Fungal Acne Treatment
Fungal acne treatment is often sought by patients frustrated by persistent clusters of small, uniform bumps that do not improve with traditional acne products. Unlike typical acne, which stems from clogged pores and bacteria, fungal acne results from an overgrowth of yeast in the hair follicles, so many standard cleansers and spot treatments offer little relief. When fungal acne appears on visible areas such as the forehead, hairline, or cheeks, it can make the skin look uneven and textured, affecting confidence and comfort. The bumps are often itchy, red, and resistant to common over-the-counter acne medications, leaving patients discouraged after trying multiple products without success. Breakouts on the chest, shoulders, or back can make patients more self-conscious, particularly during warmer months or when wearing fitted clothing. For individuals seeking clear, smooth skin after repeated frustration with ineffective treatments, targeted fungal acne therapy with Dr. Michele Green can provide meaningful improvement.
Fungal acne treatment works by reducing excess yeast on the skin and calming inflammation in the affected hair follicles. Carefully selected topical antifungal medications lower yeast levels and smooth the small, clustered bumps caused by this condition. For more widespread or persistent breakouts, additional oral prescription may be recommended to help achieve optimal clearing. Treatment plans are customized based on the severity of the flare, the areas involved, and the patient’s skin type to ensure safe and effective results. Supportive skincare also plays an essential role, including lightweight, non-occlusive products that help maintain balance without trapping heat or excess oil. A board-certified dermatologist, such as Dr. Michele Green, will tailor your fungal acne treatment plan to restore clarity, comfort, and overall skin health.
Dr. Michele Green is an internationally recognized, board-certified dermatologist with over 25 years of experience treating a wide range of medical and cosmetic skin concerns, including persistent and recurrent fungal acne. She is consistently ranked among New York City’s top dermatologists by Castle Connolly, Super Doctors, New York Magazine, and The New York Times for her expertise and dedication to patient care. Dr. Green takes a meticulous, individualized approach to diagnosis, ensuring fungal acne is accurately identified and distinguished from other types of breakouts before treatment begins. Her experience managing yeast-related folliculitis enables her to create precise, personalized treatment plans that clear the skin efficiently while supporting long-term balance. When you schedule a consultation at her private boutique dermatology practice on Manhattan’s Upper East Side, Dr. Green will work closely with you to develop a customized treatment and skincare strategy that helps you achieve clear, healthy, and confident skin.
What is Fungal Acne?
Fungal acne, also known as Pityrosporum folliculitis or Malassezia folliculitis, is a condition characterized by an overgrowth of yeast on the skin that can lead to folliculitis, an infection of the tiny hair follicles. This infection results in small lesions or red bumps that resemble regular acne. Fungal acne can occur anywhere on the body but is most commonly seen on the chin, forehead, hairline, sides of the nose, arms, upper back, and shoulders. Although anyone can develop fungal acne, it is most prevalent among young adults, particularly those with oily skin, where yeast tends to thrive.
Fungal acne appears as clusters of uniform papules that are often itchy. It resembles regular acne but is distinct. Bacterial acne primarily results from clogged pores caused by oil and dead skin cells, whereas fungal acne is caused by a yeast infection in the pores. Additionally, whereas traditional acne can manifest as comedones (blackheads and whiteheads), pustules, or cysts, fungal acne typically does not. Treating fungal acne with products meant for bacterial acne can worsen the infection. Therefore, it is crucial to have fungal acne diagnosed by an expert dermatologist, such as Dr. Michele Green in New York City.
Where does fungal acne come from?
Fungal acne results from an overgrowth of yeast on the skin. This yeast, known as Malassezia, is naturally present on your skin alongside various types of bacteria. Under normal circumstances, yeast and bacteria maintain a balance on the skin. However, if yeast growth surpasses bacterial levels or if bacteria are reduced (for instance, due to antibiotic use), folliculitis—a hair follicle infection—can occur, leading to fungal acne. Malassezia proliferation is enhanced in warm, moist environments, which is one of several risk factors for the onset of fungal acne. Additionally, the yeast on your skin feeds on the oils and sebum produced, making fungal acne more prevalent on oily skin or in areas with high oil production.
