Acne Vulgaris Treatment
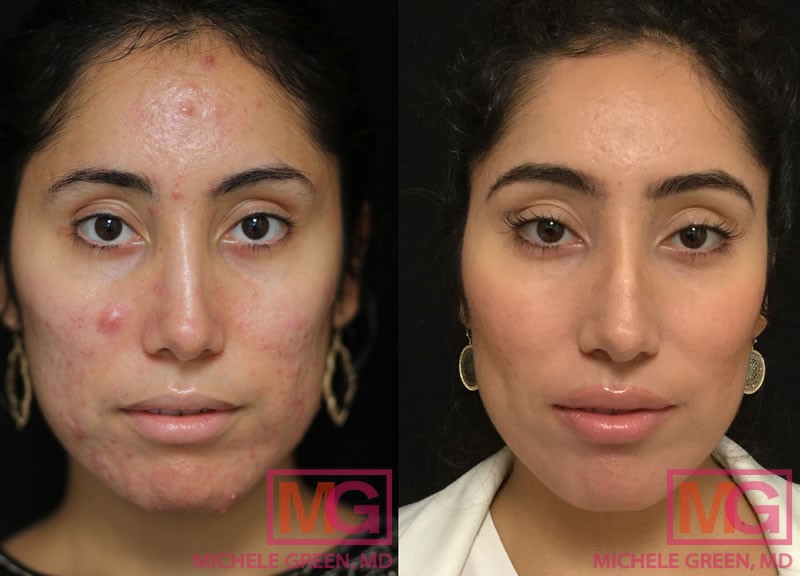
Acne vulgaris is one of the most common skin conditions, affecting as many as 50 million people in the United States each year, according to the American Academy of Dermatology. Known colloquially as “acne,” it often affects adolescents but can occur in patients of any age. Patients may develop many types of acne, including non-inflammatory blackheads and whiteheads, and inflammatory papules, pustules, nodules, and cysts. Characterized by small, red, painful, and inflamed blemishes, acne vulgaris can cause physical discomfort and feelings of frustration and low self-esteem, leading many to seek the best treatment. Board-certified dermatologist Dr. Michele Green in New York City has over 25 years of experience treating patients with acne vulgaris and can create a customized treatment plan to help manage and eliminate it.
Acne vulgaris has many causes, including genetics, hormonal fluctuations, stress, diet, environmental factors, and skincare regimens. Understanding the causes of your acne breakouts is crucial to treating and eliminating acne vulgaris. Often, the best approach to treating acne vulgaris breakouts is a combination of in-office treatments, oral medications, and topical therapies. With many treatment options available, it can be challenging to determine which are right for your specific type and severity of acne vulgaris. The first step in finding the best acne therapy for you is to schedule a consultation with expert board-certified dermatologist Dr. Green. Dr. Green will first assess your medical history and skin concerns to recommend the best treatments for acne vulgaris to help you achieve clear, acne-free skin.
Dr. Michele Green is an internationally renowned, board-certified dermatologist with over two and a half decades of experience providing some of the world’s most discerning individuals with the best non-invasive treatment options for a wide range of cosmetic concerns and medical skin conditions, including acne vulgaris. Dr. Green takes a holistic approach to acne treatment and masterfully combines non-invasive cosmetic procedures, topical therapies, and oral acne medications into individualized treatment plans that deliver clear, smooth, blemish-free skin that lasts. She is consistently recognized by Super Doctors, Castle Connolly, New York Magazine, and The New York Times as one of New York City’s best dermatologists for her dedication to her patients and expertise.
What is acne vulgaris?
