Rash Treatment NYC & Types of Rashes
There are many different types of skin rashes in the field of dermatology. Some skin rashes can signify a serious underlying infection and need prompt attention. Dr. Michele Green is an expert in all aspects of rash treatments and specializes in their diagnosis and treatment. The art of dermatology lies in the identification and proper diagnosis of skin rashes. Many skin rashes look alike, but some skin conditions can signal an underlying systemic problem. Whether it be rosacea, eczema, shingles, ringworm, or a fungal infection, the proper diagnosis and correct treatment is critical to your health. There are many common skin rashes which are easily identifiable such as heat rash and a sunburn. However, since many rashes may appear similar, it takes an expert in dermatology to to differentiate between these different skin conditions. Dr. Green has been an expert in skin rash treatment and identification in her NYC private office for over two decades and is here to help.
What are the different types of skin rashes?
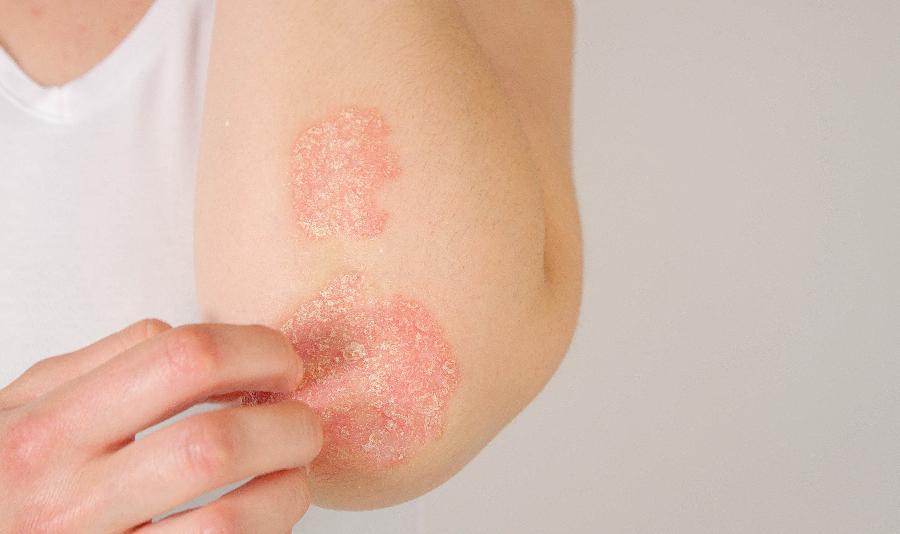
Many rashes appear alike initially, and present with red skin. Identifying which type of infection or disease process has caused this skin rash is the role of the dermatologist. The distribution of the rash is a clue to which skin disease is causing the eruption. Some of the most common skin rashes are:
- Poison ivy, Poison Sumac and Poison Oak
- Allergic reactions
- Contact dermatitis
- Atopic dermatitis
- Rosacea
- Viral infections like chicken pox
- Dry skin
- Tinea infections (fungal infections)
- Heat rash
- Scabies
- Diaper rash
- Bacterial infections
- Sun Burn
- Impetigo
- Lyme disease
- Cellulitis
Contact Dermatitis
Contact dermatitis occurs when the skin comes in contact with an irritant, which causes an allergic reaction in the skin. This allergic reaction manifests itself as a red pruritic eruption. There are many substances which can cause contact dermatitis; the exposure can result from a topical, material or environmental irritant. Contact dermatitis can come from direct contact with a variety of substances, or it can develop as an allergic reaction.
Direct, Irritant contact dermatitis is the most common of the two and occurs when the irritant causes damage to the skin’s protective barrier. This reaction can occur upon initial contact or gradually develop over time.
Common irritants include:
- Solvents
- Rubbing alcohol
- Bleach and detergents
- Shampoos, permanent wave solutions
- Airborne substances, such as sawdust or wool dust
- Plants
- Fertilizers and pesticides
Allergic contact dermatitis is different from direct contact dermatitis. Allergic contact dermatitis occurs when the substance triggers a response from the body’s immune system. This type of reaction can occur from physical contact with an allergen. The reaction to the allergen can occur immediately, within minutes, weeks, or even years after exposure, and usually affects only the area that came in contact with the allergen. One of the most common causes of a contact dermatitis is when you touch something that you are inadvertently allergic to, like in poison ivy. Initially, the body’s response to an allergic contact dermatitis may be red bumps and an itchy rash. Some weaker allergens can take years to trigger an immune response after exposure, as it takes time for the body to gradually build up enough of the irritant to cause the reaction. However, there can be more serious, life threatening reactions that cause difficulty breathing and need immediate medical attention. You should contact a health care provider right away if you start experiencing an allergic reaction to any allergen that causes difficulty breathing.
