Pregnancy Acne Treatment
Your body experiences many changes during pregnancy to support the development of a new baby. Along with these changes, side effects like acne can occur. While many people associate acne with adolescence, it can affect individuals of all ages, especially during pregnancy when hormone levels fluctuate. These hormonal shifts, especially the increase in progesterone, can cause your body to produce more sebum, which can clog pores and lead to breakouts. Acne is very common during pregnancy; more than half of pregnant women experience breakouts.
Additionally, if you had acne during adolescence, you’re at an increased risk of experiencing it again during pregnancy. Although acne can be frustrating, it should be treated carefully under proper medical guidance to ensure the safety of both you and your baby. With over 25 years of experience in medical and cosmetic dermatology, Dr. Michele Green is an expert in acne treatment and sees many pregnant patients at her private NYC dermatology practice for acne during pregnancy.
Acne blemishes can be frustrating and uncomfortable, making you feel self-conscious about your appearance. While many treatments for acne are common, managing acne during pregnancy can be especially difficult on your own. Some treatments, medications, and skincare ingredients are unsafe for the developing fetus and may increase the risk of birth defects. However, many effective acne treatments are safe to use while pregnant. It’s important to find an experienced dermatologist who can create a personalized treatment plan to address your hormonal acne safely. When you consult with Dr. Green, you can trust that your pregnancy acne treatment will be both safe and effective, helping you look and feel your best again.
Expert, board-certified dermatologist Dr. Michele Green has over 25 years of experience treating patients with acne at her private practice on the Upper East Side. Dr. Green has advanced cosmetic dermatology and cares for patients worldwide who struggle with acne and acne scars. She skillfully uses the latest technology and innovative treatments to deliver natural-looking, long-lasting results, helping her patients look and feel their best. Recognized for her dedication and expertise, Dr. Green is consistently named one of New York’s top dermatologists by Super Doctors, Castle Connolly, and New York Magazine. She values building strong relationships with her patients, taking the time to understand each person’s skin concerns and customizing treatment plans to meet their individual needs and goals. When you see Dr. Green, she will recommend a personalized combination of topical and oral medications, specially formulated skincare products, and in-office procedures to safely address your skin concerns and help you achieve clear, radiant skin.
What causes acne?
Acne is a skin condition, among other skin diseases, caused by various factors, including hormones, genetics, and the buildup of excess sebum and dirt in pores. During pregnancy, hormone levels often fluctuate, leading to increased sebum production. Sebum is a natural oil produced by sebaceous glands that helps keep skin moisturized and healthy. However, too much sebum, along with dead skin cells and bacteria, can lead to inflammation, redness, and discomfort. Changes in hormone levels and certain activities can stimulate the sebaceous glands, leading to clogged pores and acne lesions. Bacteria such as Propionibacterium acnes can infect clogged follicles, leading to inflammation. While many associate acne with adolescence, it can affect people of all ages. Acne can occur anywhere sebaceous glands are found, most commonly on the face, chest, and back. If untreated or poorly managed, acne may cause permanent scars or hyperpigmentation, which are often harder to treat than the initial breakout. If you are experiencing active breakouts, it’s important to see a board-certified dermatologist like Dr. Green promptly to prevent scarring and promote clear, glowing skin.
Types of Acne
Acne can appear in different forms, and recognizing these is important for effective treatment. Depending on the type of acne, you might need specific anti-inflammatory or antibiotic medications, which may not work for other types of lesions. Acne vulgaris lesions are divided into two main categories: non-inflammatory and inflammatory. Non-inflammatory lesions are mild and do not include pain, swelling, or infection. In contrast, inflammatory lesions range from moderate to severe and are characterized by pain, tenderness, and potential scarring. These inflammatory types can cause lasting skin damage, leading to scars. Non-inflammatory forms include comedones (blackheads and whiteheads), while inflammatory forms include papules, pustules, nodules, and cysts.
