Back Acne
Back acne, commonly referred to as “bacne,” is one of the most common forms of acne, affecting more than half of individuals who experience breakouts. According to the American Academy of Dermatology (AAD), over 50 million Americans deal with acne each year, making it one of the most common skin conditions. It can occur anywhere on the body, often causing patients to feel self-conscious. When it appears on the back, it typically presents as cysts or nodules that can be painful. Back acne can affect people of any age and gender, with risk factors including poor hygiene, an inadequate skincare routine, high stress levels, and a family history of acne. Managing acne treatment and prevention can be overwhelming, so consulting a board-certified dermatologist, such as Dr. Michele Green in NYC, is essential. Dr. Green specializes in treating all types of acne, including back and facial acne, and can help you achieve clear, healthy skin by permanently removing back acne.
Several treatment options and preventive strategies can help manage back acne and reduce the risk of future outbreaks. Prevention can be as simple as changing your post-workout bathing routine or washing your linens more frequently. When these steps aren’t enough, many over-the-counter topical cleansers and creams containing benzoyl peroxide or salicylic acid can help remove dead skin cells, clear pores, and reduce acne. If these topical treatments don’t work, it’s time to see Dr. Green to explore other options, such as HydraFacials, prescription medications like oral antibiotics, or Isotretinoin (Accutane). Dr. Green can also help you develop a personalized skincare routine with the best products to keep your skin clear and smooth.
Dr. Michele Green is an internationally acclaimed, board-certified dermatologist specializing in cosmetic dermatology with over 25 years of experience. She offers some of the most discerning men and women worldwide the best non-invasive treatments for acne and acne scars. At her private dermatology practice on Manhattan’s Upper East Side, she skillfully uses the latest technology and innovative techniques to deliver natural-looking, long-lasting results that help her patients look and feel their best. She is consistently recognized by Super Doctors, New York Magazine, and Castle Connolly as one of New York’s top dermatologists. When working with Dr. Green, she recommends a personalized blend of premium skincare products and in-office treatments, such as Botox, dermal fillers, chemical peels, laser therapies, and more, to achieve optimal results.
What is back acne?
Back acne, also known as “bacne,” is a common breakout that appears on the back. While the face is the most common area for acne, it can develop anywhere on the body where sebaceous glands are present. Body acne, which often appears on the chest, back, and buttocks, can be frustrating and uncomfortable for many individuals. Back acne is most often found along the shoulders and upper back, but can occur anywhere on the back. It can include whiteheads, blackheads, pimples, papules, cysts, or nodules. Although hormonal changes like puberty or pregnancy are common causes, anyone can develop bacne. Factors such as genetics, lifestyle, medications, skincare, and hygiene also play a role. Prompt and effective treatment is crucial to prevent long-term scarring, which can be more difficult to treat than the acne itself. Therefore, consulting a board-certified dermatologist, such as Dr. Michele Green in NYC, as soon as possible is essential for proper care.
What are the different types of acne?
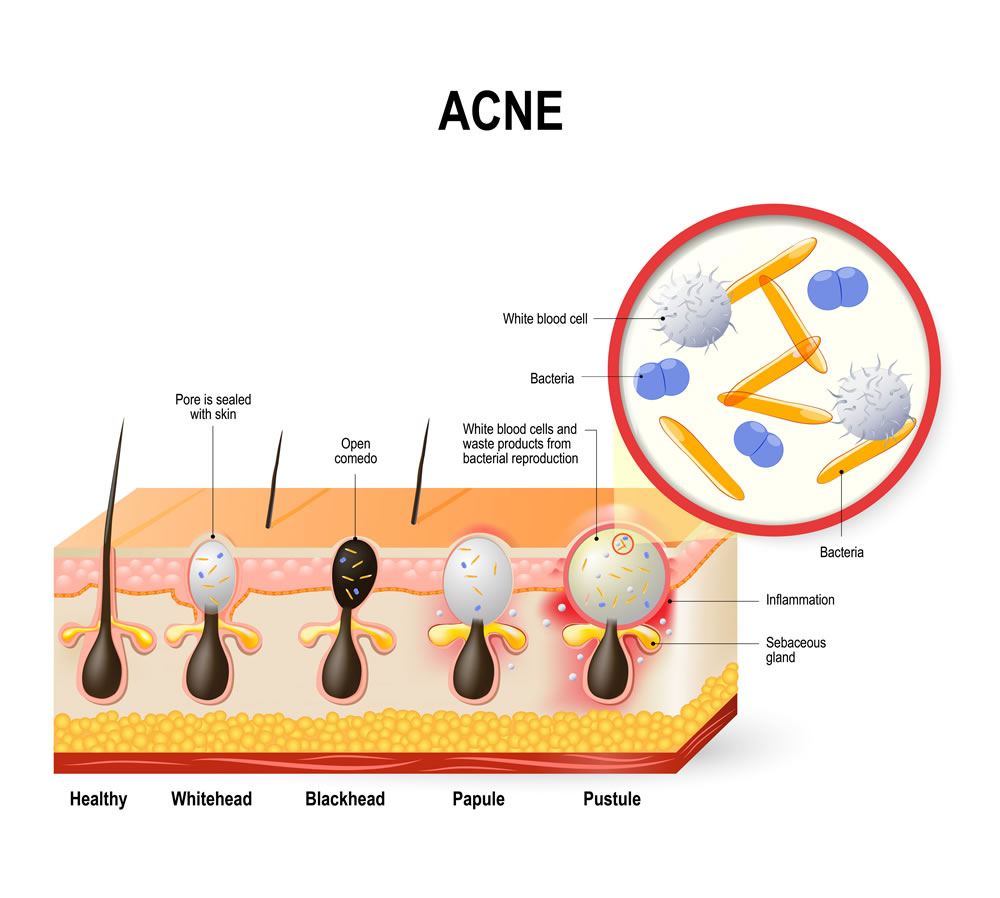
Several types of acne lesions can develop on the back, including whiteheads, blackheads, papules, pustules, nodules, and cysts. Whiteheads, also called closed comedones, form when pores or hair follicles become clogged with dirt, debris, and sebum. They are called closed comedones because the pore remains shut, trapping debris beneath the skin and giving the bump a white top. Similarly, blackheads form when oil, dead skin cells, and other debris clog the hair follicle. However, unlike whiteheads, blackheads are open comedones, meaning the pore is open on the skin’s surface. Open comedones appear black because sebum in the pore reacts with air.