Common allergens include:
- Nickel
- Medications, such as antibiotics
- Hair dyes, deodorant
- Poison Ivy, Poison Oak and urushiol
- Ragweed and pesticides
- Photo allergic products or medications. These are substances which trigger an allergic reaction due to exposure to the sun.
Poison Ivy
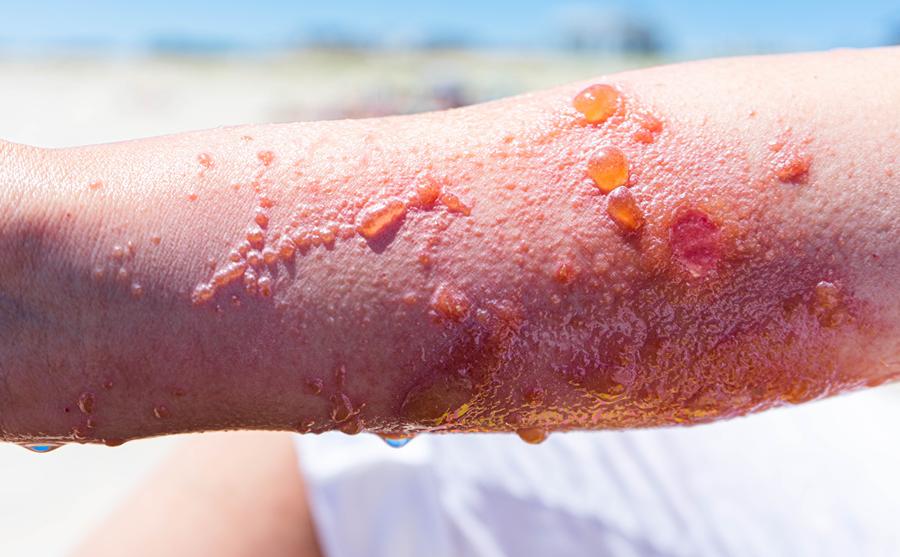
Poison Ivy, oak, or sumac can cause a red, itchy rash that often causes blisters. The rash is caused by the urushiol oil found in these plants. The itchy, blistering rash often begins 12 to 72 hours after one comes into contact with the oil.
The rash is not contagious to other people. When the rash seems to spread, this is often caused by a delayed sensitivity reaction. You can spread the oil on your skin after direct exposure by touching other parts of your body. Urushiol can stick to almost anything, including pet’s fur, gardening tools, or clothing. It is important to clean all surfaces and objects that may have the oil on it.
A poison ivy rash can be prevented after initial exposure if you wash the exposed skin immediately with lukewarm water and then soak the area. It is important to wash all clothing or objects that may have been exposed to urushiol oil. If a skin rash develops, topical and oral steroids are an effective treatment for poison ivy. Oatmeal baths, topical emollients, and antihistamines can also lessen symptoms.
Pityriasis Rosea
Pityriasis rosea is a skin rash that is often preceded by an upper respiratory tract infection. The first sign is typically known as a “herald” patch, which is a single 2-10cm ovular, red patch that typically appears on the abdomen. Several days after the original patch appears, multiple smaller, scaly, oval-shaped patches often appear on the abdomen or the back, and the rash can sometimes extend to the limbs. The spread of the rash is commonly referred to as a “Christmas-tree” distribution because of its characteristic outline. The initial rash varies from mild to intense itching. At times, the rash may be accompanied by low-grade fever, nausea, headache, and fatigue.
Pityriasis rosea is believed to be a viral infection, which is fought off naturally by the body’s immune system. Oral antihistamines, topical emollients, antibioitcs, and steroids can provide relief from the symptoms of Pityriasis rosea. Direct sunlight has also been shown to aid in the healing process.
Eczema
Eczema is a general term for an inflammation of the skin (dermatitis). The most common type of eczema is the form called atopic dermatitis. Atopic dermatitis is usually associated with hereditary conditions such as asthma and hay fever. Eczema affects about 10 to 20 percent of infants and about three percent of adults and children in the United States.
