Atypical Nevus
An atypical nevus, or dysplastic nevus, is a benign skin lesion with unusual features. Atypical nevi share some clinical and histologic characteristics with malignant melanoma, making them difficult to distinguish. While dysplastic nevi aren’t cancerous, they have the potential to change over time and develop into skin cancer. Melanoma is the most serious type of skin cancer due to its invasive nature and lethality. Early detection and treatment of skin cancer significantly improves survival, which is why regular skin checks with a dermatologist and self-examination between checks are so important. A board-certified dermatologist like Dr. Michele Green in NYC can biopsy an atypical mole to confirm a diagnosis, keeping you safe and healthy.
Atypical nevi are extremely common, with about 1 in every 10 Americans having at least one atypical nevus. Atypical moles may resemble melanoma in many ways, usually appearing larger than normal moles, having irregular borders, and varying in color. Individuals with atypical moles and a family history of skin cancer have an increased risk of melanoma. Other common risk factors for melanoma include the presence of atypical moles and fair skin, light eyes or hair, many moles or freckles, an inability to tan, and previous sunburn. Individuals at higher risk should have skin checks with a dermatologist every 4-6 months. Monthly self-examinations are important for catching new melanocytic skin lesions and malignant transformation of atypical nevi, which may present as changes in size, color, or shape.
Dr. Michele Green is an internationally renowned board-certified dermatologist with over 25 years of experience treating and evaluating moles, including atypical nevi and skin cancers. Dr. Green has consistently been recognized by Castle Connolly, New York Magazine, Super Doctors, and The New York Times as a top dermatologist in New York City for her expertise and dedication to her patients. In her private NYC dermatology office, she will conduct a full skin examination to assess all new and existing melanocytic nevi and work with you to create a treatment plan for your individualized skin concerns.
What is an atypical nevus?
Nevus is the medical term for a mole. Melanocytes are the skin cells that produce pigment. A nevus is formed when melanocytes clump together. A nevus is defined as atypical when there is a presence of unusual or abnormal cells in the tissue. Atypical nevi differ from moles in border appearance, color, size, and shape. An atypical nevus may share some clinical or microscopic features with malignant melanoma, but it is NOT a melanoma or any form of skin cancer. An atypical nevus, also called a dysplastic nevus or Clark’s nevus, is a benign melanocytic skin lesion. The presence of multiple atypical nevi may be a marker for an increased risk of developing malignant melanoma. If you have a history of atypical nevi, regular skin checks should be a priority.
What does an atypical nevus or atypical mole look like?
Atypical moles are irregular in shape with borders that fade into the skin. Due to the nature of their development, they can have variations in color and size. A single lesion can be flesh-colored, pink, reddish pink, dark brown, or multiple variations of pink and brown. They are often flat or raised with pebbly-like areas. According to the Journal of the American Academy of Dermatology, atypical moles may be larger than other common moles and are typically irregular with indistinct borders.
Atypical nevi have what we refer to in health care as the ABCDE resemblance to malignant melanoma, meaning that atypical nevi share similarities to melanoma; however, their clinical histology differentiates them. The ABCDE mnemonic is utilized during skin examinations by board-certified dermatologists like Dr. Michele Green to identify a suspicious lesion.
- Asymmetry – it is irregular in shape, size, diameter, and color.
- Border irregularity – imperfect edges that are scalloped.
- Color – variation in pigmentation that is not uniform. Some moles may have variations of the same pigment or color or multiple shades of pigmentation. They range in color from flesh-colored to tan, brown, and even bluish.
- Diameter – melanomas are usually greater than 6mm in thickness at the time of diagnosis; however, there have been instances where they are smaller.
- Evolving – has there been a change in the appearance of the mole over the past weeks or months?
In addition to this concept, the “ugly duckling” method is sometimes used. The “ugly duckling” methodology isolates the mole that is different from all the other moles or the “outlier.” Many different types of skin lesions, from atypical moles and melanoma to seborrheic keratosis and basal cell carcinoma, can fulfill one or more of the ABCDE criteria – thus, it is essential to consult with a board-certified dermatologist such as Dr. Michele Green in NYC for the proper assessment of any suspicious lesion.
