Melasma Treatment For Skin
Melasma is a common skin condition that causes brown or gray-brown patches darker than the surrounding skin, which are the main symptoms. The most often affected areas include the forehead, cheeks, upper lip, nose, and chin. While melasma isn’t harmful, these dark patches can be upsetting, frustrating, and cause self-consciousness. Fortunately, effective strategies are available for treating and managing melasma. A variety of in-office procedures, along with prescribed creams and specialized skincare products, can significantly improve the appearance of the skin. Additionally, certain lifestyle changes can help prevent the condition from worsening. For those seeking treatment, it is important to consult with a board-certified dermatologist, such as Dr. Michele Green in New York City. With their expertise, patients can explore personalized treatment options designed to restore a clear, radiant complexion and boost confidence.
Melasma is characterized by the overproduction of melanin, the pigment responsible for skin color, in the melanocytes — specialized cells that produce it. Although the exact cause of melasma remains unknown, several factors are recognized as potential triggers. These include frequent or prolonged exposure to sunlight, genetic predisposition, and hormonal fluctuations, especially those related to pregnancy or hormonal therapies, all of which can increase melanin production. Despite consistent daily sunscreen use, many people find that melasma can persist, making it seem almost unavoidable at times. There are many effective treatment options available to manage its appearance, including procedures like Cosmelan peels and Mesopeels, which exfoliate and rejuvenate the skin, as well as microneedling, which boosts collagen production and enhances skin texture. Additionally, VBeam laser therapy can target and reduce pigmentation, while specially formulated topical creams and skincare routines support overall skin health. If you’re frustrated by the appearance of melasma or other forms of hyperpigmentation, board-certified cosmetic dermatologist Dr. Michele Green is ready to help.
Dr. Michele Green, based in New York City, is an internationally renowned, board-certified cosmetic dermatologist with over 25 years of experience offering some of the world’s most discerning clients the best non-invasive treatments, including procedures to reduce melasma and hyperpigmentation. She takes a holistic approach and follows a less-is-more philosophy in facial rejuvenation, tailoring each patient’s treatment plan to their unique skin concerns and aesthetic goals. Dr. Green is consistently recognized by Castle Connolly, New York Magazine, the New York Times, and Super Doctors as one of NYC’s top dermatologists for her dedication and expertise. When you consult with Dr. Green at her private dermatology practice in Manhattan’s Upper East Side, she will work with you to develop a personalized melasma treatment plan and provide specific aftercare instructions to keep your complexion clear, bright, and radiant.
What is melasma?
Melasma is a common skin disorder characterized by blotchy brown, dark brown, or gray-brown patches that are darker than the surrounding skin. It most often affects the face, including the cheeks, nose, chin, upper lip, and forehead. Less frequently, melasma can also appear on other parts of the body, such as the chest, neck, arms, and back. It can be classified as epidermal, dermal, or mixed. In epidermal melasma, the pigment is confined to the top layer of the skin called the epidermis. In dermal melasma, the excess pigment is located in the dermis. Mixed melasma, the most common type, involves pigment in both the dermal and epidermal layers. In the past, dermatologists used a Wood’s lamp exam to evaluate the depth of pigmentation. Today, experienced board-certified dermatologists like Dr. Green can assess the treatment area clinically to diagnose and determine the specific type of melasma a patient has.
Melasma is a cosmetic skin condition and is not linked to skin cancer. Its appearance can cause frustration and low self-esteem. Although there is no cure for melasma, a specialist like Dr. Michele Green in NYC can help reduce its appearance using various skincare products, topical prescriptions, and in-office treatments. After treatment, avoiding sun exposure is especially important because it can trigger a recurrence of melasma. If you notice patches of hyperpigmentation that resemble melasma, consulting with Dr. Green in NYC is the best way to develop a personalized plan to lessen their appearance and attain clear, bright skin.

What causes melasma?
The exact cause of melasma remains unknown. Melasma is associated with melanin, the pigment that gives skin its color, produced by melanocytes, the skin cells responsible for melanin synthesis. When melanocytes are overstimulated, they cause melasma by creating uneven, darker patches on the skin. Although a specific cause has not yet been identified, certain factors can trigger or worsen melasma, including:
- Sun exposure — The most common cause of melasma is direct sunlight. Ultraviolet light, UVA, and UVB rays trigger melanocytes to produce more melanin. Even minimal sun exposure can cause melasma to return, even after treatment. Protecting your skin from UV rays is crucial to preventing melasma from returning after treatment.
- Tanning beds — Like direct sunlight, tanning beds emit harmful UV rays and visible light that can worsen skin pigmentation and increase the risk of skin cancer.
- Hormone fluctuations — Changes in hormones, particularly rising levels of estrogen and progesterone, have been linked to melasma development. Pregnancy, birth control pills, hormonal IUDs, and hormone replacement therapy can all trigger melasma since they influence estrogen and progesterone levels. Melasma is often called chloasma, or the “mask of pregnancy,” because it often appears on the faces of pregnant women.