Non-inflammatory acne lesions
- Closed comedones, commonly called whiteheads, appear as skin-colored bumps resulting from clogged hair follicles, particularly the pilosebaceous units. The material within the pores remains beneath the skin surface and is not exposed to air.
- Open comedones, commonly called blackheads, are identified by clogged pores that have an opening at the skin’s surface. When exposed to air, the accumulated sebum, dead skin cells, and pore debris oxidize, giving them their distinctive black color.
Inflammatory acne lesions
- Papules are inflamed lesions that develop from blocked hair follicles. They appear as small, red bumps that can be tender to the touch.
- Pustules resemble papules but are distinguished by their pus content caused by a buildup of white blood cells. It’s crucial to avoid picking or popping pimples, as the pus can spread to other pores and cause additional infection.
- Nodules are acne lesions that develop when Propionibacterium acnes (P. acnes) bacteria become trapped beneath the skin, forming a hard, painful lump. Nodular acne carries a significant risk of scarring after infection.
- Cysts form when nodular acne fills with bacteria and pus. Like nodular acne, cystic acne penetrates deeply into the skin. It is considered the most severe type of acne because it can cause permanent tissue damage and scarring.
What causes acne during pregnancy?
During pregnancy, reproductive hormones like estrogen and progesterone increase significantly to support the developing baby and prepare the mother’s body for childbirth. While this process is natural, elevated hormone levels can influence acne development. Specifically, increased progesterone can stimulate sebaceous glands to produce more sebum, often called the “pregnancy glow.” Although this rise in sebum—a naturally occurring skin oil—may make some people appear more moisturized and plump, it can also clog pores and cause breakouts in others. When dealing with pregnancy acne, it’s best to consult a board-certified dermatologist to prevent worsening or scarring.
How do I prevent pregnancy acne from worsening?
To effectively prevent pregnancy acne from worsening, it is crucial to seek guidance from a board-certified dermatologist or healthcare provider. While numerous at-home and over-the-counter treatments are available, not all are safe or suitable during this time. Over-the-counter products that contain certain ingredients, such as salicylic acid or retinoids, may not be recommended during pregnancy, so professional guidance is essential. In addition to dermatological care, maintaining a consistent skincare routine, staying hydrated, eating a balanced diet, and managing stress can also help mitigate acne flare-ups during pregnancy. Dr. Green can provide tailored advice and help with acne treatment that is both effective and safe for you and your developing baby. This may include gentle cleansers, suitable topical medications, or lifestyle modifications.
How long does pregnancy acne last?
Pregnancy acne is a common skin concern that many expectant mothers face, and it usually persists for the duration of their pregnancy. Usually, pregnancy acne is most noticeable during the first trimester, when hormone levels rise rapidly and can impact skin health. However, some women may experience a resurgence of acne in the third trimester due to fluctuations in hormone levels again. The severity and duration of pregnancy acne can vary greatly from person to person. For some women, breakouts may continue intermittently throughout pregnancy, while others may notice their skin improving as they near the later stages. After childbirth, many women notice a significant improvement in their skin as hormone levels stabilize. In most cases, pregnancy acne clears up naturally within a few weeks to a few months after delivery, leaving skin healthier-looking.
How do dermatologists treat pregnancy acne?
When acne worsens during pregnancy, the first step is to speak with an experienced, board-certified dermatologist like Dr. Green in NYC. Treatment options may include topical acne medications and in-office procedures such as light therapy and acne surgery, depending on the severity of the breakout and the type of acne lesions. With over 25 years of experience, Dr. Green has helped many patients with pregnancy-related acne and will coordinate with your board-certified OB-GYN to develop a personalized and safe plan for your baby.
