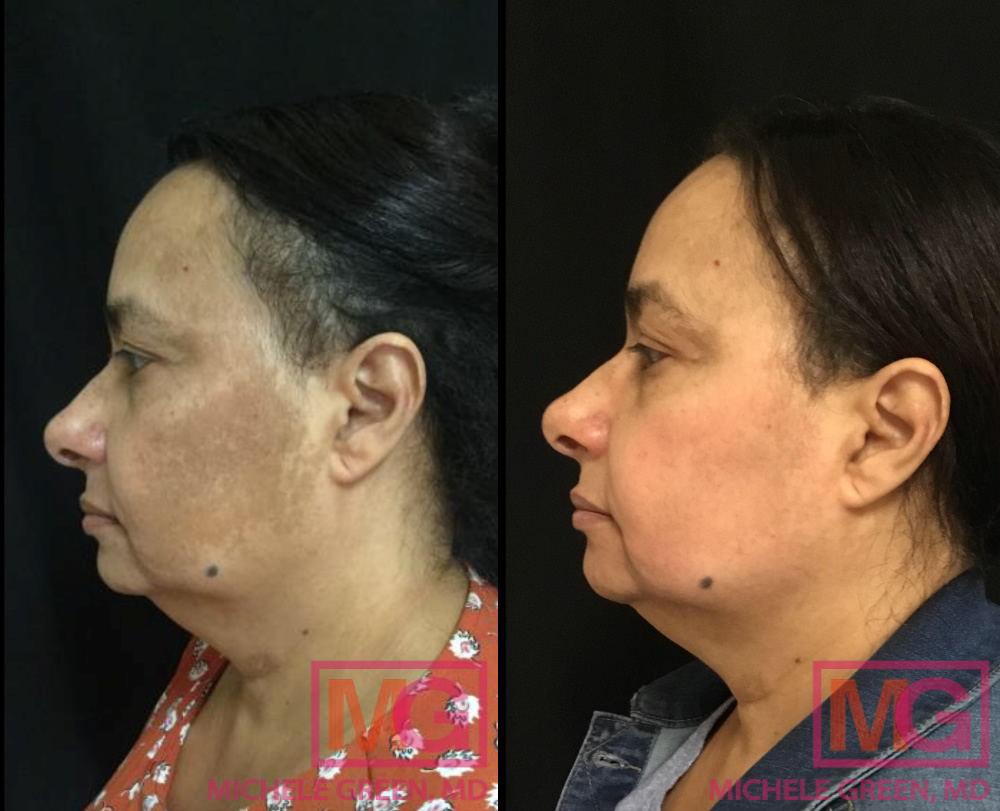
Cosmelan treatment for Melasma – before and after
Which topical skincare products are most effective for treating melasma and dark spots?
A proper skincare regimen is essential for patients with melasma, as targeted products can help lighten pigmentation, maintain treatment results, and prevent the condition from developing or worsening. Dr. Green will create a personalized skincare plan using specially formulated over-the-counter or prescription products tailored to your skin type, tone, and the severity of your hyperpigmentation.
Sunscreen is critical for managing melasma, as sun exposure can worsen the condition. Patients should apply a broad-spectrum sunscreen with an SPF of 50 or higher to protect their skin from the sun’s harmful rays. Dr. Green recommends that patients with melasma layer both a chemical and a physical sunscreen daily for optimal protection. Chemical sunscreens absorb UV rays, converting them into heat and scattering them away from the skin. Common active ingredients in chemical sunscreens include oxybenzone, octinoxate, homosalate, and octocrylene. Physical sunscreens, also known as mineral sunscreens, create a barrier on the skin that filters out harmful UV rays. Physical sunblocks usually contain titanium dioxide or zinc oxide. The Hydrating SPF 50 from Dr. Green’s proprietary skincare line, MGSKINLABs, is a mineral sunscreen that also incorporates hyaluronic acid and lactic acid to hydrate and soften the skin.