- Genetics — Between one-third and one-half of people with melasma have a family history of the condition. Identical twins often share symptoms, and those with close relatives affected by melasma are more likely to develop it themselves.
- Skin Tone — Melasma is more common among individuals with light to medium brown skin color (Fitzpatrick skin types III and IV) and darker skin tones (types V and VI) than in those with fairer skin. People with darker skin are more susceptible because their skin contains a higher density of melanocytes, which enables them to produce more melanin.
- Oral Medications — Certain oral antibiotics, cardiac drugs, and other photosensitizing medications can trigger or worsen melasma. These include nonsteroidal anti-inflammatory drugs, antipsychotics, and antiseizure medications.
- Thyroid Disease — Currently, it is believed that thyroid disease may contribute to melasma in some patients, as many individuals with melasma also have thyroid conditions. Studies, including data from clinical trial observations, have shown elevated serum TSH, anti-thyroid peroxidase, and anti-thyroglobulin antibodies in patients with melasma. In fact, the prevalence of thyroid disease is 4 times higher in patients with melasma than in the general population.
- Stress — While research is ongoing, the stress hormone cortisol is believed to be associated with the development of melasma. Long-term stress can increase hormones involved in melanin (pigment) production. More research is needed to find the exact cause of melasma. Other factors, like pregnancy, thyroid disease, UV exposure, and certain medications, are more likely to trigger melasma.
Who is at risk for melasma?
Melasma is a skin condition that mainly affects women, with men making up only about 10% of those diagnosed (J Clin Aesthet Dermatol. 2018 Feb 1;11(2):53–59.). It is most common in individuals with light to medium brown skin tones (Fitzpatrick skin types III and IV) and in those with darker skin tones (Fitzpatrick skin types V and VI). People with darker skin are more vulnerable because they have a higher density of melanocytes, which increases melanin production. Several factors contribute to melasma, with hormonal changes being a key trigger. These changes can happen during pregnancy, while using hormonal contraceptives, or at different life stages that impact hormone levels.
Furthermore, prolonged exposure to ultraviolet (UV) light from the sun can worsen melasma symptoms, as UV rays stimulate melanin production in the skin, leading to dark patches. A genetic predisposition also plays a significant role, as individuals with a family history of melasma are at higher risk of developing it. Melasma usually appears as symmetrical brown or gray-brown patches on the face, especially on the cheeks, forehead, nose, and upper lip. These patches can become more noticeable after sun exposure and may vary in intensity depending on skin type and lifestyle choices.
What is melasma on the face?
Melasma mainly affects the upper lip, cheeks (often called the malar region), the bridge of the nose, and the forehead. Although the most visible signs of melasma are usually on the face, it can also appear on other sun-exposed parts of the body, such as the forearms and neck, in some people. The exact cause of melasma isn’t fully understood, but it is believed to be triggered by many factors, especially prolonged sun exposure. Ultraviolet (UV) rays activate melanocytes, the cells that produce skin pigment, leading to hyperpigmentation. As a result, melasma tends to worsen during the sunny, hot summer months when the skin is more exposed to sunlight, which can cause the patches to darken. Conversely, in winter, when sun exposure is less, these spots may fade and become less noticeable. Besides sun exposure, other factors like hormonal changes (commonly linked to pregnancy, oral contraceptives, or hormone replacement therapy), genetics, and certain skincare products can also contribute to the development of melasma.
Is melasma the same as hyperpigmentation?
Melasma is a type of hyperpigmentation characterized by dark brown or gray patches on the skin, most commonly on the face. Its key feature is that it often appears symmetrically, meaning the pigmented areas are found on both sides of the face with a similar pattern. Although the exact cause of melasma is not fully known, several factors can worsen the condition. These include excessive sun exposure, use of tanning beds, hormonal changes (common during pregnancy or with oral contraceptive use), certain medications, skin tone, genetics, and thyroid issues. Statistically, melasma occurs more often in women than in men. It is especially common among people with darker skin tones, such as those of Hispanic, African, and Asian descent, because they have a higher number of melanocytes—cells that produce melanin—in their skin. Melasma is a long-term condition that does not go away on its own; thus, treatment usually involves both professional in-office procedures and specialized skincare routines. While there is no cure yet, symptoms can be reduced with proper care. Most importantly, patients must follow strict sun protection measures, as neglecting them can lead to discoloration recurrence after treatment.