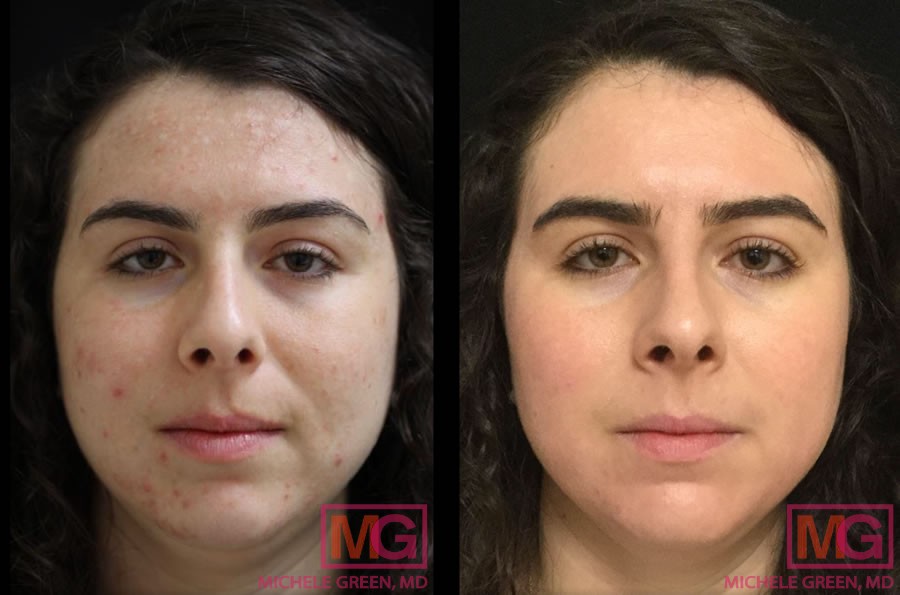
8 months before and after acne treatment
Pregnancy-Safe Acne Treatments
If you want to learn “What is the safest pregnancy acne treatment?”, the first step is to consult a board-certified dermatologist, such as Dr. Michele Green. With over 25 years of experience, Dr. Green specializes in prescribing safe and effective acne treatments for pregnant and breastfeeding women. The American College of Obstetricians and Gynecologists (ACOG) offers guidelines on the safety of various over-the-counter and prescription acne treatments. Using these guidelines, Dr. Green creates a personalized treatment plan for managing acne during pregnancy. Additionally, while some products are safe in small amounts, larger doses or prolonged use can be harmful to your baby. That’s why consulting with Dr. Green before using any acne products is essential. She will collaborate with your OB-GYN to develop a customized acne treatment plan tailored to your specific needs.
Topical Treatments
- Azelaic Acid — Because of its anti-inflammatory and antimicrobial properties, azelaic acid is a common ingredient in many topical acne treatments. It promotes cell turnover, encourages the growth of new skin cells, and fights bacteria that can infect hair follicles. As a result, it can reduce the symptoms of existing breakouts and help prevent future acne. Researchers have shown that azelaic acid is safe to use during pregnancy and does not harm the fetus.
- Topical Antibiotics — Clindamycin and erythromycin are among the most commonly prescribed topical antibiotics for treating acne during pregnancy. These antibiotics target and kill the bacteria responsible for infection in clogged pores. These ointments are best used as short-term spot treatments for active acne, as no research has documented the effects of long-term use.
- Glycolic acid — Glycolic acid is an alpha-hydroxy acid (AHA) that gently exfoliates the skin by removing excess oil, debris, and dead skin cells from clogged pores. According to the American College of Obstetricians and Gynecologists, glycolic acid products can be used during pregnancy. However, before using any glycolic acid, consult your dermatologist or obstetrician to ensure it is safe during pregnancy.
- Salicylic Acid — Salicylic acid is a beta-hydroxy acid (BHA) that functions as a chemical exfoliant to clear pores. As a BHA, salicylic acid loosens debris that clogs pores, making it easier to wash away. It is commonly found in over-the-counter acne treatment products. According to the American Academy of Dermatology (AAD), salicylic acid is generally regarded as safe when used in moderation. It is important to consult with a board-certified dermatologist or obstetrician before using products containing salicylic acid.