Hydroquinones are bleaching agents that lighten facial hyperpigmentation and melasma. Hydroquinone can be obtained only by prescription from a board-certified dermatologist, such as Dr. Michee Green in NYC, and should be used under a doctor’s supervision. Hydroquinones can be applied to the pigmented area for several months to improve the appearance of melasma. When using hydroquinone, it is essential to avoid sun exposure, as this product can increase the skin’s photosensitivity.
Retinoids and retinols are vitamin A derivatives that enhance collagen production and promote skin cell turnover. These products are commonly used to address skin texture and discoloration issues, including melasma, sun spots, fine lines, wrinkles, and acne. Retinoids, such as tretinoin, require a prescription, whereas retinol is available over the counter. The Essential Antioxidant Infusion from MGSKINLABs is enriched with retinol, essential vitamins, and nutrients to exfoliate dead skin cells and nourish the skin, resulting in a brighter, smoother complexion. Like hydroquinones, retinoids can increase the skin’s sensitivity to sunlight and should be used only with proper sun protection.
Vitamin C is a powerful antioxidant that increases skin cell turnover and reduces discoloration, resulting in a brighter, more even skin tone. Its antioxidant properties also protect the skin from oxidative stress and free radical damage. Dr. Green’s MGSKINLABs has developed Vita-C Serum, a vitamin C formulation designed to enhance cell renewal and collagen synthesis, minimize the appearance of brown spots, and improve skin texture.
Corticosteroids can be safely used only for a short duration in combination therapy, as topical steroid creams may thin the skin. They effectively lighten dark skin patches, including those caused by melasma-related pigmentation.
Other effective skin-lightening ingredients for treating melasma include tranexamic acid, azelaic acid, and glycolic acid. MGSKINLAB’s Skin Brightening Cream features a unique blend of kojic acid, glycolic acid, lactic acid, and fruit extracts that gently lighten and reduce skin pigmentation.
Can skincare products alone treat melasma?
Skincare products alone are usually not enough to fully treat melasma, but they play an important supporting role in improving and maintaining results. Topical products such as brightening creams, antioxidants, and prescription treatments can help lighten existing discoloration, slow pigment production, and protect the skin from factors that worsen melasma. These products work gradually and are most effective when used consistently over time. However, melasma often involves deeper pigment changes that topical skincare cannot fully address on its own. As a result, many patients experience only partial improvement when relying solely on skincare. When combined with appropriate in-office treatments and strict sun protection, topical products help maintain results, reduce flare-ups, and support long-term control of melasma.
How can I prevent melasma?
The best way to prevent melasma is to practice proper sun protection. Patients should always apply a broad-spectrum sunscreen with an SPF of 50 or higher. Sunscreen must be used daily, even on cloudy days, because UV rays can penetrate clouds, reflect off snow and puddles, and pass through windows. It’s crucial to reapply sunscreen every 90 minutes or after any water activities. Patients should wear a wide-brimmed hat, sunglasses, and sun-protective clothing to minimize sun exposure. If melasma develops due to specific medications, patients should consult their prescribing provider about alternatives that do not trigger or worsen melasma.
Will melasma go away?
Melasma may fade over time in some cases, but it does not resolve on its own for most patients. Ongoing triggers, including sun exposure, hormonal fluctuations, and genetic predisposition, drive it. Even when melasma lightens temporarily, the pigment-producing cells in the skin remain highly reactive and can be reactivated by even minimal light exposure. This is why melasma is considered a chronic condition that requires long-term management rather than a one-time solution. Although melasma is not harmful to physical health, its unpredictable nature can be frustrating and emotionally distressing. With the appropriate combination of targeted topical treatments, in-office procedures such as Cosmelan peels, and consistent sun protection, melasma can be significantly improved and well-controlled, resulting in a clearer, more even skin tone over time.
Will melasma go away on its own?