Where on the body are dysplastic nevi located?
Dysplastic nevi may be located anywhere on the body. Generally, they can be found in areas with more significant sun exposure, such as the arms, legs, back, and face. However, since most atypical or dysplastic nevi are genetic, they can be located anywhere on the body, including non-sun-exposed areas of your skin. You can even have dysplastic nevi located on the scalp, which is why it is important to have your scalp examined by a dermatologist during your skin check. Most individuals with dysplastic nevi also tend to have an increase in the number of common nevi as well. As a result, you must have annual visits with your dermatologist, which include a thorough head-to-toe examination.
Does atypical mole mean it’s precancerous?
An atypical mole is not always precancerous. A skin biopsy is the only effective method in determining if an atypical mole indicates precancerous changes or cancer. Most people with atypical moles do not develop skin cancer, although having many atypical moles is associated with an increased risk of melanoma. According to The National Skin Cancer Foundation, individuals who have ten or more atypical moles are at a twelve-fold increased risk of developing melanoma compared to the general population. Additionally, an atypical mole can indicate other types of skin cancer, such as squamous or basal cell carcinoma. If you have noticed abnormal changes to an existing mole or a new and unusual growth, Dr. Green can perform a complete skin check to screen for atypical moles and skin cancer.
What is the best way to diagnose a dysplastic nevus?
The proper identification of an atypical mole from a malignant melanoma can sometimes be challenging. An experienced board-certified dermatologist, however, should be able to properly diagnose and determine which moles need to be biopsied or removed for further testing. Some dermatologists may utilize dermoscopy (a microscopic magnifier used to examine the surface of the skin) while performing your skin exam to help identify skin cancer. For example, under dermoscopy, a dysplastic nevus can have the appearance of a fried egg. In addition, if you have a lot of moles, your dermatologist may also suggest having mole mapping. Mole mapping entails taking photographs of the entire body to monitor changes in your moles over time. This technique can also be useful in the early detection of skin cancer.
In her private NYC dermatology office, Dr. Green will first examine your entire body for any unusual moles or growths present. If she has any suspicions of skin cancer, she will biopsy the mole and send the tissue to a laboratory for further testing. A dermatopathologist will then observe the cellular characteristics of the sample to determine if the mole is benign, precancerous, or cancerous. Dr. Green will then recommend treatment options depending on the results of the biopsy.
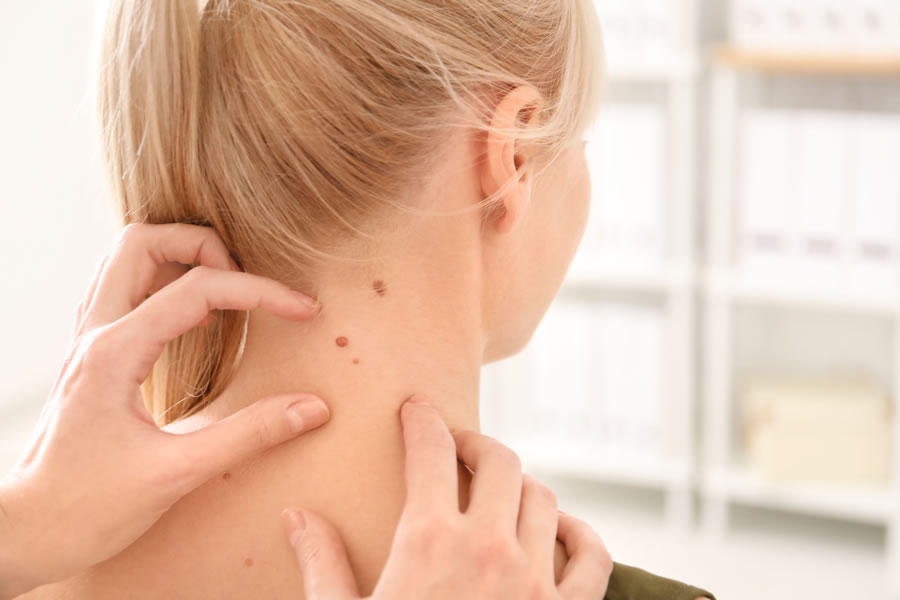
Do atypical moles need to be removed?