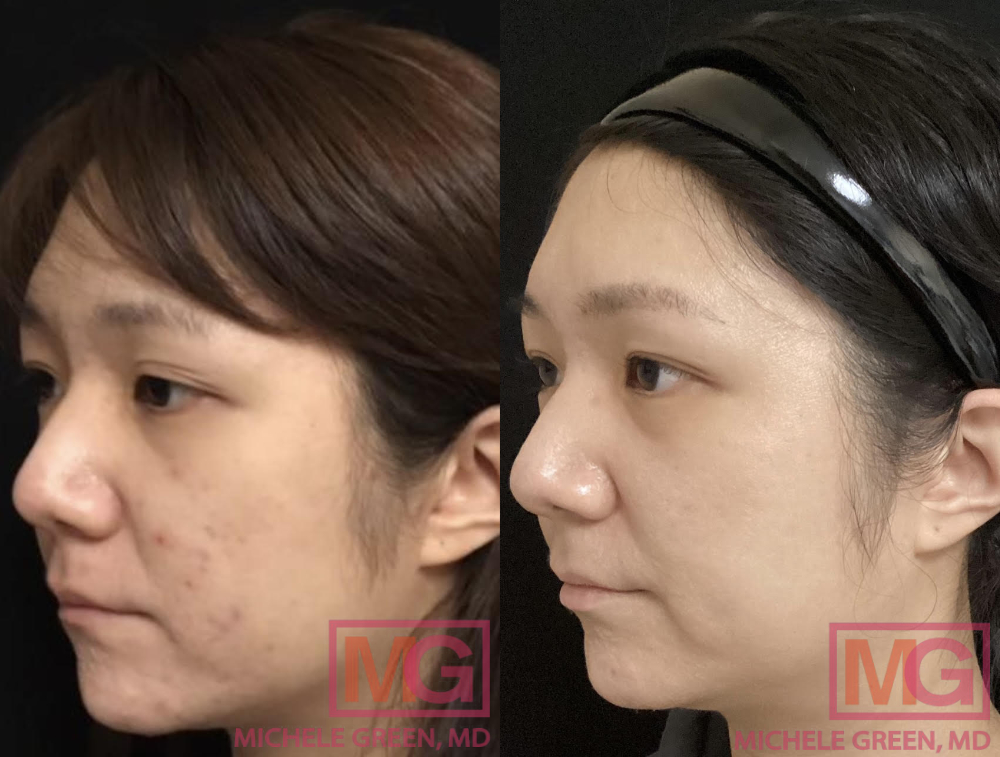
Acne vulgaris is the medical term for the skin condition commonly called acne. It is one of the most common skin conditions worldwide. Acne vulgaris occurs when the oil glands in the skin’s pores become clogged with excess sebum, dead skin cells, and other debris. Within the pores, bacteria can become trapped and rapidly multiply, leading to swelling, redness, tenderness, and irritation associated with a pimple. Acne vulgaris is commonly associated with adolescents but can occur in patients of any age. Acne is most commonly found on highly visible areas of the body, such as the forehead, chin, nose, upper back, and shoulders; however, lesions can develop wherever oil glands are present. Acne can be caused by a combination of factors, including genetics, hormones, diet, stress, hygiene, skincare, the environment, and even side effects of certain medications. Untreated or incorrectly treated acne, whether a single cyst or a persistent breakout of whiteheads, can have long-lasting ramifications, including permanent scarring (acne scars) and hyperpigmentation. A board-certified healthcare professional, such as a board-certified dermatologist, Dr. Green, can work with you to determine the underlying factors contributing to your breakouts and develop a personalized plan to address them.
What are the different types of acne vulgaris?
Acne vulgaris lesions are classified into two categories: non-inflammatory and inflammatory. Non-inflammatory acne lesions are mild and do not cause pain, swelling, or bacterial infection. Inflammatory acne lesions are moderate to severe and characterized by pain, tenderness, and scarring. Inflammatory lesions cause irreparable damage to the underlying skin tissue, leading to acne scarring. Non-inflammatory acne lesions include comedones (blackheads and whiteheads), while inflammatory lesions include papules, pustules, nodules, and cysts.
Non-inflammatory acne lesions
- Closed comedones, also known as whiteheads, are characterized by skin-colored bumps that form due to clogged hair follicles, specifically the pilosebaceous unit. The contents inside the pores are not exposed to air and are closed beneath the skin.
- Open comedones, also known as blackheads, are characterized by clogged pores with an opening at the skin’s surface. Exposure to air oxidizes sebum, dead skin cells, and pore debris, resulting in a characteristic black appearance.
Inflammatory acne lesions
- Papules are inflammatory lesions that form when a clogged hair follicle becomes inflamed. They appear as small red bumps that may be tender to the touch.
- Pustules are similar to papules but differ in that they are filled with pus due to a buildup of white blood cells. It is essential not to pick or pop pimples, as the pus released may spread to other pores, leading to further infection.
- Nodules are acne lesions that form when bacteria, Propionibacterium acnes (P. acnes), are trapped beneath the skin’s surface. They form a hard lump that is painful to the touch. Nodular acne has a high risk of scarring following infection.
- Cysts form when nodular acne fills with bacteria and pus. Similar to nodular acne, cystic acne extends deep under the skin’s surface. Cystic acne is considered the most severe form of acne because it can cause permanent tissue damage and scarring.
Who gets acne vulgaris?
Acne vulgaris is a widespread skin condition that can affect individuals of any age, but it is particularly prevalent among teenagers and young adults. The condition is often linked to hormonal changes during puberty, which can increase sebum production. Genetic factors also play a role, as acne tends to run in families and affects individuals across all races and genders. While acne is typically associated with adolescence, adult acne has become increasingly common, especially among women. This prevalence in women can be attributed to hormonal fluctuations related to menstrual cycles, pregnancy, or conditions such as polycystic ovary syndrome (PCOS). Additionally, factors such as stress, the use of certain oily cosmetics or skin products, and specific medications—including some contraceptives—can exacerbate or trigger breakouts in adults. When dealing with breakouts, it is best to consult with a board-certified dermatologist like Dr. Green to identify the root cause of the acne.
How is acne vulgaris treated?