Melasma does not typically resolve on its own without active management, even when pigmentation appears to fade temporarily. While some patients notice a slight improvement when a triggering factor, such as pregnancy or hormonal medication, is removed, the pigment-producing cells in the skin often remain highly responsive to light and environmental factors, so melasma can persist even when discoloration appears lighter or less noticeable. Without targeted treatment, the skin can’t regulate this excess pigment production, which is why melasma frequently becomes more noticeable over time. Even patients who experience periods of improvement may see the discoloration return once their skin is exposed to common triggers. Addressing melasma effectively usually requires professional treatment to reduce pigment activity, paired with long-term sun protection and consistent skincare to prevent recurrence and maintain a more even complexion.
Can melasma be cured?
Melasma cannot be permanently cured, but it can be effectively managed and significantly improved with the right approach. The condition stems from ongoing pigment sensitivity in the skin, so the tendency to produce excess pigment does not fully resolve even when visible discoloration fades. Many patients achieve excellent results with professional treatments that reduce existing pigmentation and help regulate melanin production, leading to a more even, brighter complexion. With consistent care, melasma can remain well-controlled for long periods, and in some cases, it may become barely noticeable. Long-term success depends on maintaining results through appropriate skincare and protective measures that help prevent recurrence. Although melasma may not have a definitive cure, proper treatment and maintenance allow most patients to achieve lasting improvement and greater confidence in their skin.
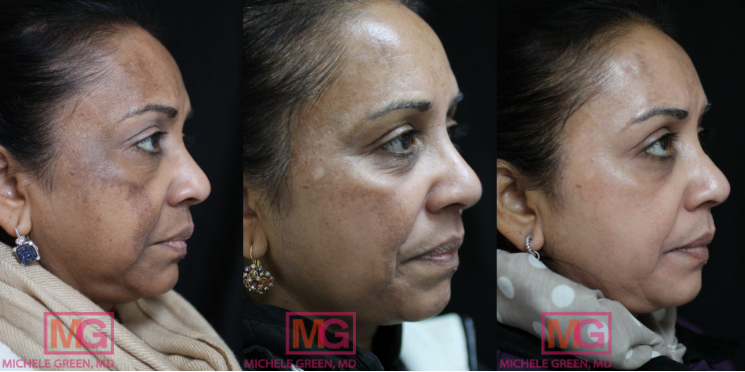
45-54 year old woman, Cosmelan treatment before and after
Frequently Asked Questions (FAQs) about Melasma
What causes facial melasma?
While patchy skin discoloration and dark spots linked to melasma can occur anywhere on the body, they most commonly appear on the face. Melasma on the face can result from various risk factors, including sun exposure, tanning bed use, hormonal fluctuations, and genetic predisposition. Melanocytes are skin cells that produce melanin, the pigment that gives skin its color. In melasma, when melanocytes produce excessive melanin, areas with surplus pigment develop as dark patches that are more pigmented than the surrounding skin. Melasma often appears on the face, which is one of the most sun-exposed areas of the body.
What causes melasma on the upper lip?
In many cases of melasma, a patient may notice the characteristic discoloration above the upper lip. This specific form of melasma is commonly called a “melasma mustache.” Typically, the factors that cause melasma mustache are similar to those that cause other cases of melasma on the face, including sun exposure, hormonal shifts, genetics, thyroid disease, and certain medications. A melasma mustache can be treated with the same topical and in-office procedures used for other melasma patches, providing relief for many patients dealing with this unwanted pigmentation.
What triggers melasma?
The most common trigger of melasma is direct sunlight. Ultraviolet light, including UVA and UVB rays, stimulates melanocytes to produce more melanin. Tanning beds are also known triggers for melasma, as they emit harmful UV rays and visible light that can stimulate melanocytes, worsen skin discoloration, and increase the risk of skin cancer. It is crucial to avoid UV exposure to prevent melasma recurrence after treatment. Even minimal sun or UV exposure can trigger a recurrence of melasma.