Many children outgrow eczema but, for others, it is a chronic condition that continues throughout adult life. The main symptom of eczema is pruritus or itchy skin, and there are times when a patient’s first symptom is itching without any obvious rash. Classic locations on the body for eczema are the face, back of ears, back of the knees, wrists, hands, or feet. Generally, you will see red bumps, or scaly red patches that can crust, turn brown, and become either hyperpigmented, with skin discoloration or hypopigmented as the eczema heals.
The precise cause of eczema is unknown, but it is believed to be linked to an overactive response by the body’s immune system to an irritant. Some forms of eczema can be triggered by substances that come in contact with the skin, such as soaps, cosmetics, clothing, detergents, jewelry, or sweat. Stress, as well changes of temperature or humidity, can also worsen eczema. Though unconfirmed, there may be a genetic component to eczema, as it is common for eczema to run in families.
There are different types of eczema ranging from atopic dermatitis, which is usually genetic and starts in childhood, to contact dermatitis, which is typically a reaction to an irritant such as nickel or poison ivy. Other forms of eczema include nummular eczema, which occurs in round coin-shaped areas, and dyshidrotic eczema, which appears predominantly on the hands and feet in the form of small cysts.
Treatment for eczema is based on alleviating symptoms and stopping the development of the disease. Topical skin care is the key to treating eczema, such as emollients, steroid creams, Elidel, and oral antihistamines, which are commonly prescribed. Daily use of moisturizers is one of the most important, yet simple treatments that needs constant maintenace. Taking oatmeal baths with warm water and avoiding hot showers typically helps to control eczema as well. Lifestyle modifications, to avoid triggers for the condition, may also be recommended. During your consultation, Dr. Green will evaluate your medical history, do a complete physical exam, and review your family history. A biopsy of the skin or skin allergy testing may also be advised to determine the correct diagnosis and treatment.
Heat Rash
Heat rash occurs during hot or humid weather. It develops when the pores become blocked, trapping sweat under the skin. The symptoms of a heat rash range from red bumps or blisters to a prickly rash or red lumps. Most heat rashes clear on their own but, in some instances, medical attention is required by a health care provider. Heat rash presents differently in adults than children. In children, the rash is predominantly found in the neck and abdomen, including the underarms. In adults, the rash can be seen in areas where the skin creases or where there is friction from clothing.
Different types of heat rash, or miliaria, are classified based on the degree of blockage within the sweat glands. Different miliaria variations include:
- Miliaria crystallina is the mildest form of heat rash where the top layer of the sweat glands are blocked. Symptoms include tiny bumps filled with clear fluid.
- Miliaria rubra, or prickly heat rash, includes red bumps which are very pruritic.
- Miliaria pustulosa includes pustular bumps which are red and itchy.
- Miliara profunda is the least common form of heat rash and occurs deeper within the layers of the skin. The blocked sweat glands cause sweat to leak into the skin, creating flesh-colored skin lesions.
Shingles
Shingles is a viral infection which can occur anywhere on the body. The shingles rash is caused by the same varicella virus which causes chicken pox. Shingles is, in short, reactivated chicken pox. Not everyone who has had chicken pox will develop shingles. Shingles is generally caused by extreme stress and fatigue, which makes the body more susceptible to infection. The virus can lie dormant in the body for years. The rash is usually painful and presents as a cluster of red blisters, along a specific dermatome, or patch of skin specific to a single spinal nerve.
The most common shingles symptom is a rash on one side of the body that is painful, sensitive to touch, and often accompanied by tingling and numbness. The rash also presents with blisters that forms a crust when they open. Some individuals also present with fatigue, fever and headache. Although singles can occur anywhere on the body, it is predominantly found on a single side of the body. Shingles can also present on the face and eyes. When Shingles presents on the face, it is extremely important to seek medical attention, as there is a risk for vision loss or blindness. Prompt medical treatment consists of oral antiviral therapy such as Valtrex, as well as topical wound care.
The CDC recommends individuals who are over the age of 50 and have had neither chicken pox nor shingles get vaccinated against the chicken pox and shingles. The FDA has approved Zostavax and Shingrix vaccine for shingles and Varivax and ProQuad for chicken pox. If you have had the chicken pox and have never been vaccinated for shingles, you may be advised to receive a Shingles vaccine.
Impetigo
Impetigo is a contagious bacterial infection which presents as a skin rash. Impetigo is very common skin infection and can appear anywhere on the body. However, it is primarily found on the face, hands and feet. Children commonly are susceptible to impetigo infections.