Papules are a type of inflammatory acne that appear as red bumps on the skin’s surface. They may be painful or irritated, but do not have a pus-filled tip. Pustules, often called pimples, are another type of inflammatory acne. Unlike papules, pustules are filled with pus, a collection of white blood cells. The pus often gives pustules a white or yellow appearance. Nodules form when a clogged hair follicle becomes infected with bacteria. They develop deeper within the tissue, resulting in a hard, red bump on the skin’s surface that is often painful. Cystic acne occurs when pus-filled acne is also infected with bacteria. Cysts form deeper under the skin and often develop a red bump on the surface, causing pain and discomfort.
The cause of back acne
Acne occurs when excess oil, dead skin cells, sweat, and other debris clog the skin’s pores. Clogged pores can prompt the sebaceous glands to produce more sebum, worsening the buildup of debris in the follicles. When pores are blocked, skin bacteria called cutibacterium can become trapped inside, leading to inflammation and more painful pimples. The pores on the back are especially prone to sweat acne, which can occur when sweat, friction, and heat combine to clog pores and trap cutibacterium within them. Friction from backpack straps, sports gear, non-wicking clothing, hats, and headbands can also contribute to this issue. Fortunately, simple lifestyle changes can help reduce the risk of developing back acne. Many factors contribute to the development of back acne, including:
Genetics: Individuals who have a family history of acne tend to have a higher likelihood of experiencing breakouts compared to those without such a background. People with a genetic predisposition to increased sebum production face an elevated risk of clogged pores, as excess oil can trap dead skin cells and bacteria in hair follicles. This combination of genetic factors makes certain individuals more susceptible to acne, underscoring the importance of understanding one’s genetic background in managing skin health.
Hormone Fluctuations: Hormonal fluctuations can significantly impact skin health, often leading to outbreaks of body acne, also known as bacne. This is particularly prevalent in individuals undergoing puberty, as their bodies experience a surge in hormones such as androgens, which can increase oil production in the skin. Similarly, women may notice a higher propensity for body acne during menstruation due to shifts in estrogen and progesterone levels, which can also affect oil gland activity. Additionally, pregnancy brings about substantial hormonal changes that can exacerbate skin issues, making some individuals more susceptible to acne on the back and shoulders.
Poor Hygienic Practice: Maintaining proper hygiene is essential to preventing back acne, also known as back zits. After physical activity, your body sweats as a natural response to regulate temperature. However, when sweat becomes trapped under tight-fitting workout clothing, it can clog pores. This environment allows oil, dirt, and debris to accumulate, which can exacerbate existing acne or trigger new breakouts. Moreover, sweat itself can serve as a breeding ground for bacteria on the skin. If this sweat is not cleansed promptly, the bacteria can proliferate, leading to inflammation and further skin issues. Additionally, having a consistent laundry routine for bed linens, including sheets and pillowcases, is crucial for skin health. When these items are not washed regularly, they can accumulate dirt, dead skin cells, dust mites, and other debris. This buildup can transfer back to your skin when you lie down to sleep, potentially clogging pores and contributing to acne development. To minimize the risk of back acne, shower promptly after exercising, wear breathable, sweat-wicking fabrics during workouts, and keep your sleeping environment clean by washing bed linens frequently.
Diet: Diets that are high on the glycemic index, particularly those rich in carbohydrates and sugars, have been linked to an increased prevalence of acne breakouts. When we consume foods that rapidly raise blood sugar levels, such as white bread, sugary pastries, breakfast cereals, full-fat milk, and carbonated beverages, our bodies respond by increasing insulin production. This spike in insulin can promote sebum overproduction and inflammation, both of which are significant contributors to acne, including bacne (back acne). To mitigate this risk, it may be beneficial to reduce the intake of these high-glycemic foods and replace them with lower-glycemic alternatives. Whole grains, fruits, vegetables, and lean proteins can help stabilize blood sugar levels and reduce the likelihood of breakouts.
Friction: Acne mechanica is a specific form of acne that typically develops from friction between the skin and various surfaces, such as clothing, sports equipment, or other materials. This type of acne is exacerbated by sweat, which can increase irritation and clog pores in the affected areas. For instance, back acne often occurs where backpack shoulder straps contact the skin, causing friction and, consequently, breakouts. Similarly, athletes may experience acne mechanica in areas that are in close contact with tight-fitting sports gear, such as shoulder pads or tight clothing, which can trap moisture and heat against the skin. The condition underscores the importance of maintaining clean, breathable fabrics and ensuring that any equipment or clothing used during physical activity allows for adequate airflow to minimize the risk of breakouts.
Medication: Certain prescription medications can increase the risk of developing body acne. Some of these include corticosteroids, which are often prescribed for conditions like asthma or autoimmune disorders; progestin contraceptives, known for influencing hormonal balance; and lithium, commonly used in the treatment of bipolar disorder. These medications can affect the skin in various ways, such as altering hormone levels or altering oil production, which may lead to clogged pores and subsequent breakouts. It’s essential for individuals taking these medications to be aware of this potential side effect and to consult a healthcare provider to manage their skin health effectively.
Improper skin care: Certain skincare products, particularly lotions and creams, can contain high levels of oil, which may increase sebum production. This excess oil can clog pores, potentially worsening acne for those with acne-prone skin. To mitigate this risk, these individuals must select non-comedogenic products. This term indicates that the formulation is designed not to block pores, thereby reducing the likelihood of breakouts. Moreover, individuals dealing with back acne may be tempted to scrub their backs vigorously to exfoliate and clear the skin. However, this approach can be counterproductive. Friction from scrubbing can irritate the skin, leading to inflammation and potentially aggravating the very condition they are trying to treat. Instead, gentle exfoliation methods that account for skin sensitivity and incorporate salicylic or glycolic acid may be more effective for managing bacne without causing additional irritation.