- Benzoyl peroxide — Benzoyl peroxide kills bacteria in papules and pustules and dries the skin to lower sebum production. It is included in many over-the-counter acne treatments, so always check the ingredient labels on your skincare products. According to the American Academy of Dermatology, benzoyl peroxide is considered safe when used in small amounts. However, it’s important to consult a board-certified dermatologist or obstetrician before using products that contain benzoyl peroxide.
Oral Treatments
A key question when managing acne during pregnancy is, “Can I use acne medication while pregnant?” and “Are antibiotics safe for pregnancy-related acne treatment?” If you have severe acne that does not respond to topical treatments, a short course of an oral antibiotic might be recommended. According to a review published in the Journal of American Family Medicine (doi: 10.3122/jabfm. 2016.02.150165), some oral antibiotics, like Erythromycin or Cephalexin, are generally considered safe during pregnancy. However, medications such as Tetracyclines, Streptomycin, and Kanamycin are not recommended because they may cause congenital disabilities. When using oral antibiotics for pregnancy-related acne, it is best to limit their use to a short duration to avoid potential side effects. Always consult your board-certified obstetrician and dermatologist to determine which antibiotics are safe for you during pregnancy.
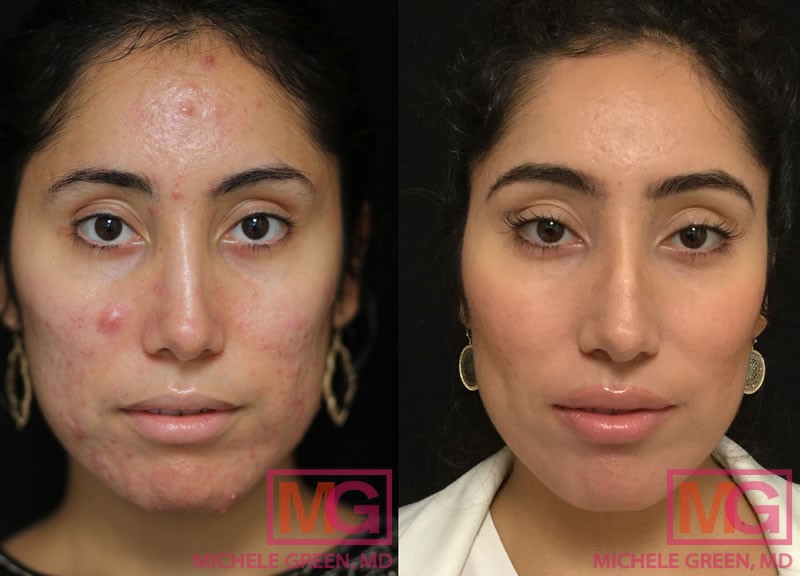
23 year old – Acne treatment, 3 months
In-office acne treatments that are safe during pregnancy.
Acne surgery
Some acne breakouts and cysts require a traditional removal method. For more severe acne, acne surgery may be an option. The procedure involves opening the pores and extracting dead skin cells, excess oil, debris, and other impurities trapped inside. This is followed by intralesional cortisone injections to reduce inflammation, accelerate healing, and help prevent acne scars. Acne surgery is most effective when combined with topical antibiotics to reduce the levels of bacteria that cause acne. Additionally, low-dose steroid solutions are often injected into the acne lesions to decrease inflammation and promote healing.
Acne Treatments that are not safe during pregnancy
Many common oral medications and Many common oral medications and skin care products for acne might not be safe to use during pregnancy or breastfeeding. Certain ingredients can enter your bloodstream and the baby’s, potentially leading to congenital disabilities. It is crucial to consult your obstetrician and a qualified dermatologist, like Dr. Michele Green, before starting any acne treatment, so you know which medications to avoid.