The rash appears as red bumps or lesions which ooze liquid, forming a yellow- brownish colored crust. The sores are contagious and can spread quickly to other parts of the body. There are two forms of impetigo. Bullous impetigo is the less severe form and presents with large skin blisters which mainly appear on the torso. Ecthyma, the more a severe form, extends deeper within the skin, causing fluid and pus filled skin sores which are painful and can turn into skin ulcers. Impetigo is not generally life-threatening but, without proper medical attention, the condition can worsen, causing other health complications such as:
- Cellulitis: This infection can spread to the lymph nodes and bloodstream becoming life threatening.
- Kidney issues: Group A Streptococcus, one of the types of bacteria which causes impetigo, can cause damage to the kidneys.
- Scarring: The large blister and skin ulcers caused by impetigo can leave scars.
Oral antibiotics are usually recommended to treat impetigo. In severe instances, intravenous antibiotics are sometimes needed to clear infection which has entered the bloodstream.
Scabies
Scabies is caused by the Sarcoptes scabiei mite. This mite cannot be seen with the naked eye; it burrows under the upper layer of the skin, laying its eggs and feeding on blood. Scabies rash is extremely itchy and causes discomfort due to bites. Anyone can be susceptible to scabies, as it is transmitted though skin to skin contact, as well as from clothing and bedding.
The mites, although not visible to the naked eye, can be seen under a microscope. A clinical diagnosis for scabies usually includes a skin biopsy for further evaluation by a pathologist under a microscope. Dermatologists are trained to identify scabies rash, which can consist of red bumps, blisters, and gray lines that can be seen along the surface of the skin. Many times, the burrows of the mite can be seen in between the fingers and feet, with with numerous excoriations on the body from this pruritic eruption.
A scabies rash can be very similar in appearance to those caused by poison ivy, dermatitis, and parasitic insects such as fleas. However, it is unique in that discomfort from the rash gets worse at night. Prompt treatment with anti-parasitic medication is essential to control the spread of the disease. Medication used to treat scabies include topical Kwell lotion, Elemite lotion, or oral ivermectin. It is important to remember that when a person first contracts scabies, there may be no symptoms for the first 4 to 8 weeks, but they are still contagious during this time. All contacts should be treated in the household as well anyone who may have come into physical contact with this person. It is also important to clean all bedding, clothing, and towels, used by the infested person to prevent the transmission of the mite.
Lichen Planus
Lichen Planus is a rash that can develop on the skin, tongue, scalp, and oral mucosa. The typical rash of lichen planus has been described as the “5Ps”: pruritic, planar, purple, polygonal papules. The rash is common around the wrist and ankles and persists for weeks, often turning blue-black or dark brown in discolored patches on the skin.
The eruption may appear as papules, pruritic bumps, blisters, or rarely, erosive sores in mucous membrane areas. The nails may be affected with ridging or grooves on the nails, leading to splitting, thinning or even loss of the nail. The scalp may also be affected with redness, irritation, patchy hair loss, or even scarring alopecia.
Lichen planus is most common in middle-aged adults. More women get lichen planus in their mouths than men. Lichen planus is believed to be caused by an autoimmune disease. Some cases of lichen planus have been found to be associated with hepatitis C virus infection.
Various medications are used to treat lichen planus including oral and topical steroids, retinoids, tacrolimus ointment, antihistamines, and ultraviolet light therapy. Many cases of lichen planus resolve within two years.
Lyme Disease
Lyme disease is a disease that develops due to a bite from an infected tick. A tick bite doesn’t necessarily mean you will contract Lyme disease, since it depends on what type of tick bit you and whether or not they were carrying the disease. Lyme disease can be life-altering, and the symptoms occur in stages depending on the severity.