Stress: Patients exposed to stressful environments or experiencing heightened anxiety levels may be at a greater risk for developing acne breakouts across various parts of their bodies. This correlation arises because stress triggers the overproduction of certain hormones, particularly cortisol, which can significantly influence skin health. As cortisol levels rise, the body’s sebaceous (oil) glands become more active, increasing sebum production. This excess sebum can clog pores, creating an ideal environment for acne-causing bacteria to thrive. Additionally, stress may contribute to skin inflammation and irritation, further exacerbating the condition. Factors such as poor diet, lack of sleep, and neglect of skincare routines—common during periods of stress—can also contribute to worsening acne breakouts.
Malassezia yeast: Fungal acne, also known as folliculitis, often appears on the back as small, itchy, acne-like red bumps or whiteheads. This condition results from infection of hair follicles, commonly caused by bacteria or the yeast Malassezia, which is present on the skin’s surface. Unlike traditional acne, which is primarily driven by excess oil production and clogged pores, fungal acne flourishes in warm, humid environments where sweat accumulation creates an ideal breeding ground for these microorganisms. Effective management of fungal acne requires a targeted approach, as standard acne treatments may not be effective. It is crucial to consult a board-certified dermatologist to diagnose the root cause of your acne.
How to treat back acne
When navigating the many treatment options for back acne, it is best to consult a board-certified dermatologist, such as Dr. Green. One of the most important reasons to consult an experienced board-certified dermatologist as soon as possible about your back acne is that inflammation associated with acne lesions can lead to scarring. Acne scars are often much more difficult to treat than acne breakouts themselves. Treating acne effectively and promptly is the best way to prevent scarring. Dr. Green can help determine the combination of oral medications, skincare products, in-office procedures, and topical treatments that will work best for your acne type and lifestyle. When you consult with Dr. Green, you will have the opportunity to discuss your specific skin concerns and overall aesthetic goals. She will then work with you to create a customized treatment plan tailored to your needs.
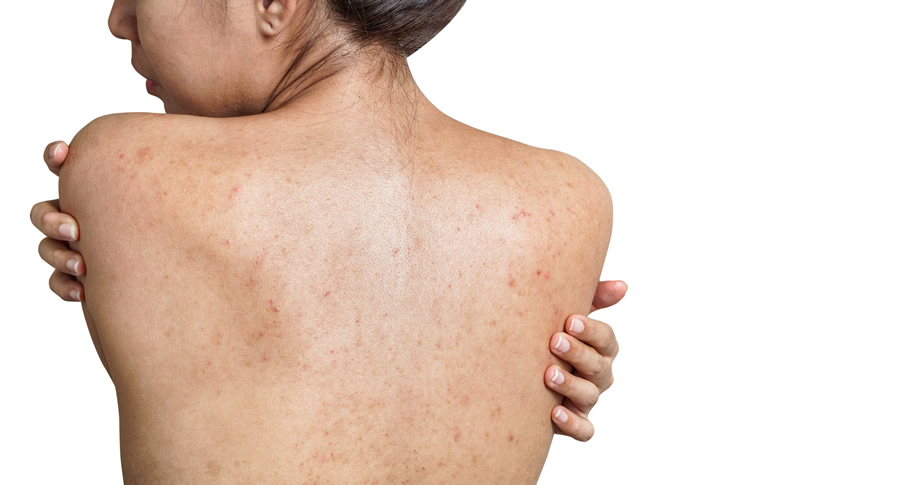
Dermatologist-approved back acne treatments
There are many ways to address back acne, including prescription topicals, oral medications, and in-office procedures. Although acne is incredibly common, each person may break out for different reasons. Thus, each patient requires a customized acne treatment plan to clear their breakouts effectively. The first step in eliminating back acne blemishes is to consult with an experienced dermatologist, such as Dr. Green in NYC. With over two and a half decades of experience, Dr. Green will examine the type of acne you are dealing with and recommend the best course of treatment.
Acne surgery
Acne surgery is an in-office procedure used to treat inflammatory acne lesions, including papules, pustules, and cysts. During the procedure, active acne lesions are opened, and their contents—such as dead skin cells, dirt, and sebum—are removed with a medical instrument. A steroid is then injected into the area to reduce inflammation and shrink the lesion. Acne surgery is highly effective at eliminating breakouts and significantly reduces the risk of acne scarring during healing.
VBeam laser
The VBeam laser is a 595nm pulsed dye laser that reduces red pigmentation in the skin. It is an effective treatment for acne because it decreases inflammation and eliminates acne-causing bacteria from the skin’s surface. There is no downtime with this treatment, and patients can resume their daily activities immediately afterward. In addition to treating acne, the VBeam laser also targets red acne scars, post-inflammatory hyperpigmentation, rosacea, facial redness, broken capillaries, and red stretch marks. Patients may need 3 to 6 treatment sessions, spaced 1 month apart, to achieve optimal acne results.
HydraFacials
A HydraFacial is a three-step medical-grade hydra dermabrasion treatment that gently cleanses, exfoliates, and nourishes the skin. Its proprietary vortex technology effectively removes sebum, dead skin cells, and debris trapped in pores, which can cause acne. After cleansing and exfoliating, antioxidants, vitamins, and peptides are infused into the skin to boost its natural protective barrier. The treatment can also be combined with LED light therapy and specialized boosters to target specific skin concerns, including acne. The red LED light helps reduce redness and inflammation associated with acne, while the blue LED light kills acne-causing bacteria on the skin’s surface. Boosters are applied after cleansing and exfoliating to deliver targeted active ingredients. The Murad Clarifying Booster offers a deeper pore cleanse to reduce breakouts, while the ZO Rozatrol Booster helps lessen redness and inflammation. HydraFacial can be performed on areas of the body prone to acne, including the face, back, and buttocks. Typically, patients receive an initial series of three HydraFacials, spaced one month apart, followed by maintenance treatments as needed to maintain results.
Chemical Peels
A chemical peel is a non-invasive cosmetic treatment that boosts skin cell turnover, removing dead skin cells from the surface and unclogging pores. Chemical peels help treat acne and improve dullness, fine lines, and uneven skin tone. There are many types of chemical peels available, and Dr. Green works with each patient individually to tailor treatment to their unique needs and aesthetic goals. Multiple sessions, spaced three to four weeks apart, are usually necessary to achieve the best results.