In contrast, hyperpigmentation is a broad term that encompasses any skin condition that causes discoloration darker than the surrounding skin. Besides melasma, other common types include sun spots, freckles, and post-inflammatory hyperpigmentation (PIH). Sun spots and freckles usually develop from prolonged sun exposure and excess melanin, forming small, pigmented patches that stand out against nearby skin. Unlike symptoms of melasma, which show symmetrical patterns, sun spots—also called age spots—may appear either in clusters or as single lesions and are typically asymmetrical. Age spots are more common in people with fair skin, while melasma mainly affects those with darker skin tones. Luckily, sun spots and freckles can be effectively treated with various non-invasive cosmetic procedures, such as chemical peels, laser therapy, and topical treatments. Post-inflammatory hyperpigmentation (PIH) is a specific type of darkening that occurs after skin inflammation from acne, injuries, eczema, or dermatitis, or as a side effect of improper laser treatments. PIH can fade over time, but it can also be successfully treated with a combination of in-office procedures and topical skincare aimed at skin rejuvenation and evening out skin tone. A key difference between melasma and other forms of hyperpigmentation lies in the treatment options available. For example, common laser treatments such as Fraxel, AlexTrivantage, and Intense Pulsed Light (IPL) often work well for sun spots and age spots, but should be avoided for melasma. This is because the heat from laser treatments can cause pigment to penetrate deeper into the skin, worsening the condition and making it harder to treat.
On the other hand, treatments like Cosmelan peels, Mesopeels, microneedling, and certain topical ingredients have proven more effective for melasma. Dr. Green, with over 25 years of specialized experience treating melasma, sun spots, and other types of hyperpigmentation across diverse skin tones, is well-equipped to accurately determine whether a patient’s discoloration is due to melasma, sun spots, or another form. During a simple physical exam, she can make accurate diagnoses. She also has extensive experience treating PIH related to acne or laser treatments, as well as other skin conditions like eczema or psoriasis. Her comprehensive approach helps patients achieve healthier skin and renewed confidence.

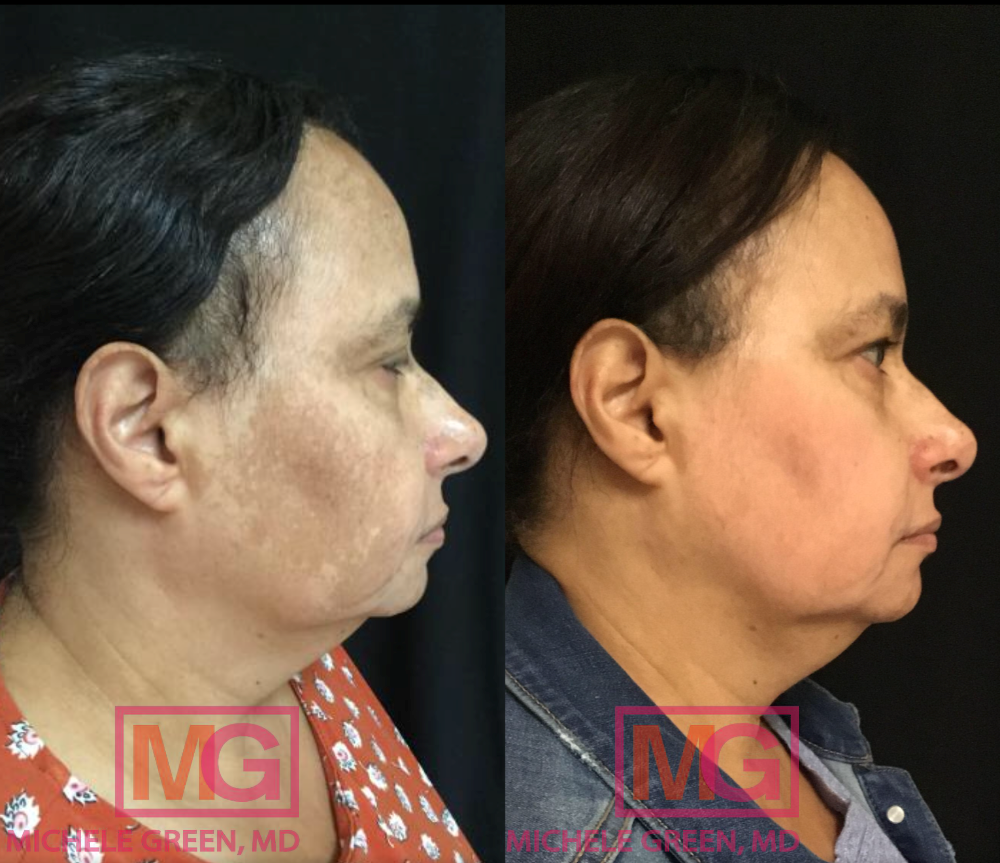
Cosmelan: 10 weeks before & after
Does melasma go away on its own?
The answer varies from person to person, mainly based on what initially caused the melasma. For those who develop melasma during pregnancy or because of taking oral birth control pills or other hormone-changing treatments, it may naturally fade after pregnancy or once the hormonal medications are stopped. However, for many people, melasma is a skin condition that needs cosmetic treatments to improve the appearance of dark patches. The treatment of melasma is an investment, and since it cannot be permanently cured with skincare alone or in-office procedures, prevention remains the best way to keep it under control. When working with Dr. Green to treat your melasma, she will give you all the necessary aftercare instructions to help you achieve and maintain a clear, healthy, and radiant complexion.
Can melasma be cured?