Acne vulgaris can be managed with various treatments. During your consultation with Dr. Green, she will begin by taking a comprehensive medical history and conducting a thorough examination of your acne. This initial assessment is crucial to determine the severity and type of acne you are experiencing. If necessary, she may recommend blood tests to rule out underlying hormonal imbalances or other conditions that could be contributing to your breakouts. The treatment plan for acne vulgaris typically involves a combination of oral and topical medications. Topical treatments may include retinoids, benzoyl peroxide, or salicylic acid, while oral medications may include antibiotics, anti-inflammatory medications, or hormonal therapy, depending on your skin’s specific needs. In cases where the skin appears particularly congested with clogged pores, Dr. Green might suggest acne surgery, a procedure that carefully extracts these blockages. To enhance healing and minimize the potential for scarring, she may also inject corticosteroids into the affected areas. It’s essential to address acne breakouts promptly with a board-certified dermatologist like Dr. Green. Early intervention not only helps manage the acne itself but also significantly reduces the risk of developing scars, which can be much more difficult and complex to treat later on.

How is acne vulgaris treated?
Acne vulgaris can be managed with various treatments. During your consultation with Dr. Green, she will begin by taking a comprehensive medical history and conducting a thorough examination of your acne. This initial assessment is crucial to determine the severity and type of acne you are experiencing. If necessary, she may recommend blood tests to rule out underlying hormonal imbalances or other conditions that could be contributing to your breakouts. The treatment plan for acne vulgaris typically involves a combination of oral and topical medications. Topical treatments may include retinoids, benzoyl peroxide, or salicylic acid, while oral medications may include antibiotics, anti-inflammatory medications, or hormonal therapy, depending on your skin’s specific needs. In cases where the skin appears particularly congested with clogged pores, Dr. Green might suggest acne surgery, a procedure that carefully extracts these blockages. To enhance healing and minimize the potential for scarring, she may also inject corticosteroids into the affected areas. It’s essential to address acne breakouts promptly with a board-certified dermatologist like Dr. Green. Early intervention not only helps manage the acne itself but also significantly reduces the risk of developing scars, which can be much more difficult and complex to treat later on.
What is the main cause of acne vulgaris?
Acne vulgaris occurs when pores and hair follicles, specifically the pilosebaceous unit, become clogged with excess oil, dead skin cells, and other debris. Naturally occurring skin bacteria can also become trapped in pores, where they multiply, leading to irritation, inflammation, and the characteristic tenderness of a pimple. Some patients have a genetic predisposition to acne due to increased numbers of sebaceous glands or higher sebum production. Acne is also strongly linked to endocrine factors, including those associated with puberty, the menstrual cycle, pregnancy, and menopause, which play a significant role in its development. Androgen hormones, or male sex hormones like testosterone, can increase sebum production and the risk of breakouts.
Additionally, keratin, a naturally occurring protein, plays a central role in acne vulgaris. Excess keratin causes skin cells to shed abnormally and clump together, forming plugs (hyperkeratinization) that block hair follicles, trapping oils and bacteria and resulting in blackheads, whiteheads, and inflamed pimples. When you consult with Dr. Green at her private dermatology office on Manhattan’s Upper East Side, she will physically evaluate your skin, collect a thorough medical and family history, and may order blood tests for laboratory evaluation. Depending on your consultation, Dr. Green will recommend a unique combination of topical treatments, oral medications, and in-office procedures to treat your existing acne and prevent new breakouts, resulting in a smooth, clear, healthy complexion.
Is acne vulgaris fungal or bacterial?
Acne can be fungal or bacterial. The most common form of acne is bacterial, caused by the bacteria Cutibacterium acne (C. acnes). C. acnes is naturally found on the skin’s surface; however, C. acnes trapped in pores or hair follicles, along with sebum, dead skin cells, and debris, can result in bacterial proliferation, inflammation, and moderate to severe acne lesions such as papules, pustules, nodules, and cysts. Fungal acne is caused by an overgrowth of Malassezia yeast on the skin, another naturally occurring skin organism. Yeast and bacteria levels on the skin’s surface are typically maintained to balance each other out. When yeast production far exceeds bacterial production, a yeast infection in the pores can lead to fungal acne breakouts. Yeast production can be accelerated in warm, oily, moist environments. During your acne assessment, a culture can be taken to determine whether a fungal or bacterial infection is causing your breakouts.
How to stop acne vulgaris?
The best way to stop acne vulgaris is to consult a board-certified dermatologist. Several factors contribute to acne, and its severity varies from patient to patient. The Journal of the American Academy of Dermatology (JAAD) provides evidence-based guidelines for managing acne vulgaris, and the Journal of Clinical Dermatology (J Clin Dermatol) offers scientific articles on the systematic treatment of acne vulgaris. However, it is important to consult a dermatologist to tailor a regimen to your specific skin type and concerns and to ensure you use these active ingredients at appropriate concentrations to avoid irritation. Acne vulgaris typically requires a combination of treatments and good hygiene. When you visit Dr. Green’s private dermatology office, she will examine your skin and determine the best course of treatment for you to stop your acne vulgaris permanently.
When should you consult a dermatologist for treatment of acne vulgaris?