Oral medications
Oral antibiotics are an effective treatment for acne because they reduce the bacteria that cause breakouts on the skin’s surface. Commonly prescribed oral antibiotics for acne include Minocycline, Tetracycline, and Doxycycline. However, oral antibiotics should not be used as a long-term solution.
Women experiencing back acne may consider Spironolactone, an oral androgen blocker that lowers androgen levels, such as testosterone, thereby reducing sebum production and preventing breakouts. Oral contraceptives can also be effective against acne due to their estrogen and progestin content. Ortho Tri-Cyclen, Yaz, and Estrostep are three FDA-approved oral contraceptives for treating acne.
Patients with moderate to severe cystic or nodular acne, or those experiencing persistent acne breakouts that do not respond to other treatments, may consider oral isotretinoin. Isotretinoin, commonly known as Accutane, is a vitamin A derivative that reduces sebum production, levels of acne-causing bacteria, and inflammation, helping to eliminate acne breakouts permanently. Accutane also speeds up skin cell turnover, preventing dead skin cells from clogging pores. It is usually prescribed for a short course, typically 5 to 6 months. Patients on Accutane are required to have monthly visits and blood work with Dr. Green to continue their treatment. Women must also commit to abstinence or use two forms of birth control during treatment. Approximately 95% of patients who take Accutane achieve permanent acne clearance; the remaining 5% may require a second course for complete clearance.
Doxycycline for back acne
Doxycycline is an oral antibiotic with anti-inflammatory properties that can be prescribed to treat severe back acne breakouts. The medication kills acne-causing bacteria on the skin, thereby preventing breakouts. Oral antibiotics, such as doxycycline, should be taken only for a short period and in small doses to avoid the development of antibiotic-resistant bacteria.
Spironolactone for back acne
Spironolactone is an oral medication used to treat hormonal acne in women by blocking androgen action at sebaceous glands and reducing androgen secretion from the adrenal gland. Lower androgen levels can reduce sebum production, leading to fewer acne breakouts and flare-ups. The American Academy of Dermatology Association found that, on average, women notice a decrease in acne breakouts and oiliness within a few weeks of starting Spironolactone.
Topical treatments
Topical antibiotics are highly effective at reducing the prevalence of acne-causing bacteria on the skin. Commonly prescribed topical antibiotics include erythromycin and clindamycin. Winlevi is a topical treatment containing clascoterone, an androgen blocker that inhibits the skin’s production of excess sebum. Topical retinoids are often prescribed for back acne. Like oral isotretinoin, topical retinoids are vitamin A derivatives that accelerate skin cell turnover, reduce inflammation, and prevent clogged pores. Commonly prescribed retinoids include tretinoin and tazarotene.
Tretinoin for back acne
Tretinoin is a prescription retinoid often used to treat acne. Retinoids and retinoid-like products, such as tretinoin, are skincare products derived from vitamin A that work by exfoliating dead skin cells from the epidermis, the outermost layer of the skin. Dead skin cells, sebum, and debris are shed at an increased rate, preventing them from becoming trapped in pores and causing acne. Tretinoin can be prescribed by a board-certified dermatologist, such as Dr. Green, to help combat back acne and achieve clearer, smoother skin.
Salicylic acid for back acne
Salicylic acid is a common ingredient in acne skincare products. It promotes skin exfoliation by clearing pores of excess oil and dead skin cells. This acne-fighting ingredient appears in various skincare products, including cleansers, exfoliants, toners, and moisturizers. Using a salicylic acid cleanser or toner pad after working out helps prevent sweat from clogging pores. The Pore Minimizing Cleanser and the Retexturizing Pads from MGSKINLABS both contain salicylic acid and glycolic acid to gently exfoliate the skin, helping prevent clogged pores and acne breakouts.
Benzoyl peroxide for back acne.
Benzoyl peroxide is a highly effective ingredient for fighting acne, as it dries out active lesions, reduces inflammation, and kills the bacteria that cause acne. Benzoyl peroxide is found in certain face and body washes and spot treatments. MGSKINLABS’ Acne Spot Treatment contains 5% benzoyl peroxide to shrink and eliminate blemishes from the skin.
Glycolic acid for back acne
Glycolic acid can significantly improve back acne due to its exfoliating properties. As an alpha hydroxy acid (AHA), it gently removes dead skin cells from the skin’s surface. This helps unclog pores, reduce breakouts, and promote cell turnover, leading to smoother, clearer skin over time. Additionally, glycolic acid has anti-inflammatory effects that may help soothe redness and irritation associated with acne, making it a beneficial choice for those struggling with back acne. The Pore Minimizing Cleanser and the Retexturizing Pads from MGSKINLABS both contain salicylic acid and glycolic acid to gently exfoliate the skin, helping prevent clogged pores and acne breakouts. However, regular use should be approached with caution; it’s advisable to start with a lower concentration and gradually increase it, while also applying adequate sun protection, as AHAs can increase the skin’s sensitivity to sunlight.
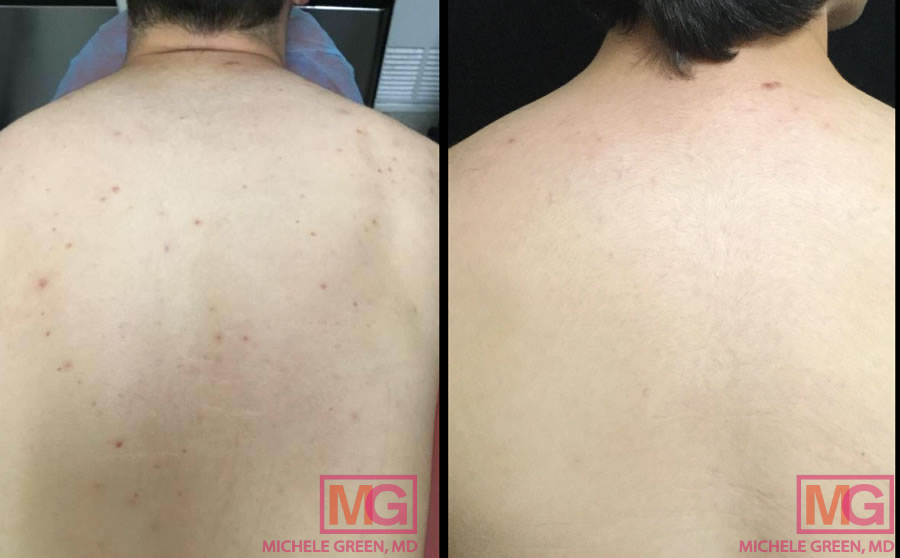
The best skincare for back acne
Cleansers and exfoliators for acne
Cleansing the skin is a crucial step in any acne skincare routine. Using a cleanser or body wash regularly helps reduce the buildup of dead skin cells, oil, dirt, sweat, and other impurities, preventing clogged pores. Glycolic acid and salicylic acid, two hydroxy acids, work together to gently exfoliate and dissolve excess oil, helping treat and clear your acne. The Pore Minimizing Cleanser from MGSKINLABS, Dr. Green’s proprietary skincare line, contains both glycolic and salicylic acid to clean pores and help prevent acne breakouts thoroughly.
