Psoriasis Treatment
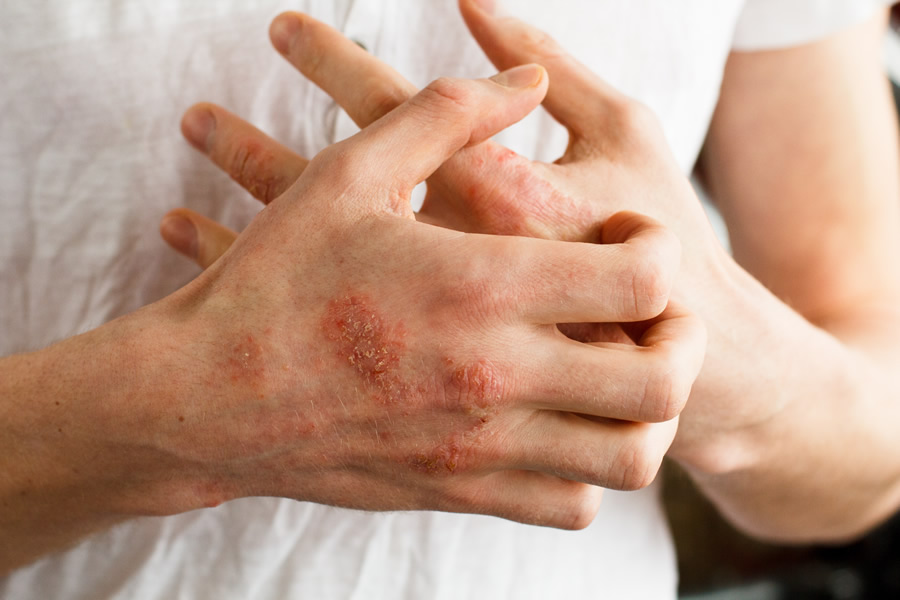
Psoriasis is one of the most common skin diseases in the world, and particularly in the United States. Eight million people suffer from psoriasis in the United States, and approximately 20 percent of these individuals have psoriatic arthritis. Psoriasis can often be misdiagnosed as other skin diseases, since it can present similar in appearance to other skin rashes, such as eczema or Tinea corporis (fungal infections). A psoriasis doctor, like Dr. Michele Green, is a board certified dermatologist, who is an expert in both diagnosing psoriasis and other dermatologic conditions, but also providing the best topical or systemic treatment available. There is a myriad of psoriasis treatments now available to treat this skin disease, from steroid creams, to retinoids, light therapy, and biologics. It is paramount to consult with an expert, like Dr. Green, for your psoriasis treatment, to help manage your disease safely and effectively.
What is psoriasis?
Psoriasis is a common, chronic skin condition in which skin cells grow at an accelerated rate. This skin disease is believed to be an autoimmune disorder, caused by overactive skin cells, which leads to a buildup on the skin of thick plaque in either large or small patches. Psoriasis can be caused or aggravated by either genetic or environmental factors, such as skin irritants, certain infections, or medications.
Dermatology and Psoriasis
Psoriasis can be itchy or uncomfortable, and your dermatologist should be your first destination for the best psoriasis treatment. Board-certified dermatologist, Dr. Michele Green, is trained to identify and treat symptoms of psoriasis, working with you to explore skin care treatment options and create personalized, wholistic health care.
Types of psoriasis
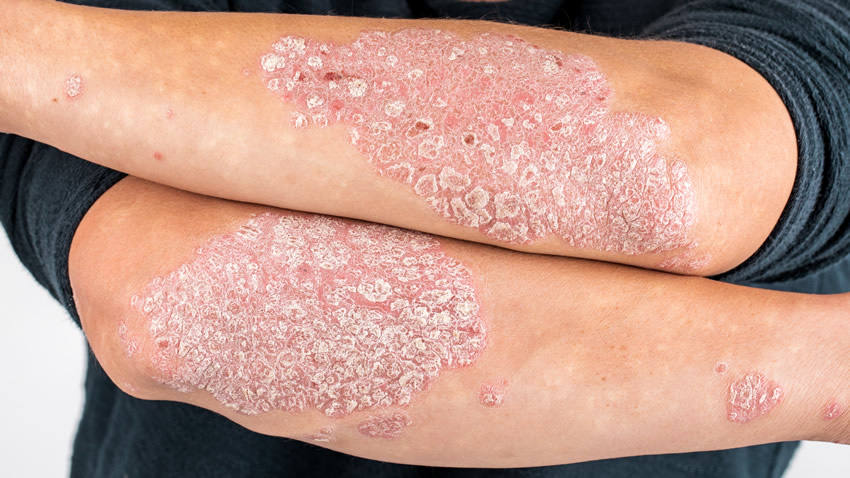
Plaque Psoriasis
Plaque psoriasis is the most common type of psoriasis. Plaque psoriasis varies from mild (covering 3% of the skin) to severe (covering 10% or more of the body), and is due to an expedited growth of skin cells where, instead of cells developing over several weeks, they develop over several days, leading to the most identifiable symptom of plaque buildup. Plaque may range in color from silver to red, and typically appears on the feet, knees, lower back, elbows and hands. Other symptoms and skin problems include:
- Dry skin thatmay flake, crack or bleed
- Itchy, stinging, or burning skin that is sensitive to touch
- Thick or rounded fingernails
- With severe psoriasis: pus-filled blisters
Symptoms from plaque psoriasis can occur anywhere on the body and, as it is chronic, symptoms will usually wane and then later appear as flare-ups, similar to atopic dermatitis (eczema).