- Topical Retinoids – Topical retinoids, such as tretinoin (Retin-A), adapalene (Differin), and tazarotene (Tazorac), are commonly used to treat acne vulgaris; however, they are not recommended during pregnancy. Because they are derived from vitamin A, retinol treatments work by exfoliating the skin and reducing excess sebum, helping to clear hair follicles. According to the American Academy of Dermatology, when retinoids are absorbed through the skin and enter the fetal bloodstream, they can cause congenital disabilities, so they should be avoided during pregnancy and while breastfeeding. Other common brand names for topical tretinoin that are unsafe during pregnancy include Refissa, Renova, and Avita. Over-the-counter retinol products should also be avoided.
- Isotretinoin – Oral isotretinoin, commonly known as Accutane or by its brand names Absorica, Claravis, Zenatane, or Amnesteem, is an FDA-approved treatment for severe, cystic, or scarring acne. Like tretinoin, isotretinoin is derived from vitamin A and is used when antibiotics and topical creams have not effectively cleared acne. The federal government regulates this medication because of the serious congenital disabilities it can cause if taken. Conversely, pregnant women or those who become pregnant while using Accutane should not take it. Isotretinoin should never be used during pregnancy or while breastfeeding, as it can be harmful if absorbed into the fetal bloodstream.
- Spironolactone – Spironolactone, also known as Aldactone, is a medication that decreases the production of androgen hormones, which can make the skin oilier. While spironolactone effectively treats hormonal acne, it has been shown to cause congenital disabilities in a developing fetus. Therefore, it should not be used if you are pregnant.
- Oral Tetracycline – Tetracyclines are a class of antibiotics that are unsafe to use during pregnancy. Two commonly prescribed tetracyclines for moderate to severe acne are doxycycline and minocycline. Their anti-inflammatory properties usually help reduce acne breakouts. However, both have been linked to congenital disabilities such as inhibited bone growth and should not be taken during pregnancy.
The Best Skincare for Pregnancy Acne
The first step in any effective skincare routine is washing your face to remove dirt, debris, and sebum from the surface. Pregnant patients generally benefit most from a gentle cleanser that removes buildup without irritating the skin. Patients should avoid cleansers containing physical exfoliants, as harsh scrubbing can damage the skin’s natural moisture barrier and worsen acne breakouts. Dr. Green’s proprietary skincare line, MGSKINLABs, features a Gentle Cleanser that effectively removes excess sebum, dead skin cells, and impurities without irritating.
A good moisturizer is an essential part of any skincare routine, especially for pregnant individuals with acne-prone skin. Acne breakouts might actually worsen if you skip moisturizer, as dryness can weaken the skin’s natural protective barrier and worsen the acne. Many people with acne-prone skin prefer a lightweight, oil-free, non-comedogenic moisturizer that won’t clog pores. MGSKINLABs Ultimately Sheer Hydrating Lotion is an excellent choice for acne because it is rich in aloe and rosewater, providing instant hydration without feeling heavy or clogging pores. Additionally, the Ultimately Sheer Lotion has an improved pore-regulating formula that helps control oil production, reduce excess sebum, and leaves a matte finish.
Some patients might be tempted to skip sunscreen because it can feel greasy. However, sunscreen is essential in a skincare routine as it protects the skin from harmful UV rays and helps maintain the skin’s barrier. For those with oily or acne-prone skin, choosing a non-comedogenic sunscreen is best. Dr. Green’s MGSKINLABs offers a non-comedogenic, hydrating SPF 50 sunscreen that combines moisture and sun protection in one product. This type of sunscreen is perfect for keeping skin hydrated and radiant while shielding against UV rays that can lead to skin cancer and premature aging. When you meet with Dr. Green, you’ll have the opportunity to discuss a personalized skincare routine, including which products to include and which to avoid.

Acne treatment before and after
Can acne scars form after pregnancy acne?