Exfoliation is the process of removing dead skin cells and other impurities from the skin to clear pores and reveal fresh, healthy skin underneath. Patients can use an exfoliant two to three times a week or as needed to prevent bacne. The Retexturizing Pads from MGSKINLABS contain glycolic and salicylic acid to provide an at-home peel effect, exfoliating dead skin cells and preventing pore blockages to help stop acne.
Acne spot treatments
Spot treatments contain potent acne-fighting ingredients to target and eliminate active blemishes. Many include benzoyl peroxide, an antibacterial agent that kills the bacteria responsible for acne. MGSKINLABS’ Acne Spot Treatment contains 5% benzoyl peroxide and can be used as needed to reduce oil production, decrease inflammation, and shrink pimples.
Moisturizer
Regardless of skin type, a moisturizer is an essential component of any skincare routine, particularly for individuals with oily or acne-prone skin. While most people believe acne only occurs on oily skin, it can also happen on dry skin due to the body’s overproduction of sebum. Light, oil-free moisturizers are essential for acne-prone skin, as they help keep the skin hydrated while preventing clogged pores. MGSKINLABS’s Ultimately Sheer Hydrating Lotion is ideal for individuals with sensitive skin, as it helps control oil production, reduce excess sebum, and leave a matte finish, making it ideal for acne-prone skin.
Sunscreen
Another essential part of a good skincare routine is using sunscreen. Choosing a non-comedogenic sunscreen is ideal for those with oily or acne-prone skin. Dr. Green’s MGS, Inc. offers a non-comedogenic Hydrating SPF 50 that combines a moisturizer and SPF into one product. This type of sunscreen is ideal for individuals who want to maintain their skin’s hydration and radiance while protecting against UV rays that can lead to skin cancer and premature aging. Sunscreen should be reapplied every 90 minutes or after any water activities.
How do I stop my acne from coming back?
In addition to in-office treatments, oral medications, and prescription topical creams, patients can make lifestyle changes to reduce the risk of bacne. One way to prevent back acne is to improve hygiene, especially during workouts and other activities that cause sweating. Patients should wear moisture-wicking, loose-fitting clothing during exercise to minimize sweat trapped on the skin’s surface. It is also important to shower as soon as possible after working out to wash away any remaining sweat and help prevent clogged pores. If showering immediately isn’t possible, using cleansing wipes to remove sweat before changing out of sweaty workout clothes is recommended. Reducing friction can also help prevent back breakouts. Instead of wearing a backpack, try an over-the-shoulder or rolling bag to lessen friction from strap contact. Mental and emotional health is also essential for overall wellness. Stress can lead to hormone imbalances, which may increase sebum production. Whenever possible, find ways to reduce stress and anxiety to lower the chances of acne breakouts. If severe acne persists despite using recommended over-the-counter products and routines, it is best to consult a board-certified dermatologist. An experienced dermatologist, such as Dr. Green in NYC, can identify the root causes and recommend the most effective treatment options for your skin.
Will exfoliating help back acne?
Exfoliating can help manage back acne by removing dead skin cells that clog pores and contribute to breakouts. However, it’s important to approach it with care to avoid irritation. It’s recommended to exfoliate once or twice a week, using a gentle scrub or chemical exfoliant based on your skin type and sensitivity. Over-exfoliating can cause redness, inflammation, and more acne, so moderation is key. Additionally, combine exfoliation with other acne-fighting treatments and a proper skincare regimen for the best results.
Do pimple patches work on back acne?
A pimple patch is an over-the-counter product designed to cover active acne lesions. Some patches contain hydrocolloid, a wound-healing ingredient that absorbs excess fluid and oil from whiteheads, forming a gel that is trapped in the bandage and kept away from the skin, turning the patch white. Other patches contain chemical exfoliants, such as salicylic acid or glycolic acid, to kill acne-causing bacteria while gently exfoliating the skin. Pimple patches can be helpful because they prevent you from touching the acne, allowing it to heal properly and helping you resist the urge to pick or pop it. While pimple patches are effective for whiteheads, they tend to be less effective for cysts and blackheads. If you’re dealing with back acne, it’s important to see a board-certified dermatologist, like Dr. Green in NYC, who can help you understand the different types of lesions on your back and treat them most effectively.
Will back acne result in scarring?
When acne breakouts go untreated, inflammatory lesions can irreparably damage the underlying skin tissue, leading to permanent acne scars. These scars are much harder to treat than the acne itself and can appear as either hypertrophic (raised) or atrophic (depressed). Most acne scars won’t disappear on their own because they result from permanent skin damage. However, various non-invasive cosmetic treatments can significantly improve the appearance of acne scars, restoring an even, smooth skin texture and enhancing self-confidence. The first step in addressing acne scars is to schedule an appointment with a board-certified dermatologist, such as Dr. Michele Green in NYC, to identify the most effective treatment for your skin type, tone, and the specific scars you have.