It is essential to consult a dermatologist as soon as an acne vulgaris breakout occurs. When left untreated, acne lesions, particularly non-inflammatory ones, can lead to inflammation, tissue damage, and scarring. Acne scars are permanent and often harder to treat than the breakouts themselves. According to the American Academy of Dermatology’s “Guidelines of Care for the Management of Acne Vulgaris” (J Am Acad Dermatol. May 2016;74(5):945–973.e33), the best approach for eliminating acne vulgaris is typically a customized combination of topical and oral therapies that target different aspects of acne pathogenesis (the factors that lead to breakouts). If your acne lesions do not respond to over-the-counter treatments, it is best to consult a board-certified dermatologist such as Dr. Green. She will first assess your medical history and skin concerns, then order blood tests to determine whether any underlying factor is causing your breakouts. She will then tailor a treatment plan that includes in-office treatments, oral medications, and topical creams to help you clear your acne for good.

In-office Treatments for Acne Vulgaris
Acne surgery
Acne surgery is a highly effective procedure for treating painful inflammatory lesions, including pustules, papules, and cysts. During the procedure, the lesions are opened, and the dead skin cells, sebum, and dirt trapped inside the pore are removed. A steroid is then injected into the lesion to shrink it, accelerate healing, and prevent acne scarring. If the acne cyst is very large, it must be drained before the corticosteroid injection. With no downtime, acne surgery is an excellent treatment option for reducing acne breakouts.
VBeam Laser
The VBeam laser is a non-invasive pulsed dye laser that can treat acne breakouts and pigmented acne scars. The VBeam laser uses a 595nm wavelength to eliminate red pigmentation, inflammation, and acne-causing bacteria. In addition to treating acne and acne breakouts, the VBeam laser treats broken capillaries, rosacea, telangiectasias, red stretch marks, and post-inflammatory hyperpigmentation. There is no downtime associated with the procedure, and patients can resume their daily activities afterward. Patients often need a series of treatments, each spaced one month apart, to achieve the best cosmetic results.
Chemical peels
Chemical peels work to gently exfoliate the skin, removing dead skin cells, debris, and sebum from clogged pores. The chemical exfoliants used during the procedure also kill acne-causing bacteria, reducing the risk of breakouts of acne vulgaris. Dr. Green typically uses trichloroacetic acid (TCA) during chemical peels for acne, as it helps to stimulate skin cell turnover and keep pores clear. TCA peels can also improve skin texture and tone, resulting in a more rejuvenated appearance. Dr. Green may recommend 4 to 6 chemical peels, depending on the type and severity of your acne.
HydraFacials
A HydraFacial is a multi-step treatment that gently cleanses, exfoliates, and nourishes the skin. The first step is to remove any superficial impurities on the skin’s surface. The second step uses salicylic and glycolic acids, two hydroxy acids, to break down dirt, dead skin cells, and sebum in clogged pores, exfoliating the skin. The last step involves hydrating and soothing the skin with a blend of hyaluronic acid and peptides. A HydraFacial can also be enhanced with personalized boosters based on specific skin concerns. The Murad Clarifying Booster is an excellent addition for treating acne breakouts, as it contains salicylic acid to provide a deeper cleanse and green tea extract to soothe redness and irritation. The ZO Rozatrol Booster is also excellent for acne vulgaris, containing rosa canina extract and lactose to reduce redness and inflammation. Additionally, red LED light therapy can further reduce redness, while blue LED light can kill acne-causing bacteria on the skin’s surface.
Oral medications for acne vulgaris
Oral antibiotics can be prescribed for moderate-to-severe acne vulgaris to reduce the prevalence of acne-causing bacteria on the skin’s surface and to help clear acne vulgaris. The most commonly prescribed systemic antibiotics for acne vulgaris include sarecycline, doxycycline, tetracycline, and minocycline. Oral antibiotics are effective for treating acne vulgaris breakouts, but they are not intended for long-term use. Proper sun protection is essential when using an oral antibiotic, as it can increase the skin’s sensitivity to sunlight.
Women experiencing acne vulgaris due to hormonal fluctuations and polycystic ovarian syndrome (PCOS) can benefit from using Spironolactone or oral contraceptives. Spironolactone is an anti-androgen medication that helps regulate androgen (male hormone) levels, reducing acne breakouts. Oral contraceptives help regulate hormone levels to reduce sebum production and acne vulgaris. In order to effectively treat acne, oral contraceptives must contain some form of estrogen and progesterone. Drospirenone, a progestin in birth control pills like Yaz (drospirenone/ethinylestradiol), effectively treats moderate acne by blocking androgens that trigger excess oil production, leading to fewer breakouts, inflammation, and clogged pores. Yaz, Ortho Tricyclen, and Estrostep are three FDA-approved oral contraceptives for the treatment of acne vulgaris.