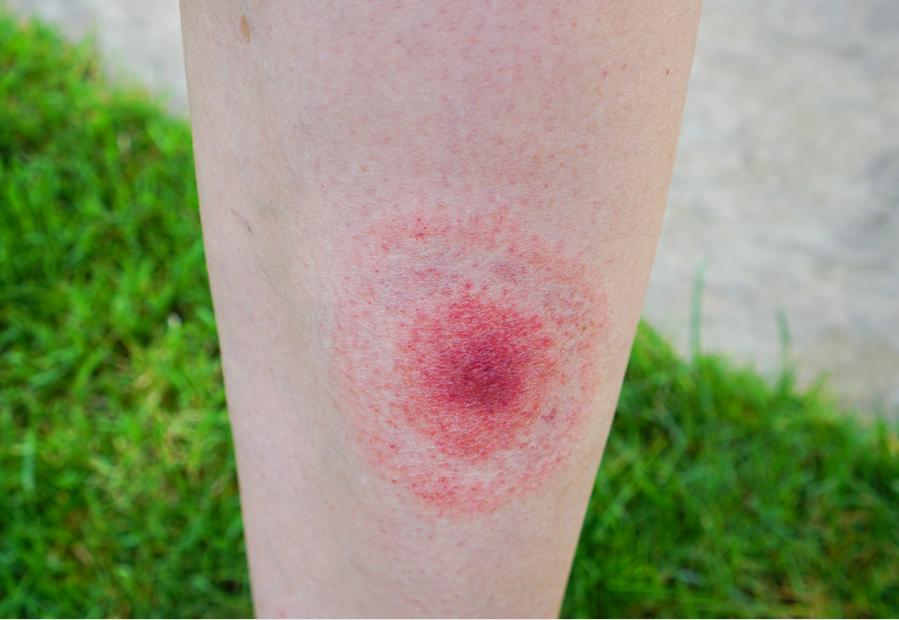
The initial sign that you have been infected is a annular red rash which looks like a bullseye at the site of the tick bite. Typically, a rash will develop and, within a few days of infection, other symptoms will occur, including fever, body aches, headache, chills, fatigue, neck stiffness, and swollen lymph nodes.
Other symptoms which evolve over time include Erythema migrans, a rash which presents all over the body. Individuals with Lyme disease can also present with joint pain, fatigue and neurological issues. Bouts of severe joint pain and swelling are especially likely to affect your knees, but the pain can shift from one joint to another.
Treatment of Lyme disease includes oral antibiotics such as doxycycline in a 14 to 21 day course. In severe cases intravenous antibiotics may be needed if the disease involves the central nervous system. Although intravenous treatment is successful in eliminating the infection, it can take weeks or months for all of the symptoms of Lyme disease to resolve.
Even after treatment, there are a subset of patients who still suffer from symptoms, such a muscle aches and fatigue. This condition has been called post-Lyme disease syndrome. Some researchers believe that the lyme infection triggers an autoimmune disease and can be treated with intravenous gamma globulins. More research is currently being done on Lyme disease and its treatment.
Scarlet Fever
Scarlet Fever is a a skin rash which often develops in individuals suffering from strep throat. Caused by the bacterium S. pyogenes, the same family of streptococcus which causes strep throat, scarlet fever can cause severe kidney damage among other life threatening issues. Before the existence of antibiotics, having scarlet fever was considered a death sentence, but thankfully today the illness can be readily treated. Scarlet Fever symptoms include:
- a red rash which looks like a sunburn
- flushed face
- “strawberry” tongue, which presents as swollen and bumpy
- fever of 101 F or higher
- chills
- difficulty swallowing
- enlarged lymph nodes
- nausea or vomiting
- headache
Dry Skin
Dry skin can often aggravate existing skin rashes. Water plays an important role in the proper functioning of your organs and bodily systems. When you are dehydrated, it can have a damaging effect on your body, including the acid mantle of the skin. By drinking sufficient amounts of water, you can prevent your skin from excessive drying. If you suffer from dry skin, skin rashes such as psoriasis and eczema can be exacerbated.
In order to protect against dry skin, you will need to moisturize frequently, using a thick moisturizer and paying special attention to the affected area. You should also avoid hot showers and use a humidifier. Your skin needs a moisturizer that both acts as a barrier on the skin to prevent moisture loss and keeps your cells hydrated. In extreme cases of dry skin, your dermatologist can prescribe topical steroid creams such as hydrocortisone cream to reduce redness and inflammation. Oral antihistamines such as Benadryl, Zyretc, or Claritin, may also be needed to help alleviate any pruritic symptoms associated with your dry skin.
Taking care of skin rashes at home
It is inadvisable to care for a rash at home without first seeking medical attention or the opinion of a dermatologist. In some incidence, rashes can lead to life threatening complications. The guidelines below can help to ease any discomfort associated with a rash while you are waiting for medical prognosis:
- Use mild non comedogenic skin cleanser to clean the area. You can also soak in an oatmeal bath. Oatmeal is an anti-pruritic treatment and will alleviate the itch.