How to treat back acne scars
One of the main reasons to see a dermatologist promptly for acne breakouts is to prevent scarring. Acne scars form when inflammation from lesions permanently damages the skin beneath. Although scar treatment is more difficult than treating active acne, options are available. The V-Beam, eMatrix, and Fraxel lasers, as well as chemical peels, are among the most effective treatments available at the office of board-certified dermatologist Dr. Michele Green for improving the appearance of back acne scars and reducing redness. When you consult with Dr. Green about your back acne or scars, she will work with you to create a personalized treatment plan based on your specific needs.
The V-Beam laser is considered the gold standard for treating redness, including that caused by acne scars. It uses pulsed dye light, which is converted into heat and absorbed by the skin’s red pigment, leaving surrounding tissue unharmed. The V-Beam laser is effective for various skin types, including sensitive skin, and is suitable for both atrophic and hypertrophic scars. It can also improve the appearance of broken blood vessels, rosacea, and stretch marks, among other concerns. The procedure is quick, involves minimal downtime, and is generally painless.
The Fraxel Dual laser is considered one of the most effective options for treating atrophic acne scars. Fraxel uses two different wavelengths, 1550 nm and 1927 nm, to target both uneven skin texture and tone. While the surface layers of the skin remain intact, the middle layers receive controlled, microscopic injuries that stimulate the skin’s natural healing process, encouraging the production of new collagen and elastin. When using the 1550 nm setting, patients can expect less visible acne scars and clearer, smoother skin. The most common side effects are usually mild, such as inflammation or redness, which typically last for the first 48 hours after treatment.
The eMatrix laser is a popular choice for treating acne scars and is safe for patients of all skin tones and types. It uses radiofrequency technology to heat the dermis deeply, triggering the skin’s natural healing process and promoting collagen remodeling and new collagen growth. This new collagen helps create a smoother skin texture. It diminishes the appearance of use by using radiofrequency technology to heat deep into the dermis, triggering the skin’s natural healing process and promoting collagen remodeling and new collagen growth. The eMatrix laser has minimal downtime, with common side effects such as redness and peeling in the treated area, which typically last up to 48 hours.
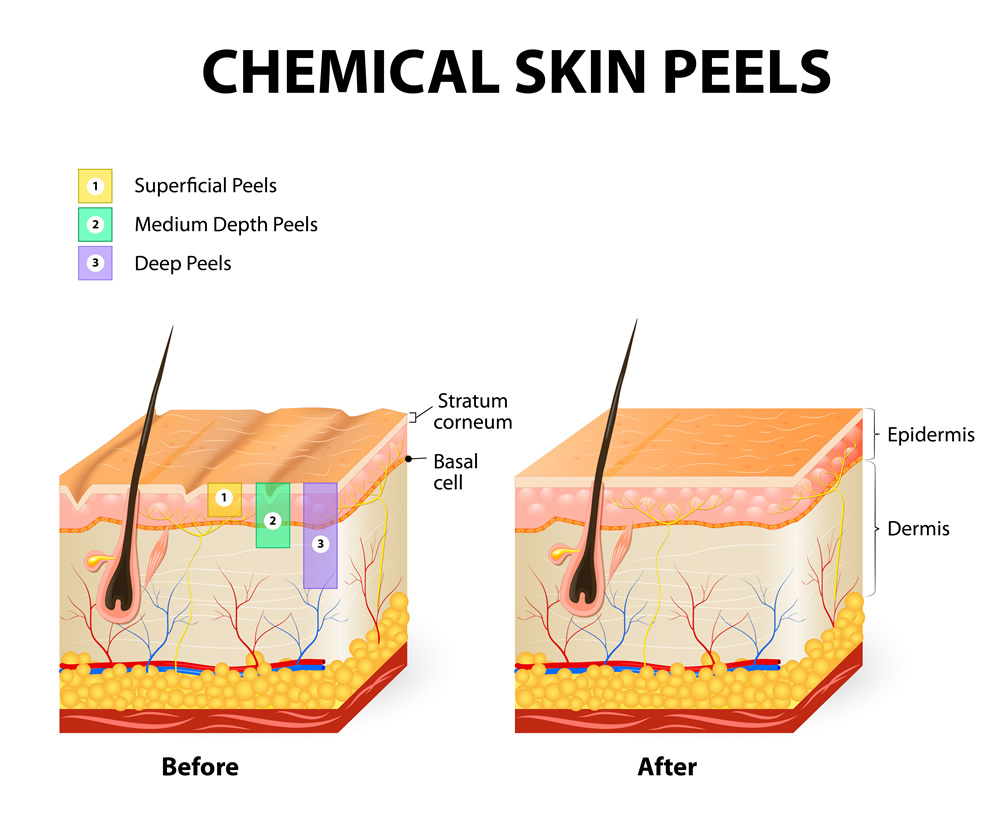
Chemical peels are cosmetic treatments designed to improve the appearance and texture of the skin. They involve applying a specialized solution that gently removes the outermost layers of skin. By removing dead skin cells, chemical peels help eliminate blemishes such as acne scars and dark spots and promote a brighter complexion. Additionally, this treatment stimulates collagen production, supporting skin elasticity and firmness. As a result, the underlying skin becomes healthier, smoother, and more radiant.
Mesopeels are specialized chemical peels designed to treat hyperpigmentation and post-inflammatory hyperpigmentation. Some patients may notice dark spots after an acne lesion has healed, which result from increased melanin production in the affected area. Mesopeels use skin-lightening agents, including kojic acid, azelaic acid, and tranexamic acid, to reduce unwanted hyperpigmentation and inhibit melanin production. They are safe for all skin types and tones and can be applied to various areas of the body, including the back, face, chest, inner thighs, and groin.
FAQs On Back Acne:
What type of acne is back acne?
There are many types of acne, and any of them can occur on the back. Some patients may experience a combination of blackheads, whiteheads, pustules, papules, cysts, and nodules. When seeking treatment for back acne, it is essential to consult a qualified dermatologist who can recommend the most suitable treatment for your specific type of acne.
Where do back pimples come from?
Several factors can contribute to back acne, including biological and lifestyle factors. Biological factors might include family history or hormonal changes. Lifestyle factors encompass hygiene, skincare routines, diet, medication use, and stress levels. Maintaining good hygiene and a proper skincare routine can significantly reduce the risk of developing bacne. Behaviors that may contribute to bacne include wearing tight clothing, having sweaty skin, not showering immediately after workouts, not washing clothes between workouts, and eating a diet high in glycemic-index foods. Adopting skin hygiene habits can significantly reduce the risk of acne.