Where is fungal acne most common?
Fungal acne most commonly appears in areas where sweat and oil accumulate throughout the day. These regions often include the upper back, chest, shoulders, and sometimes the upper arms. These areas are frequently covered by clothing, which can trap warmth and moisture, leaving the skin damp for extended periods. People who exercise regularly or live in humid climates may notice that these areas are especially prone to small clusters of bumps after physical activity. Because these regions also contain a higher concentration of hair follicles, they provide more opportunity for yeast-related inflammation to develop.
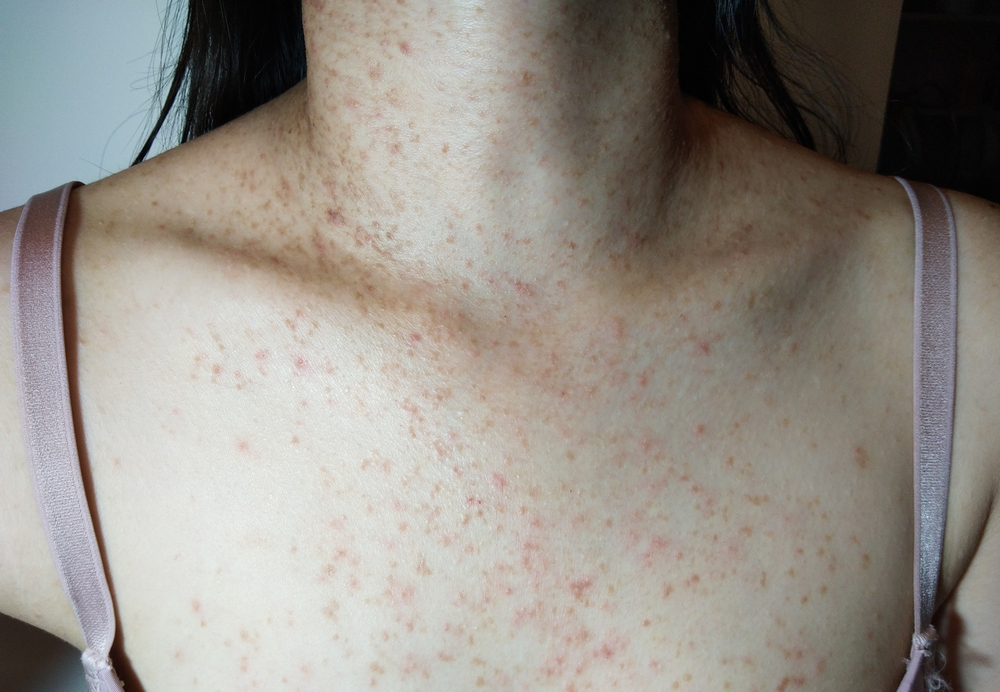
What are the risk factors for developing fungal acne?
Many risk factors can lead to the development of fungal acne. Patients living in hot, humid climates are at higher risk, as yeast thrives in warm, moist environments. Similarly, yeast can overgrow in areas where moisture is trapped. Patients who sweat excessively, wear tight clothing, or remain in sweaty garments for extended periods are also at increased risk of developing fungal acne. Fungal acne can be a side effect of certain medications. For instance, oral antibiotics are prescribed to eliminate the bacteria that cause illness, but they can also eradicate the “good” bacteria on your skin. When these beneficial bacteria are diminished, it creates an imbalance between the bacteria and yeast on your skin, which can heighten the risk of developing Malassezia (pityrosporum) folliculitis. Diet also plays a significant role in the development of fungal acne. Yeast and fungi thrive on carbohydrates and sugars to survive. Patients face a higher risk of developing fungal acne if their diets are high in sugars and carbohydrate-rich foods, such as sugary breakfast cereals, soda, baked goods, and fruit juice. Lastly, the risk of developing fungal acne increases if you have an immunosuppressed or weakened immune system. If you are immunodeficient, your body has a reduced ability to combat various infections, including fungal infections, and you are at risk for developing fungal acne.