Unfortunately, acne scars can develop from acne during pregnancy. Pregnancy acne often results from significant hormonal fluctuations that many women experience at this time. These hormonal changes can increase oil production in the skin, leading to cystic acne—deep, inflamed lesions that can be quite painful. Cystic acne is particularly known for causing scars because it affects the deeper layers of the skin. If these lesions are treated improperly or left untreated, they can damage the skin’s structure and leave permanent scars. This risk emphasizes the importance of early and effective treatment. To manage pregnancy acne and minimize scarring, it’s highly recommended to consult a board-certified dermatologist, Dr. Michele Green, who has years of experience treating acne. Dr. Green can provide personalized treatments that are safe for pregnant women, helping to reduce inflammation and promote healing while taking precautions to protect both mother and baby.
When should I see a dermatologist for pregnancy acne?
It’s advisable to see a dermatologist as soon as you notice the start of acne during pregnancy. Early treatment is essential, as untreated acne can lead to scarring that may be harder to treat than the acne itself. A board-certified dermatologist like Dr. Michele Green can offer personalized treatment options that consider both your skin health and your developing baby’s safety. By working with your board-certified OB-GYN, Dr. Green can create a comprehensive treatment plan that balances effective acne care with pregnancy precautions. This team approach ensures you get tailored solutions that minimize risk while effectively managing your skin concerns. Seeking medical advice promptly can help you control symptoms and keep your skin healthy throughout pregnancy.
Are there natural remedies for pregnancy acne?
Yes, there are many safe and effective natural remedies to help manage pregnancy-related acne, focusing on gentle skincare and dietary changes. It’s important to wash your face twice daily with a mild, fragrance-free cleanser. Look for products containing soothing ingredients like chamomile or aloe vera to help prevent irritation. Dietary adjustments are also key in managing acne. Incorporating zinc-rich foods like nuts, seeds, whole grains, and legumes into your diet can support skin health. Eating a balanced diet full of fruits and vegetables can further improve your overall skin condition. Although these remedies may offer relief, it’s always best to consult a board-certified dermatologist. When you see Dr. Green, she can evaluate your specific situation and recommend the most suitable treatments and lifestyle changes for effectively and safely managing pregnancy acne.
Other Pregnancy Acne Frequently Asked Questions (FAQs):
Can diet affect pregnancy acne?
Diet can significantly influence pregnancy acne, as certain food choices may cause inflammation and higher insulin levels, which can worsen hormone-related skin breakouts. During pregnancy, hormonal swings are the main cause of acne; however, nutrition also plays a crucial role in managing the severity and frequency of these skin issues. Research shows that diets high in sugar and refined carbs can trigger insulin spikes, a hormone that can boost androgen (male hormone) production, leading to increased skin oil. This excess oil can clog pores and promote acne. Additionally, some studies link dairy products to acne, possibly due to hormones in milk or their effects on insulin levels. To help reduce pregnancy acne, it’s beneficial to follow a balanced diet rich in low-glycemic, whole foods. Emphasizing fruits, vegetables, whole grains, legumes, and healthy fats can help keep blood sugar levels steady and lower inflammation. Staying well-hydrated by drinking plenty of water also supports skin health during pregnancy.
Can hormonal changes during pregnancy trigger acne?
Hormonal changes during pregnancy can indeed cause acne in many women. Throughout pregnancy, a woman’s body experiences significant hormonal fluctuations, especially increases in progesterone and estrogen. These changes can boost oil production in the skin as the sebaceous (oil) glands become more active. This excess oil can clog pores, creating an environment where bacteria can thrive, leading to breakouts and acne. Additionally, some women may notice heightened skin sensitivity during pregnancy, which can contribute to acne. Therefore, it’s common for expectant mothers to go through these skin changes during this transformative period.
When does acne start in pregnancy?