Any suspicious skin lesion should be biopsied and sent to a laboratory for examination. It can be difficult at times to visually differentiate between a normal mole and other melanocytic lesions, even for a board-certified expert. A biopsy is the only conclusive way to determine whether a mole is an atypical nevus or a malignant melanoma. There are several types of biopsy techniques, and the size and clinical suspicion of the lesion will determine the technique used. An experienced dermatologist, like Dr. Michele Green, will either perform a punch, excision or shave biopsy and send the specimen to the lab for review and processing. A dermatopathologist will histologically review the specimen under a microscope and provide an accurate diagnosis. According to the Journal of the American Medical Association of Dermatology (JAMA), “The agreement between the clinical diagnosis of an atypical mole and the pathologist’s interpretation of dysplasia has been reported as low as 60%;” thus, it is essential to have any suspicious lesions biopsied and analyzed in order to gain an accurate assessment. Further treatment for a lesion will depend on the diagnosis from the dermatopathologist.
There are instances in which the biopsy results reveal mild to moderate atypia. Depending on the histologic interpretation of the atypia, your dermatologist may need to remove more skin around the lesion or perform a deeper excision. In low-grade lesions with mild atypia, no further treatment is usually necessary. However, there are instances where the diagnosis indicates severe atypia. In these instances, it is usually recommended that further treatment be done to remove the atypical mole. Generally, most dermatopathologists will recommend a deeper shave or excisional biopsy to clear the margins and remove any underlying atypical cells. Once the margins are clear, there is very little concern that the atypical nevus will require any further dermatologic treatment.
Do atypical moles change?
Yes! Atypical moles can change in appearance over time. Atypical moles can change shape or color, grow in size, or begin to itch or bleed. It is important to conduct regular skin checks on yourself, paying attention to the appearance of various moles on your body. Suppose you notice that a mole is evolving and changes over time; make an appointment with a board-certified dermatologist for further assessment. While most atypical moles are non-cancerous, any changes in a mole’s appearance should be assessed.
What is the difference between atypical nevus and melanoma?
An atypical mole is a benign skin lesion with unusual clinical and histologic features. Atypical moles may resemble melanoma in many ways, appearing larger than normal moles, having irregular borders, and varying in color. There is no exact cause for the development of atypical nevi, though genetics and UV exposure likely play a role. While atypical nevi are not skin cancer, having atypical nevi puts you at an increased risk for malignant melanoma. Atypical nevi also have the potential to develop into skin cancer over time. Malignant transformation of atypical nevi may present as changes in size, color, or shape. Other common risk factors for melanoma include the presence of atypical moles and fair skin, light eyes/ hair, a family history of skin cancer, many moles or freckles, an inability to tan, and sunburn.
Melanoma is a form of skin cancer that accounts for approximately 1% of all skin cancers seen in dermatology and is the most deadly form of skin cancer. Cutaneous melanoma forms within damaged or mutated melanocytes and results in uncontrollable cell growth that can become metastatic and spread to other organs if not treated promptly. Most melanomas arise de novo, meaning they do not arise from a preexisting benign mole. High-risk factors for malignant melanoma include a family history of melanoma, first-degree relatives with melanoma, high-risk sun exposure, excessive tanning, sunburns, and chemical exposure. Although individuals with fair skin have a higher risk for melanoma, individuals of all skin types can develop melanoma. Early detection is essential in treating patients and in long-term survival. Melanoma risk should be assessed during your annual skin exam with the dermatologist. Dr. Green has found that most patients have no idea that they have skin cancer, and she encourages everyone who visits her office to have skin checks each year.
While atypical nevi and melanoma share some clinical and histologic features, a biopsy of a suspicious skin lesion can confirm diagnosis. Early detection and treatment of skin cancer significantly improves survival. Individuals with atypical nevi are generally at an increased risk for melanoma and should have regular skin checks with their dermatologist every six months. In between skin checks with a dermatologist, those with atypical moles should vigilantly perform self-examinations on a monthly basis to evaluate for new or changing skin lesions. Any new or evolving skin lesions should always be evaluated by a board-certified dermatologist, such as Dr. Green in NYC, to rule out skin cancer.