How to tell the difference between fungal and bacterial acne
Fungal and bacterial acne on the skin can be difficult to distinguish for an untrained eye. Nevertheless, some characteristics can help differentiate the two. Fungal acne usually appears clustered in one specific area of the face but can also develop on the chest, arms, shoulders, upper arms, and upper back. In contrast, bacterial acne typically appears randomly across the face and does not usually develop in other body areas. Additionally, fungal acne is often pruritic or itchy, which is not commonly the case with bacterial acne. Ultimately, the best way to distinguish between bacterial and fungal acne is to have diagnostic testing performed by a board-certified dermatologist like Dr. Green. In addition to a culture, a gentle skin scraping may be performed to examine the skin under a microscope and confirm the presence of yeast. The sample will then be cultured to determine whether a fungal or bacterial infection causes the acne.
How to tell if I have fungal acne?
Many patients initially mistake the spots for typical acne, which is caused by clogged pores filled with oil and dead skin cells. However, it is crucial to differentiate between typical acne and fungal acne, as the treatments for each are significantly different. While typical acne can often be treated with a salicylic acid cleanser, merely clearing and exfoliating the pores is usually not enough to treat fungal acne. If you are experiencing an acne breakout and are uncertain whether it is fungal, consult board-certified dermatologist Dr. Green. She will evaluate your medical history and likely order blood tests and a fungal or bacterial culture to identify the type of acne you have. In rare instances, a biopsy of the area may be performed and sent to a laboratory for further analysis. Once a diagnosis is confirmed, she can prescribe topical or oral medications best suited to address your acne breakouts.
Will fungal acne go away on its own?
Fungal acne generally does not clear completely without treatment, even when the breakout does not appear severe. One reason is that it is often mistaken for regular acne, leading many patients to continue using products not designed to address yeast overgrowth. When untreated, the bumps can persist and remain itchy or irritated, particularly in areas with higher oil production. Some people may try to manage it by washing more frequently or switching skincare products, yet these changes alone are rarely enough to eliminate the underlying issue. Because the condition is driven by yeast rather than clogged pores or bacteria, it typically requires targeted therapy to fully resolve. Without proper treatment, the breakout often persists and can interfere with overall skin clarity and comfort.
How do you get rid of fungal acne breakouts?
There are several effective treatment options for fungal acne, including topical antifungal creams and oral medications. If you suspect the pimples on your face are fungal acne, you can schedule a consultation with Dr. Green. During your appointment, she will review your medical history and may order blood work and cultures to confirm a diagnosis. She will then prescribe the most appropriate products to treat your fungal acne. It is essential to obtain a proper diagnosis of fungal acne, as treating it like a typical acne breakout with regular acne medication can worsen it.