Is back acne normal during pregnancy?
Pregnancy acne is very common, with over fifty percent of pregnant women developing it, usually starting around the sixth week of pregnancy. During the first trimester, your body produces more progesterone, which increases sebum—the oil produced by the sebaceous glands that lubricates the skin and hair. While sebum production is natural, excess oil can clog pores, leading to acne outbreaks or worsening existing acne. Therefore, pregnancy itself does not directly cause acne; however, hormonal changes during pregnancy can trigger skin changes that often lead to acne. A history of acne or flare-ups at the start of your menstrual cycle is another risk factor for developing acne during pregnancy. To help manage back acne during pregnancy, it’s essential to follow a consistent skincare routine, avoid harsh chemicals, and consult with an experienced dermatologist for personalized advice to keep your skin clear and healthy.
Is back acne the same as chest acne?
Yes, back acne is the same as chest acne. Back acne refers to acne vulgaris on the back, while chest acne refers to acne vulgaris on the chest. Both types of acne are caused by factors such as genetics, hormonal fluctuations, and lifestyle habits, including poor diet and inadequate hygiene. Body acne is often linked to hygiene issues, such as not showering after workouts, wearing tight clothing, and not washing clothes frequently. Back and chest acne can often be controlled with targeted skincare, topical prescriptions, oral medications, and in-office treatments.
Can steroids give you back acne?
Certain medications may increase your risk of developing back acne breakouts, including corticosteroids and anabolic steroids, both of which are sometimes shortened to “steroids.” Corticosteroids are medications used to reduce inflammation in the body. They can be applied locally via injection, cream, or gel, or taken systemically by mouth. Corticosteroids can stimulate androgen production, potentially leading to increased sebum production. Anabolic steroids are synthetic versions of testosterone that promote muscle growth and development and increase sebum production. With more sebum on the skin’s surface, the risk of clogged pores and back acne breakouts is higher.
Does back acne mean high testosterone?
While back acne isn’t directly caused by high testosterone, elevated testosterone levels can lead to back and facial acne. Hormonal shifts, which can occur at any time, are a major risk factor for developing back acne. Testosterone is a hormone found in both men and women and plays a role in several aspects of health, including bone density, sex drive, and fertility. Studies have shown that individuals with higher testosterone levels are more likely to experience acne breakouts. Excess testosterone can stimulate increased sebum production, raising the risk of clogged pores and acne.
Can creatine cause back acne?
Creatine is a peptide that enhances athletic performance by accelerating muscle recovery and promoting water retention. Although the body naturally produces creatine, it can also be taken as a supplement, enabling athletes to train longer. There is currently no known link between creatine and acne breakouts. However, increased physical activity can increase sweating, potentially increasing the risk of bacne. To prevent breakouts, people should wear breathable clothing during exercise and shower promptly afterward.
Will the sun help with acne?
Many patients believe that sun exposure helps clear acne, but in truth, the sun’s rays can dry out the skin, prompting it to produce more oil to replace the lost moisture. Excessive oil production from overactive sebaceous glands can clog pores, leading to breakouts. UV rays can also cause serious skin damage, leading to hyperpigmentation such as sunspots, age spots, melasma, and freckles, and increasing the risk of skin cancer.
Wearing sunscreen outdoors is essential for reducing the risk of bacne. Patients should choose a non-comedogenic, broad-spectrum sunscreen that they can apply regularly and consistently. A non-comedogenic skincare product won’t clog pores. The sunscreen should have a minimum SPF of 50 and be reapplied every 90 minutes when outdoors, with a thorough rinse at the end of the day to maintain clear, acne-free skin. Dr. Green’s specialty skincare line, MGSKINLABS Inc., offers a non-comedogenic Hydrating Sunscreen with SPF 50 that also functions as a moisturizer. This type of sunscreen is ideal for individuals seeking to streamline their skincare routine, maintain healthy, moisturized skin, and protect against harmful UV rays, which can lead to skin cancer and premature aging.

How often should I shower if I have back acne?
Patients with back acne should shower daily to prevent the buildup of dead skin cells, sebum, dirt, and other impurities. It is especially important to shower after exercising or heavy sweating to minimize the risk of sweat clogging pores. Patients can use a salicylic acid or benzoyl peroxide cleanser in the shower to gently exfoliate the skin, reduce acne-causing bacteria on the surface, and help prevent back acne.
Can you get a tattoo with back acne?
According to tattoo artists and healthcare professionals, patients should wait to get a back tattoo until their back acne has cleared. Back acne creates an uneven surface for the artist and can increase the risk of infection and spread acne bacteria from one area to another. If you are prone to back acne, seek treatment before scheduling any tattoo appointments.
Is body acne normal?
Yes, back acne is very common, affecting millions of people worldwide. Although acne isn’t a serious health issue, it can be frustrating and painful. Fortunately, many treatments are available to improve bacne. When dealing with any type of acne, the best first step is to consult a dermatologist, such as Dr. Green, for a personalized treatment plan. It is crucial to treat acne breakouts promptly to prevent scarring, which is often more difficult to treat than the initial breakouts. When you consult with Dr. Green on the Upper East Side of NYC, she will customize a treatment plan for your specific back acne to help eliminate it for good and achieve clear, radiant skin.
Is back acne unattractive?
The presence of Back acne does not define attractiveness, but those experiencing it may feel self-conscious and less confident. Treatments such as acne surgery, HydraFacials, VBeam laser, oral medications, and topical creams can help manage and clear breakouts, restoring confidence. When you consult with expert board-certified dermatologist Dr. Michele Green in NYC, she will create a back acne treatment plan to help you look and feel your best again.
Why do back pimples hurt so much?