Many patients ask, “How do I get rid of melasma?” Melasma is notoriously hard to treat, as many common methods for dark spots, like laser procedures, can actually make symptoms worse. Since melasma can be very tough to manage, prevention is one of the most effective strategies. Preventive steps typically involve limiting sun exposure and stopping any medications or skincare products that may cause it. These approaches can help prevent melasma, dark spots, and other forms of hyperpigmentation. Dr. Green always recommends applying a daily broad-spectrum sunscreen with an SPF of 50 or higher. The best way to prevent unwanted pigmentation and signs of premature aging, and to reduce skin cancer risk, is to protect the skin from the sun’s harmful UV rays.
When unwanted melasma or hyperpigmentation appears on the skin, it can be effectively treated with targeted in-office procedures and specialized topical creams. According to melasma researcher AJ Pandya, the most effective treatment approach is a combination of various topical and in-office therapies. The best way to find out which combination is suitable for you is to schedule a consultation with a board-certified dermatologist, Dr. Michele Green. She will assess your melasma and skin to determine the most appropriate treatment options based on your skin type, skin tone, and the specific kind of melasma you have.
How to Treat Melasma
Chemical peels for melasma
A chemical peel is a skin resurfacing treatment that can enhance skin tone and texture. During a chemical peel, Dr. Green applies a chemical solution to the skin’s surface to gently and effectively remove discolored, dead skin from the outer layers of the epidermis. This chemical exfoliation promotes skin cell turnover, unclogs pores, and improves uneven skin tone, revealing a vibrant, healthy glow. Dr. Green can customize each chemical peel to suit her patients’ specific needs and goals. Depending on the strength and type of peel used, it can improve skin texture, reduce the appearance of acne breakouts or scars, and diminish sun damage, fine lines, wrinkles, and melasma. For patients with sun-damaged skin and pigment irregularities such as hyperpigmentation or melasma, Dr. Green often recommends a trichloroacetic acid (TCA) peel. However, TCA peels are not suitable for every skin type or tone, and it is important to consult with an expert, such as a board-certified dermatologist, to ensure the peel is safe and effective for you.
Cosmelan peel to remove melasma.
The Cosmelan peel is a two-step professional treatment used to target melasma and other types of hyperpigmentation. In the first step, Dr. Green applies the Cosmelan 1 mask to the affected areas. The mask remains on for several hours, with the exact duration determined by Dr. Green based on the severity of the pigmentation, skin tone, and skin type. The patient can easily remove the mask at home with a gentle facial cleanser. The second step involves applying specific topical products from the Cosmelan line, including a proprietary Cosmelan 2 depigmentation cream, a gentle moisturizer, and a tinted sunscreen. These products are used after the treatment to help maintain the results and prevent excess pigment from returning. The patient returns four weeks after the initial treatment for a re-evaluation and possibly a touch-up with Cosmelan if any hyperpigmentation remains.
Cosmelan causes an initial “peeling” effect, leaving the skin smooth and significantly reducing the appearance of facial hyperpigmentation. Dr. Green prefers Cosmelan because it is a simple, safe treatment with minimal downtime that delivers impressive results, helping patients look and feel their best. Cosmelan is safe and effective for all skin tones, including those with darker skin, which may not be suitable candidates for other chemical peels.
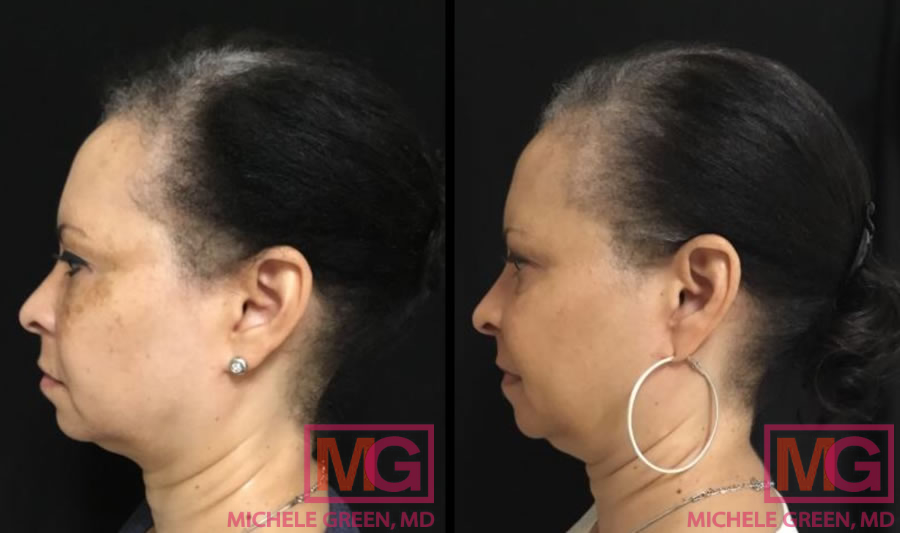
Cosmelan 11 months before and after
Mesopeels for Melasma
A Mesopeel is a specially formulated chemical peel designed to reduce and eliminate hyperpigmentation, including melasma, with minimal recovery time. Mesopeels use active skin-lightening ingredients such as tranexamic acid, kojic acid, and azelaic acid to decrease melanin levels, inhibit melanin production, and brighten the skin. They are very gentle and can be performed on patients of all skin types and tones. Additionally, they can be applied to the face and other areas of the body, such as the neck, chest, back, buttocks, and inner thighs. Patients typically need six treatment sessions to achieve optimal cosmetic results, while those with more severe melasma may require additional sessions.