Patients with more severe cases of acne breakouts who do not respond to topical or oral medications can benefit from oral isotretinoin. Isotretinoin, more commonly known by its brand name Accutane, is a vitamin A derivative that decreases sebum production, reduces the size of sebaceous glands, increases the rate of skin cell turnover, and inhibits the growth of acne-causing bacteria on the skin’s surface. Other brand names of oral isotretinoin include Absorica, Amnesteem, Claravis, Myorisan, and Zenatane. Accutane is typically prescribed for a short 20-week course to treat and eliminate acne vulgaris breakouts permanently. Clinical trials with Accutane have demonstrated complete or nearly complete cessation of acne breakouts after therapy. Roughly 95% of patients who take Accutane find that their acne vulgaris does not return. The remaining 5% of patients can undergo a second course of Accutane to clear their breakouts permanently. The most common adverse effects of Accutane include dry skin, lips, and eyes. Because the FDA regulates Accutane prescriptions, patients must have monthly visits and bloodwork tests before the medication can be prescribed. Because Accutane can cause severe congenital disabilities if taken while pregnant, patients who can become pregnant must additionally have monthly pregnancy tests and pledge to either abstinence or two forms of birth control.
Prescription topicals to treat acne vulgaris
Topical retinoids, derivatives of vitamin A, have been used to treat acne vulgaris for more than 30 years and are highly effective at reducing inflammation and follicular clogging. They accelerate skin cell turnover, exfoliating the skin and removing pore buildup. Many topical retinoid formulations are available, including tretinoin, adapalene, dapsone, and tazarotene. Retinoids should be used at night with proper sun protection, as they can make the skin more sensitive to the sun. Topical antibiotics manage acne breakouts by eliminating the bacteria responsible for acne vulgaris and reducing inflammation. The most common topical antibiotics prescribed for acne vulgaris are erythromycin and clindamycin, available in concentrations of 1-4%. Winlevi is a topical treatment containing clascoterone, an androgen inhibitor that blocks the skin’s production of excess oil. By preventing excess sebum production, Winlevi helps keep pores clear and treats active acne breakouts. It is suitable for both males and females aged twelve and older.
What is the fastest way to cure acne vulgaris?
The most effective approach to treating acne vulgaris is to consult a board-certified dermatologist, such as Dr. Green. A personalized evaluation will help determine the most suitable treatment plan for your skin type and condition. Among the available options, Accutane (isotretinoin) is one of the most potent treatments. It’s typically prescribed as a 20-week oral course and is known for significantly reducing acne lesions and preventing future breakouts. Accutane works by targeting multiple factors that contribute to acne, including excess oil production, clogged pores, and inflammation. Accutane is FDA-regulated and closely monitored by your board-certified dermatologist. Accutane is the closest thing to a cure for acne, and the results are permanent. Overall, a tailored approach under professional guidance is key to effectively managing and potentially curing acne vulgaris.
The best skincare regimen for acne vulgaris
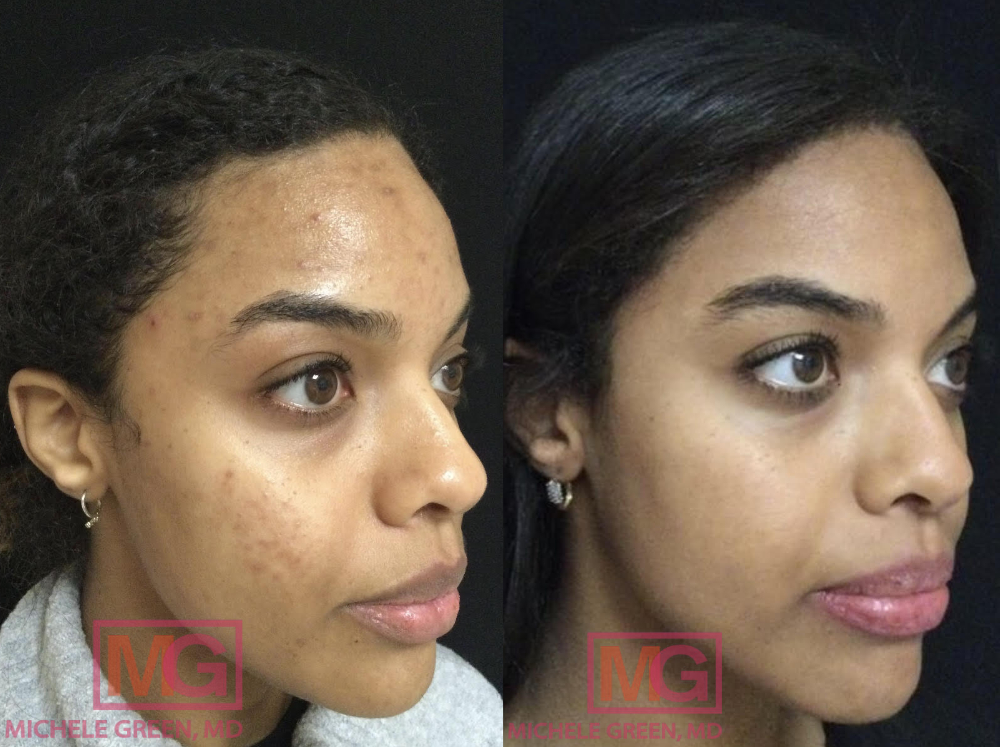
Adhering to a proper skincare regimen is essential for managing acne vulgaris and preventing new acne lesions. Board-certified dermatologist Dr. Michele Green’s proprietary skincare line, MGSKINLABs, contains an Acne Kit designed to manage acne breakouts effectively. The Pore Minimizing Cleanser uses glycolic and salicylic acid to gently exfoliate the skin, unclog pores, and minimize the appearance of enlarged pores. The Retexturizing Pads also contain glycolic and salicylic acids to cleanse the skin further and soften skin texture. Lastly, the Acne Spot Treatment contains 5% benzoyl peroxide to kill acne-causing bacteria, dry out acne lesions, and reduce inflammation. It is important to use the spot treatment once daily on inflamed breakouts to help kill bacteria, and to limit its use to once daily to avoid skin irritation, as these active ingredients can be drying and cause skin irritation.