Back pimples can develop due to a genetic predisposition to increased sebum production or hormonal fluctuations that increase sebum production. Often, back pimples arise from poor hygiene practices, including not showering after sweating or exercising, re-wearing damp clothes, or wearing tight-fitting clothing. When dead skin cells, sweat, dirt, and sebum are trapped in pores, back pimples can develop. Bacteria can also become trapped in pores, resulting in inflammation and infection. These types of pustules, papules, and cysts on the skin can be painful due to the underlying inflammation. Treatment with topical or oral medications, or with corticosteroid injections, can help shrink and eliminate the lesion, reducing associated pain.
Is back acne dangerous?
Back acne, also known as acne vulgaris, is generally considered a non-life-threatening condition; however, it can pose significant problems when it becomes severe, persists, or goes untreated. When inflamed lesions develop, such as painful cysts or nodules, they can damage surrounding skin tissue, leading to permanent scarring or changes in skin texture and pigmentation. These outcomes can be particularly challenging to address and often require more intensive treatment than the original acne itself. In addition to physical complications, deep or infected lesions can cause considerable discomfort, including tenderness, inflammation, and swelling, which may hinder daily activities and overall quality of life. For these reasons, seeking professional treatment at the earliest signs of back acne is crucial. Early intervention can help reduce inflammation, minimize the risk of long-term skin damage, and ultimately enhance overall skin health.
Will tanning help back acne?
Tanning is often seen as a quick fix for acne because the temporary darkening of the skin can mask redness and blemishes. However, this approach does not address the root causes of acne and may worsen the condition over time. While ultraviolet (UV) light may initially dry the skin, reducing oiliness briefly, this dryness can trigger the sebaceous glands to overcompensate by producing even more oil. Excess oil can clog pores, increasing the risk of new breakouts and worsening existing acne. Furthermore, UV exposure can contribute to several long-term skin issues, including post-inflammatory hyperpigmentation—a condition in which dark spots form in areas of previous inflammation, such as acne lesions. This can result in an uneven skin tone, making acne marks more pronounced over time. Instead, it is recommended to use a broad-spectrum, non-comedogenic sunscreen to protect the skin from harmful UV rays while preventing clogged pores.
Why is back acne caused?
Back acne occurs when hair follicles become clogged with excess oil, dead skin cells, and bacteria. Several factors contribute to its development, including hormonal changes—such as those during puberty, menstruation, or hormonal therapy—dietary choices, and lifestyle factors such as stress and sweating. Additionally, tight clothing or backpacks can create friction on the skin, further exacerbating the problem. Understanding these causes can help individuals manage and reduce back acne.
Will sunburn get rid of back acne?
While some people believe sun exposure can clear acne, a sunburn can actually worsen back acne. Sunburn irritates the skin, increasing inflammation and making existing blemishes more prominent. Additionally, sun exposure can increase skin oil production in response to irritation, potentially worsening acne rather than improving it. It’s important to protect the skin with sunscreen and maintain a proper skincare routine to manage back acne effectively.
Will sunbeds help with back acne?
Using sunbeds to treat back acne is not recommended. While some believe tanning can improve acne’s appearance, UV exposure can cause skin irritation and inflammation, which may worsen the condition. The heat from sunbeds can also exacerbate clogged pores, a common contributor to acne breakouts. Additionally, public sunbeds may not be properly sanitized, which can spread bacteria and lead to further skin issues. Instead of using tanning beds, consider other acne treatments, such as topical medications, or consult a dermatologist, who can provide safer, more effective options for managing back acne.
Will sleeping without a shirt help with back acne?
Sleeping without a shirt may reduce friction and irritation on the back, which can help improve back acne. When you sleep in clothing, the fabric can cause constant friction against your skin, which may worsen acne caused by friction, sweat, or the buildup of oils on the skin’s surface. By eliminating this layer of clothing, you allow your skin to breathe more freely, potentially decreasing the likelihood of breakouts in those areas. As an alternative, you can try sweat-wicking fabrics, engineered materials that draw moisture away from the skin through capillary action, moving it to the garment’s outer surface for rapid evaporation.
However, it’s important to note that back acne can arise from a variety of factors, not just friction. Conditions such as hormonal imbalances, genetic predispositions, and excessive oil production can also play significant roles. Sleeping shirtless may not directly address these underlying causes, especially if the acne is linked to hormonal changes or family history. To effectively combat back acne, it’s crucial to consult with a board-certified dermatologist like Dr. Michele Green.
Will my back acne go away?
Yes, back acne, also known as bacne, is not permanent and can clear up with the right approach. Establish a consistent skincare routine tailored to your skin type. Use gentle cleansers to remove excess oil and bacteria, and exfoliate to unclog pores. Treat active breakouts with products containing salicylic acid or benzoyl peroxide. Maintaining a healthy lifestyle is equally crucial. Stay hydrated, eat a balanced diet rich in vitamins and minerals, and wear breathable fabrics to help minimize flare-ups. If your back acne persists despite these efforts, consider consulting a dermatologist for personalized advice and potential prescription treatments. With dedication and the right care, you can achieve clearer skin over time.
How to get started with back acne treatment today
Back acne is a skin condition that can be challenging to treat and may lead to self-consciousness and low self-esteem. Visiting a board-certified dermatologist as soon as back acne develops is crucial to prevent acne scars, which can be harder to treat than the breakouts themselves. If you’re struggling with back acne, prevention strategies and treatment options are available, including acne surgery, HydraFacials, VBeam laser, and oral and topical medications to help manage and treat breakouts. Scheduling a consultation with an acne expert, such as Dr. Michele Green in NYC, is the best way to understand and manage your breakouts and help you achieve clear, acne-free skin.
Dr. Michele Green, in New York City, is an internationally renowned, board-certified dermatologist with over 2.5 decades of experience providing customized acne scar and acne treatment plans to some of the world’s most discerning individuals. Taking a holistic approach to back acne treatment, Dr. Green will recommend a personalized combination of specially formulated skincare products, prescription treatments, and in-office therapies to help you achieve a healthy, clear, radiant, and pimple-free complexion that lasts. Dr. Green is recognized by Castle Connolly, Super Doctors, and New York Magazine as one of the top dermatologists in New York City for her dedication to patient care and expertise. To get started on eliminating your back acne once and for all, call 212-535-3088 or contact us online today to schedule a consultation with Dr. Green at her private dermatology office in Manhattan’s Upper East Side.
 212-535-3088
212-535-3088 