Microneedling with depigmentation serum
Microneedling, also known as collagen induction therapy, is a safe and effective way to improve skin tone and texture. It can also help reduce the appearance of melasma, especially when used with a specially formulated depigmenting serum. This minimally invasive cosmetic treatment involves a practitioner using a handheld device with tiny, sterile microneedles to create controlled trauma on the skin’s surface. The procedure triggers the skin’s natural healing process and speeds up skin cell turnover, leading to a smoother texture and a brighter, more even tone. One benefit of microneedling is that it forms microchannels that enhance the skin’s ability to absorb topical solutions. For melasma, Dr. Green applies a proprietary depigmentation serum rich in skin-lightening and brightening agents to decrease hyperpigmentation and clarify the skin. Most patients need a short series of 3-6 sessions, spaced about 1 month apart, to achieve optimal skin rejuvenation results. Patients value the minimal downtime and mild side effects, which typically include redness and swelling in the treated area.
VBeam laser to treat melasma
The VBeam laser is a pulsed dye laser designed to target red pigmentation on the skin, such as facial redness, rosacea, broken capillaries, spider veins, red acne scars, and red stretch marks. It is also very effective at reducing redness and inflammation associated with melasma and post-inflammatory hyperpigmentation. This laser emits 595nm light to eliminate red pigments in the skin. During treatment, the surrounding skin remains unaffected, resulting in no downtime. Usually, 4 to 6 laser sessions, spaced one month apart, are recommended for the best results.
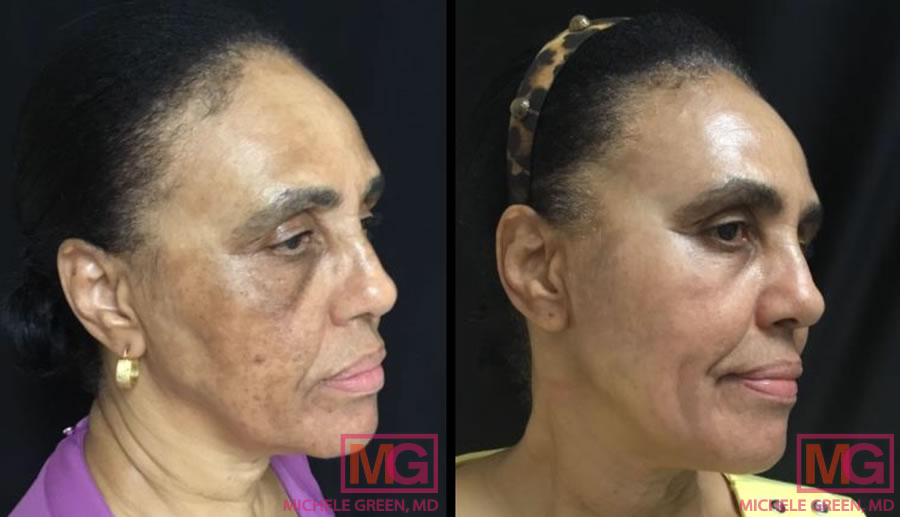
Cosmelan 8 months before and after
What is the best treatment for melasma?
According to the American Academy of Dermatology, there is no one best way to treat melasma. It is highly recommended to start by consulting an experienced, board-certified dermatologist, such as Dr. Michele Green in NYC. Melasma is a complex skin condition, and many traditional treatments for other types of hyperpigmentation, such as certain laser procedures, can worsen its appearance or make it harder to treat. Some of the most effective in-office options for melasma include chemical peels, Cosmelan peels, Mesopeels, microneedling with depigmenting serum, and VBeam laser treatments. Skin-lightening topical treatments and skincare products may also be recommended, especially those containing active ingredients like vitamin C, hydroquinone, azelaic acid, kojic acid, or tretinoin. Usually, patients see the best skin rejuvenation results with a personalized mix of topical therapies and in-office treatments. Dr. Green will work with you to develop a tailored treatment plan that targets your specific concerns and aesthetic goals, helping you look and feel your best. The most effective way to treat melasma at home is to limit sun exposure and follow a targeted skincare routine. Sun exposure is the main trigger for worsening melasma symptoms because UV rays stimulate melanin production in the skin. Using a broad-spectrum SPF 50 and wearing sun-protective clothing, like a wide-brimmed hat and sunglasses, can help reduce melasma dark spots and lower the risk of recurrence after treatment. A good skincare routine for melasma includes products with active skin-lightening ingredients such as vitamin C, tranexamic acid, kojic acid, azelaic acid, niacinamide, and glycolic acid. Prescription hydroquinone or retinoids can also be used at home to lighten pigmentation further and achieve a more even skin tone.