Is melasma harmful?
Melasma is not harmful to physical health and does not pose a medical danger to the skin. It is a benign pigmentation condition that does not damage skin cells, increase the risk of skin cancer, or progress into a more serious disease. Melasma is a cosmetic concern that affects skin tone and appearance. That said, the condition can have a significant emotional and psychological impact on many individuals, particularly when the discoloration is difficult to manage. Feelings of self-consciousness, frustration, or lowered confidence are common, especially since melasma often appears on highly visible areas of the face. Melasma does not require treatment for safety reasons, but evaluation by a board-certified dermatologist is still important to confirm the diagnosis and rule out other causes of pigmentation. Once properly identified, melasma can be managed effectively with appropriate treatment and long-term care to improve skin appearance and quality of life.
How does melasma start?
Melasma often begins when a triggering factor activates pigment production in skin already predisposed to discoloration. Common initiating factors include hormonal changes, increased sun exposure, heat, and certain medications that heighten light sensitivity. In many patients, the first signs appear as faint, uneven darkening that gradually becomes more noticeable. These early changes may seem subtle, but continued exposure to triggers allows pigment to deepen and spread.
When does melasma start?
Melasma most commonly begins during periods of hormonal fluctuation or increased environmental exposure, which is why it often appears in adulthood. Many patients first notice melasma during pregnancy, while using hormonal birth control, or during hormone replacement therapy. Others may develop it later from cumulative sun exposure over many years, particularly if they have a genetic predisposition or a darker skin tone. Melasma can also emerge after starting certain medications or following prolonged heat exposure. Although it can begin at different times for different individuals, it is most frequently diagnosed between the ages of 20 and 50.

What causes melasma in females?
Due to hormonal fluctuations, women are significantly more likely than men to develop melasma. Estrogen and progesterone are two hormones linked to the development of melasma. Women who use hormonal birth control or hormone replacement therapy often develop melasma and notice it fades when these medications are stopped. Additionally, melasma commonly appears during pregnancy due to increased hormone levels. Common risk factors for melasma, including sun exposure, genetics, certain medications, and stress, can also contribute to its development in women.
What causes melasma in males?
It is estimated that only 10 percent of melasma patients are men. Nevertheless, a range of environmental and biological risk factors can contribute to the development of melasma in men. Sun exposure is a major trigger, as ultraviolet (UV) light stimulates melanocytes, the pigment-producing cells, to increase melanin production. Furthermore, genetic factors are significant, as melasma often runs in families and is more common among individuals with darker skin tones. Other contributing factors may include heat, stress, certain medications, and cosmetic products that irritate the skin or heighten sun sensitivity. Although men develop melasma less frequently than women, Dr. Green treats both men and women with melasma at her private, boutique dermatology office on Manhattan’s Upper East Side, providing personalized treatment plans tailored to each patient’s skin type, tone, and severity of melasma.
Is melasma cancerous?
No. Melasma is a common skin condition characterized by facial discoloration. It is benign and not cancerous. Skin cancer is a serious disorder caused by the uncontrolled growth of abnormal skin cells. It can appear as dark spots on the skin and may resemble other forms of hyperpigmentation to the untrained eye. If you are unsure whether your dark spots are due to hyperpigmentation, melasma, or skin cancer, it is best to schedule a consultation with a board-certified dermatologist, such as Dr. Green. In certain cases, it may be wise to perform a biopsy of the affected area. Skin conditions that are often mistaken for melasma include lichen planus and lentigines (age spots), among others. The biopsy will involve removing a small piece of the discolored skin for testing to rule out more serious skin conditions. The test results will also reveal the severity of the melasma, indicating its depth and extent. This way, more serious conditions, such as skin cancer, can be ruled out, and an appropriate treatment plan can be established.
How does melasma happen?