What is the difference between atypical moles and freckles?
There are unique differences between moles and freckles, which their appearances can distinguish. Freckles are superficial and are due to pigment changes in the superficial layer of the skin. Freckles are formed when the melanocytes, the cells responsible for producing melanin, absorb too much ultraviolet light, increasing melanin production and freckle formation. Atypical moles, or atypical nevi, are typically darker in appearance than freckles. Atypical moles are not superficial like freckles and look more like skin growths. Melanocytic nevi are typically more deeply pigmented, generally larger than freckles, and have more irregular features and abnormal cells. While freckles can be removed with various types of laser treatments and chemical peels, atypical nevi must be removed through excision, shave, or punch biopsy and sent to a lab for further assessment.
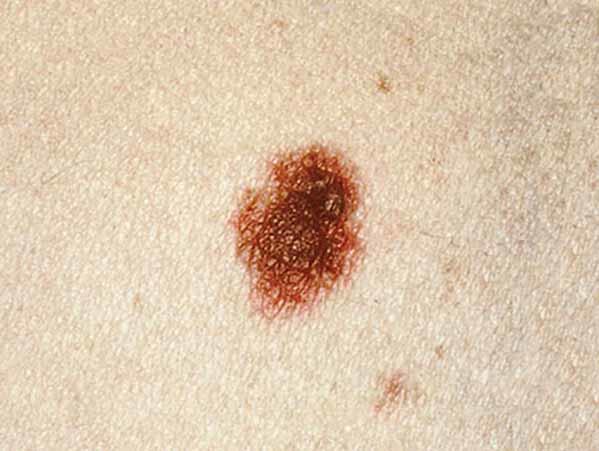
Source: Cancer.gov
What is an atypical spitz nevus?
An atypical spitz nevus is an uncommon, benign growth that shares similar visual characteristics with melanoma. While an atypical nevus is comprised of melanocytes, an atypical spitz nevus contains epithelioid or spindled cells. A spitz nevus can appear as red, pink, blue, brown, tan, or black and can be raised or flat. An atypical spitz nevus has various irregularities to its appearance, such as an irregular border or a mix of various colors. Atypical spitz nevi are very rare. Although atypical spitz nevi can look like melanoma, there is no need to cause alarm as these growths are not skin cancer. Most individuals with an atypical spitz nevus do not require any treatment. However, it is important to see a health care provider or dermatologist if you believe you may have an atypical spitz nevus to get an accurate diagnosis.
What is Familial Atypical Multiple Mole Melanoma Syndrome?
According to The American Academy of Dermatology (J am acad dermatol), Familial Atypical Multiple Mole Melanoma (FAMMM) is a genetic condition characterized by the presence of multiple melanocytic nevi, usually more than 50, and a family history of malignant melanoma. This syndrome is associated with mutations in the CDKN2A gene, and some patients have an increased risk of pancreatic cancer as well as other malignancies. Typically, one or more first or second-degree relatives (parent, sibling, child, etc.) have malignant melanoma and many moles, some of which are atypical. Patients suffering from this melanoma syndrome have an increased lifetime risk of developing melanoma and must be monitored closely with frequent self-examinations and in-person skin checks.
What is atypical mole syndrome?
Atypical mole syndrome or dysplastic nevus syndrome is characterized by an individual who has more than 100 moles, one or more moles that are 8 mm or larger in diameter, and one or more atypical moles. People who have ten or more atypical moles have a twelve times greater risk of developing malignant melanoma. Atypical moles are often found in individuals with a family history of atypia or degree relatives. In some studies, atypical moles and an increase in melanoma were seen in individuals experiencing hormonal changes, such as pregnancy or puberty. If you have atypical moles or a family history of atypical moles, you need to be especially vigilant in the surveillance of existing and new moles and proper follow-up. Consistent routine dermatology visits are the key to early detection, melanoma detection, and prevention.
What is atypical moles dysplastic nevi?