Which oral medications can help treat melasma?
Treating melasma can be a long process, and relying only on topical treatments may not work for everyone. For those having trouble managing melasma with topicals alone, an oral medication called tranexamic acid can be added as a supplement. Tranexamic acid is often used topically for melasma and taken orally by women with heavy or painful periods. Current research suggests that off-label oral tranexamic acid may be effective in treating melasma by inhibiting melanocyte activity, reducing excess melanin production, and preventing melanin transfer to skin cells. When used with topical treatments, oral tranexamic acid may help reduce the appearance of melasma and promote a clearer, more even skin tone. If you’re interested in whether oral tranexamic acid is right for your melasma, schedule a consultation with board-certified cosmetic dermatologist Dr. Michele Green.
Can sun exposure worsen melasma?
Sun exposure is a key factor that can worsen melasma, a condition marked by dark, discolored patches on the skin. Ultraviolet (UV) radiation from the sun can activate melanocyte cells, which produce melanin, leading to increased pigmentation. Without proper sun protection, such as broad-spectrum sunscreen or protective clothing, people with melasma risk worsening their condition. Extended sun exposure can stimulate melanin production in sensitive areas, resulting in more stubborn, darker spots. Therefore, it is important to consistently use sun protection to manage melasma and prevent further pigmentation issues.
Can laser treatments remove melasma?
No lasers should be used to treat melasma. While Fraxel and IPL lasers can reduce sun spots, age spots, and other forms of hyperpigmentation, they may worsen melasma pigmentation. Unwanted side effects from improper laser treatments for melasma include increased hyperpigmentation, burns, and scarring. Once laser treatment has been performed, melasma can become even harder to remove. Dr. Green uses Cosmelan peels, Mesopeels, chemical peels, VBeam laser treatment, and microneedling to prevent the condition from worsening. Treating melasma is difficult, and no single treatment is ideal for every patient or skin type. During your initial consultation, Dr. Green will examine the area and create a personalized plan that is safe and effective for your skin.
What is the best cream for melasma treatment?
A proper skincare routine is essential for patients with melasma to improve treatment outcomes. Topical skincare products are also crucial to prevent melasma from returning after treatment. Dr. Green created a proprietary skincare line, MGSKINLABs Inc., with specially formulated products to target various skin concerns, including melasma. When consulting with Dr. Green, she will design a personalized skincare routine that combines prescription and topical treatments to reduce dark patches and help achieve a clear, radiant, and long-lasting complexion.
Hydroquinone is an ingredient in prescription skin-bleaching creams that helps lighten hyperpigmentation and melasma. Its skin-brightening effects come from disrupting melanocytes, the skin cells that produce melanin or pigment. Hydroquinone should not be used long-term and should only be applied under the supervision of a board-certified dermatologist, such as Dr. Green. Overuse or improper use can cause skin irritation and worsen melasma. Additionally, hydroquinone increases the skin’s sensitivity to sunlight, so consistent sun protection is essential while using it.
Retinol and retinoids can be effective skincare ingredients for people with melasma. These vitamin A derivatives work by increasing skin cell turnover, stimulating collagen production, and exfoliating dead, discolored skin cells to reveal healthier, new skin. With consistent use over time, noticeable improvements in skin tone and texture can be seen. Tretinoin is a potent vitamin A derivative that is not available over the counter and must be prescribed by a healthcare professional. Retinols are available without a prescription and tend to be less irritating than prescription-strength retinoids. The Essential Antioxidant Infusion from MGSKINLABs features a unique blend of vitamin A and other nourishing vitamins and minerals to rejuvenate the skin and reduce pigmentation. Patients with sensitive skin may find retinol or tretinoin irritating, potentially causing redness, flaking, stinging, dermatitis, or worsening hyperpigmentation. These patients can use a short course of topical corticosteroids to reduce inflammation and prevent the worsening of melasma.
Vitamin C is a powerful antioxidant with many renewal properties, making it a valuable part of any melasma skincare routine. In addition to improving overall skin tone and texture by promoting collagen production and skin cell growth, vitamin C also prevents melanin production by blocking the enzyme tyrosinase. Dr. Green’s MGSKINLABs Vitamin C formula, the Vita-C Serum, contains a high concentration of vitamin C and is designed to encourage skin cell renewal and collagen synthesis, resulting in reduced hyperpigmentation and a clearer, healthier complexion.
Other effective skin lightening agents include kojic acid, azelaic acid, and tranexamic acid, which work by decreasing tyrosinase activity and inhibiting melanin production. The Skin Brightening Cream from MGSKINLABs features a unique blend of kojic acid and fruit extracts to reduce hyperpigmentation and promote a more even skin tone.
What is the best sun protection for melasma?