Melasma occurs when melanocytes, the cells that produce skin pigment, produce excess melanin that becomes unevenly distributed across the skin’s surface. This process is driven by light exposure, hormonal signaling, and skin inflammation. When melanocytes are repeatedly stimulated, they deposit pigment more deeply and irregularly than normal, leading to the patchy discoloration characteristic of melasma. Over time, this excess pigment accumulates in specific areas of the skin, especially on the face, where exposure to sunlight and visible light is most consistent. A single event does not cause the condition; rather, it develops through repeated activation of pigment cells that disrupt the skin’s ability to maintain an even tone. Once these pigment cells are activated, they can remain overly responsive, which explains why melasma behaves differently from other types of hyperpigmentation.
What causes melasma on the face?
Melasma on the face develops when pigment-producing cells called melanocytes become overstimulated and produce excess melanin in localized areas of the skin. The face is particularly prone to melasma because it is exposed daily to sunlight and heat, which can activate melanocytes and worsen pigmentation. Hormonal influences play a major role, especially fluctuations in estrogen and progesterone, which can increase the skin’s sensitivity to light and trigger excess pigment production. This is why melasma frequently appears during pregnancy, while using hormonal birth control, or during hormone replacement therapy. Genetics also contributes, as individuals with a family history of melasma are more likely to develop facial pigmentation, especially those with darker skin tones who naturally have more active melanocytes. Certain medications and skincare products that increase photosensitivity or irritate the skin can further stimulate pigment formation on the face. When these internal and external factors interact, melanin becomes unevenly distributed, leading to the characteristic patches of discoloration most commonly seen on the cheeks, forehead, nose, and upper lip.
What causes melasma in pregnancy?
For many pregnant women, the development of melasma can be a frustrating aspect of pregnancy. Often called chloasma or the “mask of pregnancy,” melasma can occur due to elevated estrogen and progesterone levels, particularly during the third trimester. Fortunately, for most patients, pregnancy-induced melasma typically fades on its own after childbirth as hormone levels normalize. Additionally, if you’re experiencing melasma during pregnancy, safe and effective topical treatments, such as vitamin C, can help reduce pigmentation. If melasma persists for three to six months postpartum, it may indicate the need for cosmetic treatments, such as the Cosmelan peel, to fully address the pigmentation.
What causes a melasma mustache?
A melasma mustache develops when pigment-producing skin cells become overactive, creating darker discoloration across the area between the nose and upper lip. This pattern is strongly influenced by hormonal sensitivity, which is why it is frequently seen in women who are pregnant, using hormonal birth control, or undergoing hormone replacement therapy. Heat and visible light can further activate pigment in this area, making the discoloration appear more concentrated and difficult to fade. In some patients, thyroid imbalance or medications that increase photosensitivity may also contribute to the development of this pattern. The melasma mustache can be difficult to get rid of because everyday exposure to light can repeatedly stimulate pigment in the same location, even when the rest of the face appears more even. Effective management typically focuses on reducing pigment activity while protecting the skin from environmental triggers that commonly affect this highly sensitive area.
Why is my melasma getting darker?
UV radiation from sun exposure and tanning beds is the primary factor that can exacerbate melasma, as it prompts melanocytes to produce more melanin. When melanocytes are stimulated unevenly, melanin can accumulate in specific areas of the face rather than others, eventually leading to melasma. This is why most individuals notice their melasma symptoms worsen during the summer months. To reduce UV-induced melasma, patients should use adequate sun protection, including sunscreen and wide-brimmed hats. Hormonal fluctuations, particularly estrogen, can also aggravate melasma by stimulating melanocytes to produce more pigment. This explains why pregnant women and those using oral contraceptives are at a higher risk of developing melasma.
Other factors that can worsen melasma include certain antiseizure medications, phototoxic drugs, and hypothyroidism. Additionally, some over-the-counter skincare products, especially harsh exfoliants and photosensitizing agents, can worsen the appearance of melasma. If you notice skin changes shortly after starting a new product or medication, it may indicate that the product or medication is triggering your melasma. By identifying your triggers and practicing sun protection, you can help prevent your melasma from worsening or recurring.