Differin gel is an excellent over-the-counter exfoliant containing adapalene. In addition to increasing skin cell turnover, using Differin gel regularly can help reduce the buildup of dead skin cells and sebum, prevent the formation of new acne lesions, and improve skin texture and tone. Moisturizer is an essential step in any skincare routine, as it helps hydrate the skin and protect its natural moisture barrier. The best moisturizers for acne-prone skin are non-comedogenic ones, meaning they will not clog pores. The Ultimately Sheer Lotion from MGSKINLABs contains glycerin and the lipid squalene to hydrate the skin, as well as green tea extract to soothe inflamed skin. Sunscreen is incredibly important in any skincare regimen to protect the skin from harmful UV rays. For maximum sun protection, patients should use a broad-spectrum sunscreen with an SPF of 50. MGSKINLAB’s Hydrating SPF 50 contains zinc oxide to create a barrier against UV rays and hyaluronic acid to nourish the skin.
Will my acne vulgaris go away on its own?
Acne vulgaris is a skin disease characterized by dead skin cells, sebum, debris, and bacteria trapped in clogged pores. It often develops during adolescence but can affect patients of any age. While some patients may resolve their breakouts with over-the-counter products such as salicylic acid, azelaic acid, or benzoyl peroxide, most require medical intervention to clear their acne completely. Acne medications and treatments target the factors that cause breakouts, including excess sebum production, high concentrations of bacteria on the skin’s surface, inflammation, and clogged pores. These therapies can take time to work fully so that patients may see results after several weeks or months of treatment. If you are experiencing chronic acne, the best course of action is to schedule a consultation with board-certified dermatologist Dr. Michele Green to determine a treatment plan to help you clear your acne vulgaris and achieve clear, healthy skin.
Can acne vulgaris cause scars?
Yes, acne vulgaris can cause scarring. More specifically, inflammatory acne lesions such as papules, pustules, nodules, and cysts can cause irreparable damage to the underlying skin tissue, often resulting in permanent acne scars. Acne scars can appear as depressed indentations (atrophic scars) or raised growths (hypertrophic or keloid scars). Atrophic scars develop when insufficient collagen is produced during the wound-healing process, while hypertrophic scars develop when collagen is overproduced. Acne scars are often harder to treat than the initial acne lesion itself, which is why it is essential to consult with Dr. Green as soon as an acne vulgaris breakout occurs. While it may not be possible to completely remove acne scars, Dr. Green offers various non-invasive cosmetic procedures to help reduce their appearance.
Resurfacing lasers such as the Fraxel Laser and eMatrix Laser are excellent for stimulating collagen production and improving skin texture. Microneedling, also known as collagen induction therapy, can stimulate the production of new collagen, soften the appearance of depressed acne scars and fine lines, and even out skin tone. Dermal fillers like Juvederm, Restylane, and Sculptra can be injected into the skin to replenish lost volume from acne scarring. For some patients, acne scarring can also result in post-inflammatory hyperpigmentation, which appears as red or dark marks on the skin. Red acne scars can be treated with the VBeam laser, while dark marks can be treated with chemical peels like TCA peels or Mesopeels. Keloids or hypertrophic scars can be injected with a corticosteroid to shrink and flatten the scars. Patients can develop many types of acne scars, and it often takes a combination of treatments to address them fully. However, once your acne vulgaris breakouts are eliminated, Dr. Green can devise a customized acne scar treatment plan to eliminate your acne scars and create clear, radiant skin that lasts.
Frequently Asked Questions about Acne Vulgaris
Acne vulgaris vs. pimple
Acne vulgaris is the medical term for the skin condition commonly called acne. Within the broader term acne vulgaris, there are several types of acne, including open and closed comedones, papules, pustules, cysts, and nodular acne. Treatment depends on the type of acne present, which is why it is essential to consult a board-certified dermatologist when creating your treatment plan.
What is the most common type of acne?
The most common type of acne is comedonal acne, also known as whiteheads and blackheads. Comedonal acne forms when pores become clogged with dead skin cells, debris, and other impurities. Whiteheads are comedonal acne lesions covered by skin, appearing as skin-colored bumps. Blackheads are comedonal acne lesions with an opening at the skin’s surface, resulting in oxidation of the pore’s contents and the appearance of a dark, black bump.
What are the four stages of acne vulgaris?