While in-office treatments and topical skincare products can help treat and manage melasma, nothing is more effective than sun protection. Patients with melasma should avoid sun exposure, as UV rays can trigger or worsen it and lead to recurrence after treatment. Many melasma treatments also increase skin photosensitivity, and UV exposure during this time can worsen existing melasma. Therefore, patients must always wear a broad-spectrum sunscreen that guards against both UVA and UVB rays, which can stimulate melanocytes to produce melanin. Dr. Green’s own Hydrating SPF 50, from her MGSKINLABs Inc. line, offers broad-spectrum coverage with a smooth, silky finish to ensure sun protection and comfort. Sunscreen should be worn daily, as UV rays can penetrate clouds and windows and reflect off puddles and snow.
For optimal protection, Dr. Green recommends using both chemical and physical sunscreens. Chemical sunscreens work by absorbing heat energy from the sun’s rays and reacting chemically within the skin. Physical sunscreens typically contain ingredients like zinc oxide, iron oxide, or titanium dioxide, and they function by sitting on the skin’s surface to form a barrier against strong UV rays. By layering these two types of sunscreens, you can better protect your skin from the sun and help prevent the development or worsening of melasma. Wearing a wide-brimmed hat, large sunglasses, and sun-protective clothing is also an effective way to enhance your sun protection and prevent melasma from worsening or returning.
Is melasma permanent?
The severity and duration of melasma vary from person to person. Patients who develop melasma during pregnancy or due to birth control pills, hormonal IUDs, or hormone replacement therapy may see their skin return to normal after giving birth or stopping hormone medications. However, for many people, melasma is a persistent condition that won’t go away without some type of cosmetic treatment. It’s important to note that certain laser therapies, such as Fraxel, IPL, and Picosure, can sometimes worsen the condition by pushing pigment deeper into the skin, making future treatments more difficult. If you see brown or gray patches on your face, it’s crucial to consult a specialist such as a board-certified dermatologist like Dr. Michele Green in New York City. Dr. Green can provide a comprehensive evaluation and develop a customized treatment plan with you. This personalized approach aims not just to treat melasma effectively but also to help you achieve a clear, radiant, and evenly toned complexion for long-lasting results.
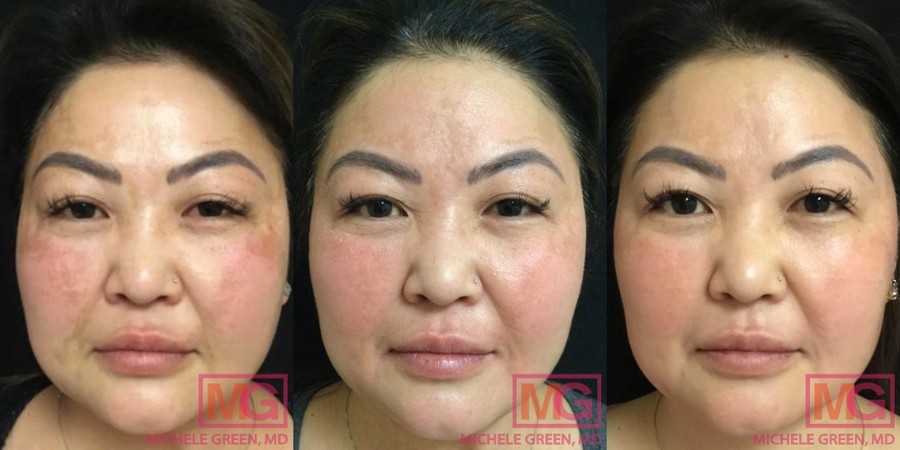
Cosmelan 6 weeks before and after
Frequently Asked Questions (FAQs) About Melasma:
Is melasma dangerous?
No, melasma is not dangerous. It is not a sign of skin cancer, nor does it have the potential to develop into skin cancer or any other harmful skin condition. However, some skin cancers can resemble melasma in certain ways. If you are worried about a brown or dark lesion on your skin and are unsure whether it is a sign of skin cancer or melasma, schedule an appointment with a board-certified dermatologist, such as Dr. Green. During your appointment, Dr. Green will thoroughly review your medical and family history and then clinically evaluate the hyperpigmented areas to rule out serious skin conditions. A skin biopsy may be performed and sent to the lab for further examination as part of a routine check to rule out melanoma and other types of skin cancer, if necessary.
Will melasma go away after pregnancy?
Pregnancy can cause a skin condition called chloasma, commonly known as “the mask of pregnancy.” This condition appears as dark, discolored patches on the face, especially the cheeks, forehead, upper lip, and chin. It is mainly caused by hormonal changes, particularly increased levels of estrogen and progesterone during pregnancy. Many women develop this pigmentation, but it usually resolves on its own within a few months to a year after childbirth, as hormone levels return to normal. To manage melasma during pregnancy, it is advised to use a broad-spectrum sunscreen with SPF 50 and limit sun exposure, since many standard treatments are not safe during this time. For women who find that melasma persists after pregnancy, consulting a board-certified dermatologist, such as Dr. Green, can offer safe and effective treatment options. With over 25 years of experience, Dr. Green customizes treatment plans for each case of melasma, helping women find relief from this common and often frustrating skin condition.
Can birth control cause melasma?