Can lasers treat melasma?
No, laser treatment for melasma is not recommended. Lasers such as IPL, Fraxel, and Picosure effectively treat other forms of pigmentation, including sun spots, age spots, and freckles. However, when applied to melasma, the heat from these lasers can “burn the pigmentation,” making the melasma more entrenched in the deeper layers of the skin and much harder to remove. Dr. Green often sees patients who have tried laser treatments for pigmentation, and in many cases, these treatments can worsen the appearance of melasma. Dr. Green prefers to treat melasma with gentle peels, such as the Cosmelan peel or Mesopeels, to minimize the risk of exacerbating existing hyperpigmentation. Dr. Green understands the importance of accurately diagnosing and effectively treating pigmentation the first time, with the safety and satisfaction of her patients being her top priorities.
Why does melasma come back?
Melasma is a chronic skin disorder with multiple underlying causes. In some cases, the dark patches may fade naturally once the cause is treated. However, most patients with melasma require intervention to fully resolve the hyperpigmentation, which may include targeted topical treatments and non-invasive cosmetic procedures such as the Cosmelan peel. Melasma can recur even after treatment if patients fail to practice proper sun protection. During and after treatment, patients must exercise extreme caution in the sun, as any exposure can trigger a recurrence. A broad-spectrum sunscreen with at least SPF 50 should be applied to guard against both UVA and UVB rays. For optimal protection, Dr. Green recommends that her patients use two types of sunscreen: layering a chemical sunscreen beneath a physical sunscreen for the best defense.
Additionally, melasma may recur due to certain medications. Melasma is a challenging skin condition to treat and manage. Trusting an experienced expert to develop your treatment plan is the most effective, efficient, and safest way to achieve a clear complexion while maintaining beautiful, youthful-looking skin over the long term. Dr. Green has over two decades of experience treating melasma and hyperpigmentation in patients of all skin types and tones. She dedicates time to customizing your melasma treatment plan to address your specific skin concerns and aesthetic goals. Moreover, she will create a personalized skincare regimen and discuss any necessary lifestyle changes to help you keep your melasma at bay for good.
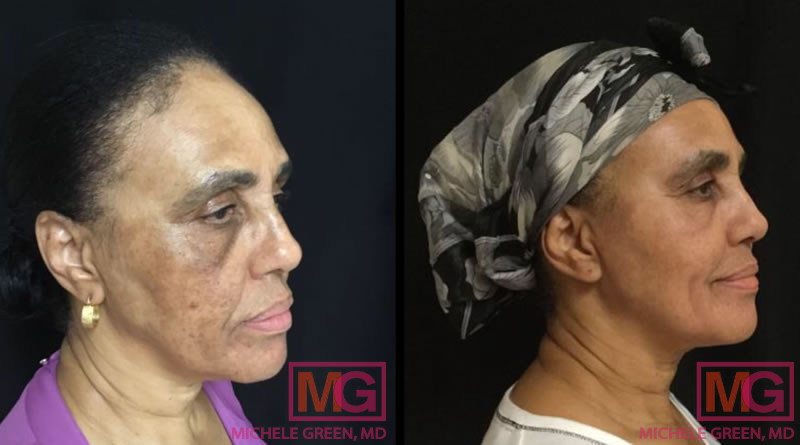
Where does melasma come from?
Melasma begins when melanocytes respond abnormally to signals that regulate pigment production. These signals influence not only melanin production but also how deeply pigment settles in the skin layers and how evenly it is distributed. In melasma, this regulation is disrupted, leading to concentrated areas of pigmentation that do not fade like typical sun-related dark spots. Long-term interactions between pigment cells and the external environment shape the condition. This internal imbalance explains why melasma differs from other forms of discoloration and why it often requires targeted treatment to restore more even pigment activity.