Dermatologists can classify acne vulgaris into four stages or grades based on the severity of breakouts. Stage 1 is mild acne vulgaris, characterized by predominantly comedonal lesions and a few papules or pustules. Stage 2 is moderate or pustular acne vulgaris, characterized by multiple papules and pustules, along with blackheads and whiteheads. Stage 3 is moderately severe or nodulocystic acne vulgaris, characterized by numerous papules and pustules. Several inflamed nodules or cysts may develop and may extend to the back or chest. Stage 4 is severe nodulocystic acne vulgaris, characterized by numerous inflamed nodular or cystic lesions.
At what age is acne vulgaris the worst?
Acne vulgaris typically occurs most severely during adolescence due to hormone fluctuations associated with puberty. However, it can affect men and women of all ages to varying degrees.
At what age does acne vulgaris typically start?
Acne vulgaris is a common skin condition that typically begins during puberty, between the ages of 11 and 12. This onset is driven primarily by hormonal fluctuations associated with adolescence, which increase skin oil production. As a result, most teenagers and young adults experience some form of acne, and it can persist into their 20s or even 30s. However, acne can manifest at any age, sometimes starting earlier in childhood or later in adulthood due to factors such as hormonal imbalances, stress, or dietary choices. For those experiencing breakouts, it is crucial to seek the expertise of a board-certified dermatologist. They can provide individualized treatment plans tailored to one’s skin type and the severity of the condition. Early intervention is key to preventing potential complications, such as scarring, which can be challenging to treat once they occur. By consulting a dermatologist promptly, individuals can effectively manage their acne and reduce the risk of long-term skin damage.
Which vitamin deficiency causes acne vulgaris?
Acne vulgaris is a complex skin condition influenced by numerous factors, including hormonal fluctuations, bacteria, and genetic predisposition. Among these, Vitamin D deficiency has emerged as a significant contributor to the development and exacerbation of acne. Research indicates that individuals with acne often have lower Vitamin D levels than those with clearer skin. Vitamin D plays a crucial role in immune regulation and the proliferation and differentiation of skin cells. Insufficient Vitamin D may impair the immune system’s ability to combat inflammation, thereby increasing the severity of acne lesions. Vitamin D supports skin barrier function, and deficiency can compromise skin integrity, thereby promoting acne development. Thus, addressing Vitamin D deficiency through dietary changes, supplements, or increased sun exposure may help manage acne vulgaris. However, further research is needed to understand the relationship between Vitamin D levels and acne fully and to establish effective treatment protocols. It is best to consult a board-certified dermatologist before taking vitamin D supplements.
Can acne vulgaris spread?
Acne vulgaris is a common skin condition that is not contagious, meaning it cannot be transmitted from one person to another through contact. However, certain practices may facilitate the transfer of acne-causing agents. For instance, sharing makeup products, such as foundations or brushes, as well as towels or other personal items, can introduce excess oil, dead skin cells, and bacteria onto your skin. This exchange may disrupt your skin’s natural balance, potentially leading to clogged pores and more breakouts. Therefore, maintaining personal hygiene and using individual skincare and cosmetic products are essential to help prevent acne from worsening.
Can other conditions appear as acne vulgaris?
Yes! One skin disorder commonly mistaken for acne vulgaris is acne rosacea. Rosacea is a chronic inflammatory skin condition characterized by facial redness, flushing, and broken blood vessels. Patients with rosacea can also develop acne rosacea, characterized by acne-like lesions. Although acne rosacea resembles acne vulgaris, they are not the same. The exact cause of acne rosacea is unknown, though environmental or biological risk factors may trigger a breakout. Acne vulgaris, however, forms when pores are clogged with sebum, dead skin cells, debris, and, in cases of inflammatory acne, bacteria. Visible signs such as diffuse redness and facial telangiectasia often accompany acne rosacea. Another skin disorder often mistaken for acne vulgaris is perioral dermatitis. This disorder is characterized by inflammation and irritation of the skin around the mouth. It can appear as a bumpy, red, scaly rash that is often itchy. Lifestyle habits, topical or inhaled steroid use, or biological factors can trigger perioral dermatitis. If you are experiencing red bumps on your face that may look like acne breakouts, consult with a board-certified dermatologist like Dr. Green. Because acne vulgaris can resemble acne rosacea, perioral dermatitis, and other skin conditions, a proper diagnosis is crucial to ensure you use the correct treatments for your skin concerns.
Why did I get acne vulgaris?
Acne vulgaris occurs when pores become clogged with oil, dead skin cells, and debris, resulting in red bumps on the skin’s surface. Several risk factors contribute to the continued prevalence of acne vulgaris, including:
- Changes in hormone levels associated with puberty, menstruation, pregnancy, or menopause
- Medications such as corticosteroids, lithium, or testosterone
- Family history of acne breakouts
- A diet that is high in carbohydrates, sugars, dairy, and glycemic index foods.
- Chronic stress
- Improper hygiene, such as not washing with soap or cleanser after exercising
When you consult with Dr. Green in her private NYC When you consult with Dr. Green in her private NYC dermatology office, she will first review your medical history and skin concerns. She may order blood tests to determine whether any underlying factors are causing your acne breakouts. Afterward, she will create a customized acne vulgaris treatment plan to help you eliminate breakouts for good and achieve clear, smooth skin.