The severity and timing of outbreaks can differ among individuals. During the first trimester, significant hormonal changes happen. These fluctuations, especially in progesterone, can cause increased oil (sebum) production on the skin, which may clog pores and lead to acne breakouts. Women experiencing acne during the first trimester often notice breakouts around six weeks into pregnancy. Acne may improve for some women in the second trimester but can flare up again in the third trimester due to higher androgen levels, which boost sebum production. Regardless of when your pregnancy-related acne starts, Dr. Green offers a variety of safe and effective treatment options.
Is sulfur acne treatment safe in pregnancy?
Sulfur possesses antibacterial properties that can eliminate Propionibacterium acnes, a bacterium that causes acne. Sulfur also provides anti-inflammatory effects that help reduce redness and swelling, especially in pregnancy-related acne. It helps regulate oil production, which can be beneficial for those experiencing pregnancy acne, as oil production often increases during this time. Sulfur-based acne treatments have been used for decades without reports of adverse effects during pregnancy. Because of this, many dermatologists feel comfortable prescribing topical sulfur treatments, but it is best to consult with your board-certified OB-GYN before adding any new products to your routine.
Is pregnancy acne normal?
Yes, pregnancy acne is common among many expecting mothers, affecting over 50% of them. It occurs due to hormonal fluctuations that stimulate the sebaceous oil glands in your skin during pregnancy. This increase in breakouts is temporary and typically subsides once hormone levels stabilize, especially in the third trimester and postpartum. If you continue to experience acne after pregnancy, it’s best to consult a board-certified dermatologist, like Dr. Green, to find the most effective treatment for clear skin.
Which treatments and skin care can help with acne while pregnant?
Remember that pregnancy acne is temporary and caused by the increased androgens your body produces. Following a careful skincare routine or removing certain ingredients from your current regimen is crucial to managing pregnancy acne. It’s easy to start using ingredients that cause dryness or are too harsh, which can actually worsen irritation and breakouts as your skin produces even more oil to compensate. Safe and effective ingredients during pregnancy include azelaic acid, clindamycin, erythromycin, glycolic acid, benzoyl peroxide, and salicylic acid. HydraFacials and acne surgery, along with the right skincare routine, are also safe and effective for pregnancy-related acne, helping to clear dirt and debris from your pores. Navigating many over-the-counter and in-office cosmetic treatments can be overwhelming. Still, the key is to consult an experienced, board-certified dermatologist like Dr. Michele Green to develop a safe plan for you and your baby.
What makes pregnancy acne worse?
Acne during pregnancy often occurs due to increased sebum production triggered by hormonal changes. In addition to hormonal fluctuations, certain lifestyle habits can make acne worse. Patients who exercise and sweat frequently are more likely to develop acne during pregnancy. Sweat trapped under workout clothes can clog pores, trapping oil, dirt, and debris, and worsening existing acne or causing new spots. It’s important to remove dirty clothes and wash your skin right after exercising to help prevent acne. Patients who regularly use harsh physical exfoliants may see their acne worsen because these exfoliants strip the skin of its natural moisture barrier, leading to more sebum production. Some skincare products can be oily and clog pores, so choose products labeled as non-comedogenic, which are less likely to clog pores. Additionally, popping pimples can increase breakouts, as pus and bacteria from one lesion can spread and infect other clogged pores. If you’re experiencing pregnancy acne, it’s best to consult a board-certified dermatologist, such as Dr. Green, who has the knowledge and experience to treat your acne safely and effectively.
When will pregnancy acne clear?
The duration of Pregnancy acne varies among women; unfortunately, acne during pregnancy does not follow a fixed timeline. In early pregnancy, progesterone levels are high. Increased progesterone stimulates oil production, which can clog pores and cause acne. Many women find that their acne breakouts persist through the first and second trimesters, then clear up during the third trimester. However, some women experience acne throughout the entire pregnancy and see significant improvement after giving birth. Others continue to have persistent acne even while breastfeeding, with the acne finally clearing up several months postpartum. The duration of acne may be influenced by the ongoing hormonal changes during pregnancy and breastfeeding.