Why is melasma difficult to treat?
Melasma is difficult to treat because the pigment-producing cells remain highly sensitive and reactive. Even after visible dark patches fade, the underlying tendency to produce excess pigment often persists. This makes melasma prone to recurrence or worsening when the skin is exposed to everyday influences such as sunlight, heat, or visible light. In many cases, the pigment also extends deeper into the skin, limiting the improvement achievable with surface-only treatments. Some common pigmentation treatments that work well for sun spots or age spots can actually aggravate melasma, leading to darker or more widespread discoloration. Successful management usually requires a carefully tailored approach that combines appropriate in-office procedures, targeted topical care, and strict long-term sun protection to gradually calm pigment activity and maintain a more even skin tone.
What increases melasma?
Melasma tends to worsen when the skin’s pigment-producing cells are repeatedly stimulated over time, allowing discoloration to deepen, darken, or spread. Even low levels of daily light exposure can gradually intensify existing pigmentation, especially when the skin is not consistently protected. Heat exposure can also play a role, as warmth increases skin inflammation and blood flow, which can indirectly stimulate pigment activity. Changes within the body that affect skin sensitivity, such as shifts in hormone levels or internal inflammation, may further amplify melanocytes’ response to environmental exposure. Certain skincare habits can also worsen melasma, particularly the use of irritating products that disrupt the skin barrier and trigger inflammation. When the skin barrier is compromised, pigment regulation becomes less stable, leading to discoloration that intensifies over time. These cumulative influences help explain why melasma may become darker, more widespread, or harder to control if protective measures are not consistently followed.
What causes melasma to spread?
Melasma can spread when pigment production in the skin becomes less controlled, affecting areas beyond where the discoloration first appeared. This often occurs when the skin is repeatedly irritated, disrupting normal pigment production and allowing dark patches to widen. Aggressive skincare routines, harsh exfoliation, or inappropriate cosmetic treatments can contribute to this process by increasing skin sensitivity and inflammation. In some cases, aggressive attempts to treat pigmentation may unintentionally worsen its distribution, making the affected areas appear larger than they originally were. Managing spread typically focuses on stabilizing pigment activity and protecting the skin to make it appear more even in tone.

Cosmelan – 10 weeks before and after
How do I get started with the best melasma treatment today?
Melasma is a complex pigmentation condition driven by changes in how the skin regulates and produces melanin, often resulting in uneven dark patches that can be difficult to manage without proper care. Understanding the causes of melasma is an essential first step in addressing the condition effectively, as successful treatment depends on identifying contributing factors and selecting appropriate therapies that calm pigment activity and support long-term skin balance. With the right combination of in-office treatments, targeted topical skincare, and consistent protection, melasma can be significantly improved and kept under control over time. Because each patient’s skin responds differently, an individualized approach is critical for achieving the best cosmetic outcome. An expert in cosmetic dermatology, such as Dr. Green in NYC, will evaluate your skin, review your medical history, and create a personalized treatment plan designed to improve pigmentation while maintaining healthy, radiant skin.
Dr. Michele Green is an internationally renowned, board-certified cosmetic dermatologist with over 25 years of experience providing some of the world’s most discerning clients with the finest non-invasive melasma treatments, including Cosmelan peels, Mesopeels, and microneedling. Dr. Green takes a holistic approach and adheres to a less-is-more philosophy in facial rejuvenation, tailoring each patient’s treatment plan to address their unique concerns and aesthetic goals. She is consistently recognized by Castle Connolly, New York Magazine, Super Doctors, and The New York Times as one of New York City’s top dermatologists for her dedication to patient care and expertise. If you are seeking the best melasma treatment in New York, please call our office at 212-535-3088 or contact us online to schedule a consultation and begin developing your customized treatment plan with Dr. Green today.
 212-535-3088
212-535-3088 