Guttate Psoriasis
Guttate psoriasis is less common than plaque psoriasis, and the patterning of psoriasis appears as smaller, tear-drop shaped red spots along the skin. Guttate psoriasis is occurs when the immune system begins to attack normal cells within the body, and is often triggered by an initial infection, such as:
- Bacterial Infection (primarily strep throat)
- Tonsilitis
- Upper Respiratory Infection
Guttate psoriasis also varies in intensity from mild to severe but, depending on the location, may be considered as a more severe case. For example, if a patient has lesions on the face or scalp psoriasis, a dermatologist may classify this as more severe due to the way this affects the patient’s quality of life.
Erythrodermic Psoriasis
Erythrodermic psoriasis is a very rare, very severe psoriasis that can lead to other medical complications, and can sometimes be life-threatening. This form of psoriasis occurs when the immune system produces an abundance of T-cells, which typically are used to fend off disease, and the T-cells move to destroy healthy skin cells. Symptoms of erythrodermic psoriasis usually develop out of other forms of psoriasis, but additionally can include:
- Pain in the joints and nails
- Severe redness, itching and pain
- Sheets (rather than flakes) of skin shedding
- Burnt-looking dermis
- Postules and blisters
- Higher heart rate
- Large body temperature changes
Erythrodermic psoriasis often can develop when treatment of psoriasis is inconsistent, but can also be triggered by an allergic reaction, sunburn, or overuse of corticosteroids. In some cases, erythrodermic psoriasis can throw off a psoriasis patient’s body chemistry, which puts the patient at an increased risk for life-threatening complications due to fluid retention, infection, pneumonia, or congestive heart failure. Therefore, it is essential that you contact your health provider if you think you may have erythrodermic psoriasis.
Pustular Psoriasis
Pustular psoriasis is another rare form of psoriasis that can sometimes be coupled with plaque psoriasis. It is more common in adults than children, and is identified by white bumps that are filled with pus, found on hands and feet. There are three distinct types of pustular psoriasis that vary in intensity.
The first, Palmoplantar pustulosis, is the most mild case, in which small blisters can crust over or crack and symptoms may fade. Acropustulosis is accompanied by a greater amount of pain from very small, white blisters and legions on the infected area. If you observe red, tender skin that quickly develops large blisters overtop, you may have generalized pustular psoriasis, which is an extremely rare, severe psoriasis that requires immediate medical attention.
Psoriatic Arthritis
According to a study from the National Psoriasis Foundation, 30% of psoriasis patients in the United States end up with psoriatic arthritis, which is a painful condition that creates stiffness and limited mobility in the joints due to inflammation from psoriasis.
People with psoriasis and psoriatic arthritis are often at greater risk for other medical issues such cardiovascular disease and diabetes, and therefore should keep all health care providers up-to-date on any flare-ups or further developments. Psoriatic arthritis may also require the joint care of your dermatologist and a rheumatologist, as rheumatology focuses on a variety of different arthritic diagnoses.
What are my psoriasis treatment options?
Though there is currently no cure for psoriasis exists, a variety of clinical trials are underway to continue the investigation of psoriasis. Psoriasis symptoms can be treated through a variety of different treatment options:
- Topical treatments such as creams, lotions, oils and gels (Over-the-counter and prescription)
- Therapy that targets and supports the immune system (Cyclosporine, Methotrexate, Retinoids)
- Live-organism therapy (Biologic agents like Enbrel or Humira)
- Light therapy (Ultraviolet light lasers, PUVA and and UVB Phototherapy)
How does light therapy treat psoriasis?
Phototherapy, or light therapy, exposes the skin to lasers, LED lights, and ultraviolet or infrared radiation in order to either treat the whole body or target specific areas of irritated skin. Excimer lasers are a preferred form of light therapy as they can target specific areas of the skin in fewer treatments, preventing the damage of healthy skin and other side effects that can occur.
In extremely severe cases of psoriasis, PUVA phototherapy may be used, which is an aggressive form of therapy to keep severe psoriasis symptoms at bay. Ongoing studies are being carried on related to light therapy treatments and their increased risk of skin cancers, such as squamous cell carcinoma, and malignant melanoma.
If you’re frustrated with the appearance of your psoriasis, there are multiple treatment options. Contact us online today or call 212-535-3088 to learn more about how Dr. Green’s individualized approach to psoriasis treatment can help you.
 212-535-3088
212-535-3088 