- Use warm water compress to clean the area.
- With a clean washcloth gently, pat the area to keep it dry.
- Take an inventory of any new products, materials or environment you have been exposed to which may have triggered the rash.
- Use a non-comedogenic cream and a gentle skin wash if the area is excessively dry or flaking.
- Avoid the urge to scratch, as this can cause further irritation and infection.
- To further ease discomfort, to dry up any blisters from the rash, you can apply over-the-counter hydrocortisone cream and/or calamine lotion. Oral antihistamines such as Benadryl and Zyrtec can also reduce the severity of a reaction.
- If the rash is on your scalp, try using an anti-dandruff shampoo.
- For further pain and discomfort associated with your rash, you can try taking over-the-counter pain-reducers, such as ibuprofen or acetaminophen.
COVID-19 (Novel Coronavirus)
Though typically COVID-19 does not present as a skin rash, recent cases have presented with a few types of rashes. The rash of COVID-19 can present in various ways:
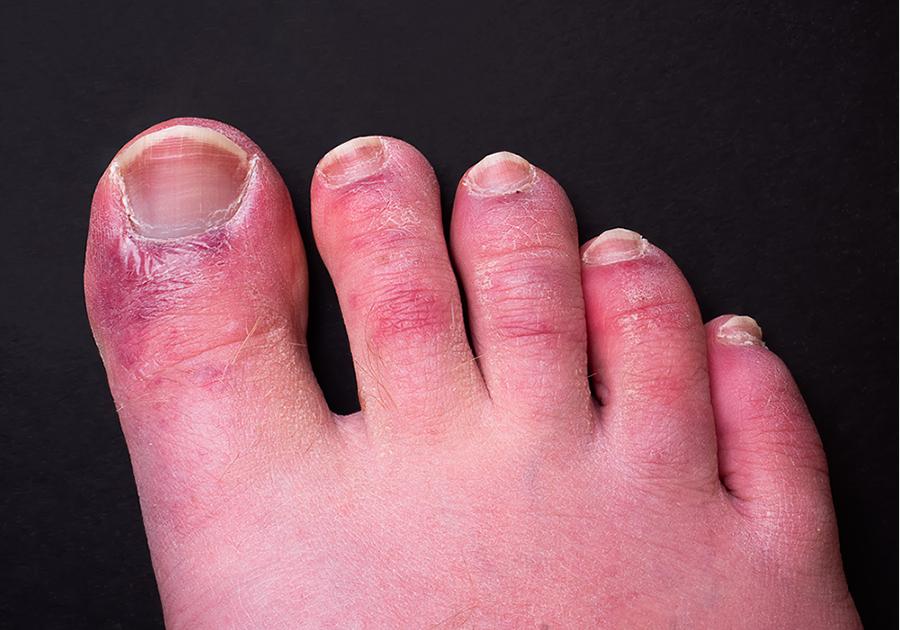
- It can present as a frostbite-like rash on the hands and feet, resembling chilblains and are painful. This eruption on the feet has been called “Covid toes”. This rash seems to be a later manifestation of the rash and lasts approximately 12 days and is seen in nine percent of cases.
- A hive-like rash which consists of small, elevated red or white patches on the skin, lasting approximately 7 days and found in the more severe cases of the disease. Close to 20 percent of COVID-19 cases present with this rash.
- A maculopapular rash which consists of small red patches and bumps on the skin, which tends to look like similar to other viral eruptions. This rash can sometimes be pruritic and is associated with more severe cases, with the eruption lasting around 9 days. Nearly half of the patients who present with COVID-19 rash have this type of skin eruption.
- An eruption of small uniformly shaped blisters on the arm and legs, which can present as one of the early symptoms of the virus. The rash is usually pruritic and lasts about 10 days. Nine percent of cases present with this rash, and is is more common in middle aged individuals.
- Livedo (necrosis) presents as a purplish skin eruption with a lace-like pattern. It is a sign of diminished circulation and more common in older patients who are very ill with the disease. This rash would portend a poor prognosis and was found in six percent of COVID-19 patients
- Enathem (oral rash) are small red spots or petechiae that occur in the mucous membranes.
If you have a new rash and need prompt and accurate diagnosis and treatment Contact Dr. Michele Green online today or call 212-535-3088. The rash may be a symptom of an underlying disease which needs immediate treatment. For further information about particular skin diseases you may visit the other pages on our web site.
 212-535-3088
212-535-3088 