Is it safe to use chemical peels or facials during pregnancy?
Chemical peels vary widely in formulation and strength, with some ingredients posing greater risks than others. Stronger agents, especially those containing salicylic acid or trichloroacetic acid (TCA), can be absorbed into the bloodstream and potentially affect the developing fetus. Besides chemical peels, many facials include ingredients that may not be safe for pregnant women. Specifically, treatments with retinoids, which are used to combat acne and aging, have been linked to congenital disabilities. Therefore, avoiding these ingredients during pregnancy is essential. For safer options, pregnant women should opt for gentler facial treatments that focus on hydration and soothing effects. Simple facials involving manual techniques or mild, non-irritating products may be a better choice. However, it’s always best to consult a board-certified dermatologist, such as Dr. Michele Green, to ensure any skincare treatments are safe and beneficial for both mother and baby.
Which face wash is good for pregnancy acne?
The Mayo Clinic recommends using a gentle yet effective cleanser to remove dirt and debris from the pores without stripping the skin’s natural moisture barrier. Dr. Michele Green’s proprietary line of skincare products, MGSKINLABS Inc., offers a soothing Gentle Cleanser for Sensitive Skin that unclogs pores and cleanses without removing natural moisture. This lipid-free cleanser leaves a thin moisturizing film on the skin, making it ideal for people with sensitive skin.
Will pregnancy acne go away after giving birth?
Acne usually clears up within weeks after giving birth for most patients. However, some may experience ongoing acne flares postpartum as hormone levels continue to fluctuate. Postpartum acne is expected to improve once hormone fluctuations stabilize and hormone levels return to normal. Patients with persistent postpartum acne should see an experienced, board-certified dermatologist, such as Dr. Michele Green, who can recommend a safe and effective acne treatment plan tailored to their specific needs.
How to get rid of postpartum acne?
While postpartum acne often clears up on its own as hormone levels stabilize, certain treatments can help reduce acne and improve its appearance. After giving birth, hormone fluctuations during lactation can contribute to postpartum acne. Similar to pregnancy acne, there are restrictions on which medications can be safely used to treat it. HydraFacials, acne surgery, and targeted topical creams can decrease postpartum acne lesions while you are breastfeeding. If you are not breastfeeding, other treatment options can be considered. When seeking postpartum acne treatment, it is important to consult a board-certified dermatologist, such as Dr. Green, who can create a personalized treatment plan that is safe for both you and your baby.
How to start with pregnancy acne treatment today
During pregnancy, your body experiences many changes, including the development of acne. With so many acne treatments available, figuring out which options are safe and effective during pregnancy can feel overwhelming. Fortunately, a board-certified dermatologist like Dr. Green can guide you through your pregnancy acne treatment and offer expert advice on managing it. Dr. Michele Green in NYC will create a personalized plan that may include a combination of topical treatments, targeted skincare products, and in-office procedures such as HydraFacials and acne surgery, both of which are safe and effective during pregnancy. If you’re ready to clear your pregnancy-related acne and achieve smooth, clear skin, Dr. Green is here to help.
Dr. Michele Green, based in New York City, is a board-certified cosmetic dermatologist renowned worldwide for her holistic approach to treating active breakouts and residual acne scars. With over 25 years of experience, she has treated some of the most discerning men and women from around the globe. She has a special focus on helping pregnant patients who struggle with acne achieve a clear complexion. Dr. Green takes the time to understand each patient’s unique acne condition and creates customized treatment plans that address their specific skin concerns safely. Her dedication to her patients and her expertise are reflected in her consistent recognition as one of New York’s top dermatologists by Castle Connolly, Super Doctors, New York Magazine, and The New York Times. To start with a personalized acne treatment plan, please call Dr. Green’s NYC office at 212-535-3088 or contact us online today to schedule a consultation.
 212-535-3088
212-535-3088 