An atypical mole or dysplastic nevus is a benign, pigmented growth with irregular characteristics. A mole or nevus is a common growth that occurs due to a clumping of melanocytes, or cells that give rise to pigmentation, under the skin. Moles are referred to as atypical or dysplastic when they contain unusual cells in the tissue. An atypical or dysplastic mole can appear as flat or slightly raised, irregularly shaped with jagged or blurred edges, or as a mix of various colors, including red, pink, brown, tan, and black.
Are nevus cancerous?
There are many types of nevi, and not all of them are cancerous. A nevus is the medical term for a mole or a clump of melanocytes. A melanocytic nevus or common nevus is a normal, benign mole. A congenital nevus is a mole that has been present since birth – these moles are benign but are at risk of developing into melanoma, with an increased risk for congenital nevi larger than 8 mm. An atypical or dysplastic nevus is a mole that contains irregular features from a normal mole. While having multiple atypical nevi increases the risk of developing melanoma, not all atypical nevi result in cancer. If you are concerned that one or more of your moles may be cancerous, consult with a board-certified dermatologist such as Dr. Michele Green for a consultation. During your skin examination, Dr. Green will observe the visual characteristics of each mole to assess if a biopsy should be sent to a laboratory for further testing.
Are melanocytic nevus cancerous?
A regular melanocytic nevus is not cancerous. A melanocytic nevus refers to a common mole, which is comprised of a clustering of melanocytes in the skin. Melanocytic nevi are benign, pigmented lesions and warrant no treatment. Changes in the appearance of a melanocytic nevus can be due to irritation in the area or cellular changes in the mole itself. A dermatologist like Dr. Green in NYC should assess any melanocytic nevus that has changed in appearance.
Are atypical moles cancerous?
Not all atypical moles are cancerous. Atypical moles carry the same physical characteristics as melanoma, but they are benign. Having multiple atypical moles, however, does increase the risk of developing melanoma in the future. If you have atypical moles, your primary care provider or dermatologist may suggest performing monthly self-examinations to track your moles. In these self-examinations, you should look for any changes in the shape, color, size, or texture of your atypical moles – any changes should warrant further examination by a dermatologist to assess if the mole may be cancerous.
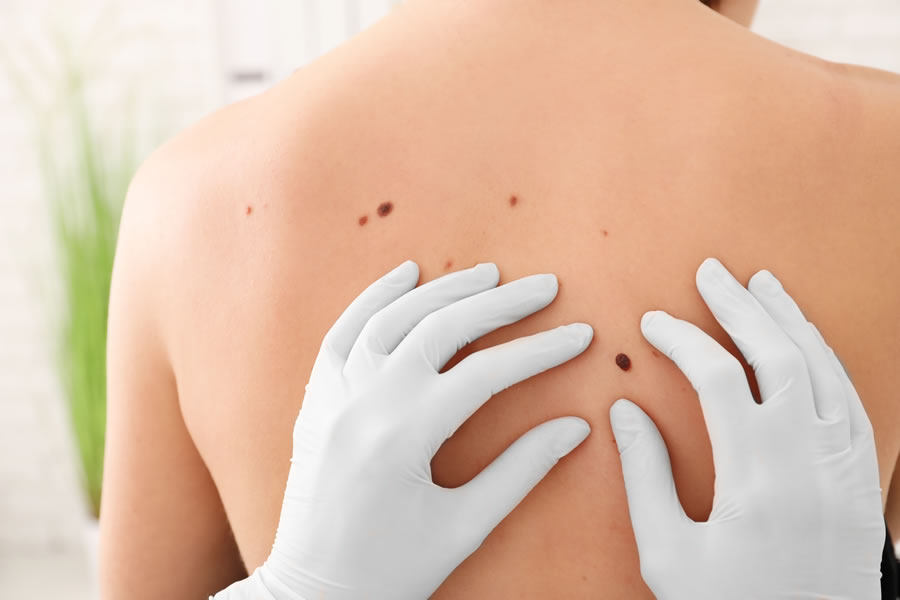
Can atypical moles grow?