What natural remedies treat acne?
Tea tree oil is a powerful natural remedy known for combating acne-causing bacteria. Often used as a targeted spot treatment, it can significantly reduce the severity and duration of breakouts. Its antimicrobial properties are attributed to compounds such as terpinen-4-ol, which help diminish inflammation and prevent bacterial spread on the skin. Another beneficial natural ingredient is aloe vera, known for its soothing and hydrating effects. It helps alleviate inflammation and redness associated with existing pimples. While aloe vera can provide relief for inflamed skin, it does not actively prevent new breakouts. In addition to incorporating these natural remedies into your skincare routine, maintaining a balanced diet is crucial for managing acne. Consuming excessive processed foods and sugar can trigger hormonal fluctuations and inflammation, leading to acne flare-ups. Focusing on whole foods, such as fruits, vegetables, lean proteins, and healthy fats, can support overall skin health. While these natural approaches can be beneficial, it’s wise to consult with a board-certified dermatologist if you’re experiencing an increase in breakouts or if your skin issues persist. They can provide personalized advice and treatment options tailored to your specific skin needs.
What is the strongest natural antibiotic for acne?
Some natural antibiotics that can help break out acne include honey, tea tree oil, and sulfur. These ingredients contain antibacterial properties that may help fight acne. However, natural remedies are not always effective or safe, and it is important to consult a board-certified dermatologist, such as Dr. Green, before applying anything new to the skin. Honey-based products can help reduce redness associated with acne, but their antibacterial properties often do not protect against acne-causing bacteria like C. acnes. Some clinical studies support the use of tea tree oil for mild acne; however, it is essential to dilute it and never apply it directly to the skin, as it can cause irritation and burning, especially in patients with sensitive skin. Instead of trying home remedies that can irritate your skin and worsen acne breakouts, it is best to consult Dr. Green to get the right treatment options for your specific skin concerns.
What not to do with acne vulgaris?
Certain precautions should be taken to avoid worsening acne vulgaris breakouts. Patients should avoid harsh exfoliants or scrubs when cleansing the skin, as these can cause dryness, irritation, and worsening of acne. Oily skincare products should be avoided to prevent clogged pores and the development of new acne lesions. Skincare products for acne-prone skin should be oil-free and labeled non-comedogenic, meaning they will not clog pores. Patients with acne vulgaris should not wear sweaty clothes for a long time after working out, as sweat trapped between workout clothing and skin can clog pores, trap oil, debris, and bacteria, and lead to acne breakouts. Instead, patients should remove sweaty clothes and cleanse their skin as soon as possible to prevent new acne from forming. It is also critical not to “pop” or squeeze acne breakouts, as this can cause scarring.
Can you pop acne vulgaris?
No! An acne vulgaris lesion should never be popped or picked at, as the pus and bacteria trapped inside can spread to other clogged pores and infect them. Popping a pimple can also damage skin tissue and create an acne scar, which is often harder to treat than the acne lesion itself. The best thing to do when experiencing acne vulgaris is to consult with Dr. Green in her private boutique dermatology office in New York City. There, she will assess your skin and medical history and order any necessary lab tests to determine factors that may be contributing to your acne vulgaris. She will then customize an acne vulgaris treatment plan with in-office treatments, topical and oral medications, and targeted skincare products to help eliminate your acne for good.

How to get started with acne vulgaris treatment today
Acne vulgaris is a skin condition that affects as many as 50 million Americans annually, making it one of the most common skin disorders in the US. Breakouts are typically associated with adolescence, though they can persist or develop well into adulthood. While some individuals can keep breakouts at bay with over-the-counter products, many find that their skincare routines are not enough to prevent or manage acne vulgaris. Fortunately, many professional treatment options are available at Dr. Green’s private dermatology office, including topical treatments, oral medications, and in-office treatments. Research has shown that the best way to combat acne vulgaris is to take a combination approach, using various topical and oral therapies along with dermatological procedures to achieve smooth, clear, bright skin that lasts. With so many treatment options to choose from, it can be difficult to know which will be best for you, which is why the best first step in treating acne vulgaris is to schedule an appointment with expert dermatologist Dr. Michele Green.
Dr. Michele Green is an internationally renowned board-certified dermatologist with over two and a half decades of experience providing some of the world’s most discerning individuals with the best non-invasive treatment options, including acne surgery, HydraFacials, and prescription acne medications. Dr. Green takes a holistic approach and embraces a less-is-more philosophy, creating customized skincare routines and treatment plans tailored to her patients’ unique concerns and aesthetic goals. She is consistently recognized by Castle Connolly, New York Magazine, Super Doctors, and The New York Times as one of New York’s best dermatologists for her dedication to her patients and expertise. Please call us at 212-535-3088 or email our New York City-based office today to schedule a consultation with Dr. Michele Green and get started with your personalized acne treatment.
 212-535-3088
212-535-3088