Hormonal birth control can contribute to the development or worsening of melasma, a skin condition marked by dark, discolored patches. This happens due to overproduction of melanin, the pigment that gives skin its color. The main hormones involved are estrogen and progesterone, which are present in various forms of hormonal contraceptives such as birth control pills, patches, and rings. These hormones can stimulate melanocytes—cells responsible for melanin production—causing increased pigmentation in sun-exposed areas of the skin. Studies show that up to 25% of women using oral contraceptives may experience some type of hyperpigmentation as a side effect. Factors such as sun exposure, skin type, and a personal or family history of melasma can also increase the risk. Therefore, women considering or currently using hormonal birth control should consult a healthcare professional about potential side effects, including melasma, and discuss preventive measures like using sunscreen and following proper skin care routines to reduce the risk.
What treatments should be avoided with melasma?
When treating melasma, it’s important to be cautious about the treatments you choose, as some can worsen the condition rather than improve it. Specifically, certain laser procedures effective for other types of hyperpigmentation—such as sun spots and age spots—should be avoided. For example, lasers like Fraxel and Intense Pulsed Light (IPL) therapy may help with various pigmentation issues; however, they can unintentionally push melasma deeper into the skin. This not only makes the melasma more noticeable but can also complicate future treatments. While some practitioners might recommend specific laser treatments for melasma, it’s important to understand that results vary greatly and these methods may not be the safest for everyone. Instead, there are more reliable and proven options. Chemical peels, which involve applying a solution to exfoliate the skin and encourage renewal, can effectively lighten melasma without risking further pigment deepening. Similarly, microneedling—a procedure that creates tiny injuries in the skin to stimulate collagen production—has also been shown to be a safe and effective way to treat melasma.
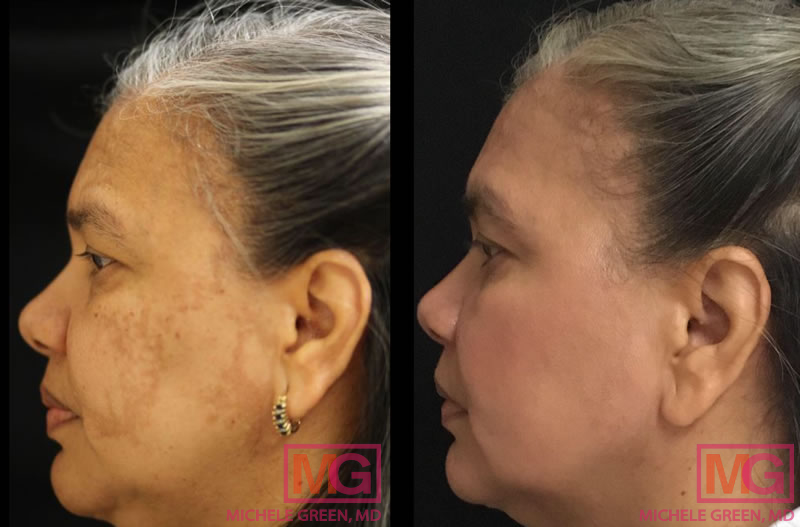
Cosmelan 1 year before and after
How do I get started with treating my melasma today?
Melasma is a complex skin condition that can pose significant challenges for those seeking effective treatment and reduction options. This condition, marked by dark, discolored patches usually on the face, can be resistant to treatment with only over-the-counter skincare products aimed at dark spots. Some of the most effective cosmetic treatments for melasma include Cosmelan peels and Mesopeels, both designed to exfoliate and renew the skin while gently addressing hyperpigmentation. Additionally, microneedling is another option that boosts collagen production and improves skin texture and tone, making it a good choice for many individuals with melasma. These advanced treatments not only offer safe and effective solutions but also typically involve minimal downtime and few, if any, side effects. Dr. Green’s expertise extends beyond melasma to include other forms of hyperpigmentation, such as post-inflammatory hyperpigmentation, sun spots, and sun-damaged skin. With her guidance, you can explore the most effective options to tackle your specific skin concerns, leading to clearer, more radiant skin. If you’re dealing with melasma or related pigmentation issues, Dr. Green is dedicated to helping you find the right solution.
Dr. Green is a highly acclaimed, board-certified cosmetic dermatologist with more than 25 years of experience providing top treatments to some of the world’s most selective clients, including those seeking to reduce hyperpigmentation and melasma. She takes a holistic approach and follows a less-is-more philosophy for facial rejuvenation, tailoring each patient’s treatment plan to meet their unique needs and aesthetic goals. Dr. Michele Green is often recognized by the New York Times, New York Magazine, Super Doctors, and Castle Connolly as one of NYC’s leading dermatologists for her dedication and expertise. When you consult with Dr. Green at her private dermatology practice in Manhattan’s Upper East Side, she will collaborate with you to develop a personalized treatment plan designed to achieve a clear, radiant complexion that lasts. To schedule a consultation with Dr. Green and learn more about the causes of melasma and the best treatment options, please contact us online today or call our New York City-based dermatology office at 212-535-3088.
 212-535-3088
212-535-3088