Yes! Atypical moles can grow in size and change over time. An atypical mole can grow rapidly and become larger than the tip of a pencil eraser. If these changes occur, consult with a dermatologist for a skin examination. While most atypical moles are non-cancerous, changes in size or other physical characteristics could be indicative of a precancerous mole. A board-certified dermatologist such as Dr. Michele Green can take a biopsy of the mole and send it to a lab for an accurate diagnosis.
Why remove an atypical mole?
An atypical mole, while non-cancerous, has unusual clinical and histologic features that can cause it to develop into skin cancer in the future. Atypical moles have the potential to change over time in size, color, and shape, which may indicate malignant transformation. It is important to remove atypical moles before they develop in order to prevent malignant melanoma, the most serious type of skin cancer due to its invasive nature and lethality. This is especially important for individuals with atypical moles and a personal or family history of skin cancer, who are at a higher risk. Individuals with atypical nevi are generally at an increased risk for melanoma and should have regular skin checks with their dermatologist every six months. In between skin checks with a dermatologist, those with atypical nevi should vigilantly perform self-examinations on a monthly basis to evaluate for new or changing skin lesions. Early detection and treatment of melanoma is crucial for success. Any new or evolving skin lesions, including those that itch, bleed, ooze, or scale, should be evaluated by a board-certified dermatologist, such as Dr. Green in NYC. A quick and easy biopsy can confirm a diagnosis and keep you safe and healthy.
Skin cancer prevention, early detection, and self-examination
If you have a familial history of skin cancer or a diagnosis of a dysplastic or atypical nevus, you should limit your sun exposure and practice proper sun protection. You should limit your time outdoors, especially during the peak hours of 10 am and 4 pm when the rays of the sun are the strongest. When outside, wear protective clothing such as wide-brimmed hats, long-sleeve shirts, and long pants to minimize sun exposure. A broad-spectrum sunscreen with an SPF of 50 or higher should always be applied before going outdoors for maximum UVA and UVB protection. Sunscreen should be reapplied every two hours and reapplied after activities involving swimming and water sports.
According to the American Academy of Dermatology, yearly skin cancer examinations are extremely important to early melanoma detection. In her private Upper East Side dermatology office, Dr. Michele Green starts each consultation with a full-body skin exam and counsels every patient on sun avoidance and proper sun protection. In addition to frequent routine dermatology follow-up visits, you can also perform a self-examination at home. When doing a self-examination, examine your entire body, including your fingers and toes, to identify new growths or lesions as well as any changes in size, color, border, or shape of existing moles. It is also important to note that any existing lesion that does not heal quickly or is routinely irritated or itchy warrants further attention. If there is a new or changing mole that you are concerned with, please inform Dr. Green to evaluate these changes.
Where can you get your skin examined for melanoma and atypical moles?
An atypical nevus is a benign skin lesion with unusual features. Atypical nevi share some clinical and histologic characteristics with melanoma, making them difficult to distinguish. Melanoma is the most serious type of skin cancer due to its invasive nature and lethality. While atypical nevi aren’t cancerous, they have the potential to change over time and develop into skin cancer. Individuals with atypical moles are at a higher risk for malignant melanoma, and even more so if they have a personal or family history of skin cancer. Early detection and treatment of skin cancer significantly improves survival, meaning regular skin checks with a dermatologist and self-examinations between checks need to be a priority, especially for those with atypical moles. A dermatologist can biopsy an atypical mole to confirm a diagnosis. Any new or evolving skin lesions should always be evaluated by a board-certified dermatologist, such as Dr. Green in NYC, to rule out skin cancer.
Dr. Michele Green has over two and a half decades of experience performing skin examinations and biopsies to assess atypical nevi and other skin lesions and growths. Dr. Green is a world-renowned, board-certified dermatologist who employs the most innovative techniques for treating both medical and cosmetic conditions. She is consistently recognized by Castle Connolly, New York Magazine, Super Doctors, and The New York Times as one of NYC’s top dermatologists. When you consult with Dr. Green in her private Upper East Side dermatology office, she will work with you to develop an individualized treatment plan that best suits your particular skin concerns. To get started with atypical nevus assessment today, schedule a consultation with Dr. Green by contacting us online or calling the NYC-based office at 212-535-3088.
 212-535-3088
212-535-3088 