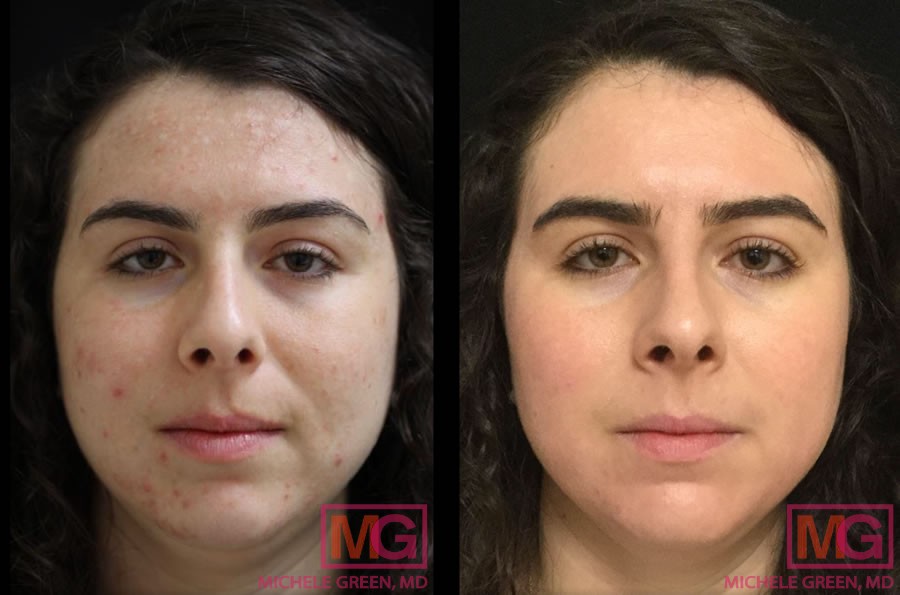
Acne treatments – 8 months
The following are common treatment options for fungal acne prescribed by board-certified dermatologist Dr. Michele Green in her private NYC dermatology practice:
Ketoconazole cream
Ketoconazole is an antifungal that has proven highly effective in alleviating the symptoms of fungal acne. A 2020 study comparing patients using a 2% Ketoconazole cream with those receiving a placebo for fungal acne found that nearly 50% of participants using the cream experienced improvement. In addition to the 2% cream, Ketoconazole is also available as a shampoo, commonly known as Nizoral, which can be applied to the body as directed daily.
Nizoral shampoo
Nizoral shampoo is an antifungal dandruff shampoo that can also help reduce fungal acne when applied to the skin. It can be used as a body wash in the shower every other day to treat active fungal acne. Once the skin condition clears, you may follow the same procedure with the shampoo once a week to prevent fungal acne from recurring and to maintain healthy, clear skin. Ketoconazole is an effective topical treatment for eliminating fungal acne while remaining gentle on the skin. The treatment can also be combined with prescription oral medication for additional support if necessary.
Oral medications to treat fungal acne
Fluconazole and Itraconazole are two oral prescription medications used to treat fungal and yeast infections. They are generally prescribed when topical treatments have not fully eliminated fungal acne. To effectively treat fungal acne breakouts, Fluconazole and Itraconazole are often paired with a topical antifungal cream, such as Ketoconazole or Clotrimazole. Monthly blood tests are needed to monitor liver enzymes while patients take these oral antifungal medications.
Can over-the-counter products for regular acne treat fungal acne?
Over-the-counter acne products formulated for typical acne vulgaris are generally ineffective for treating fungal acne, medically known as Malassezia folliculitis. Traditional acne treatments such as benzoyl peroxide and salicylic acid are designed to reduce bacteria, clear clogged pores, and decrease inflammation from excess oil and dead skin cell buildup. Fungal acne develops differently, driven by an overgrowth of Malassezia yeast within the hair follicles rather than bacteria. Because these common acne ingredients do not target yeast, they do not address the underlying cause of fungal acne. In some cases, relying solely on standard acne products may delay improvement and prolong irritation, especially with heavier or oil-based formulations, which create a warm, occlusive environment that allows yeast to thrive. When breakouts are itchy and resistant to conventional acne therapy, evaluation by a board-certified dermatologist is essential to confirm the diagnosis and initiate appropriate antifungal treatment.
What skincare is best for fungal acne?
The best skincare approach for fungal acne focuses on reducing yeast overgrowth while supporting a balanced skin barrier. Antifungal ingredients such as ketoconazole, selenium sulfide, or zinc-based formulations are often recommended to directly reduce Malassezia levels on the skin. These are available in prescription creams or medicated cleansers. Sweat and sebum can contribute to yeast proliferation, so using a gentle, non-irritating cleanser twice daily helps remove excess sweat and sebum without stripping the skin. Oil-free, lightweight moisturizers are preferred, since heavy, occlusive products can trap heat and moisture, potentially worsening flare-ups. Consistent hygiene habits, such as showering promptly after sweating and avoiding tight, non-breathable clothing, also support treatment outcomes. An individualized plan developed with a dermatologist ensures that both active antifungal therapy and daily skincare products work together to clear the condition and reduce the likelihood of recurrence.
How to manage fungal acne at home
There are several habits you can adopt at home to lower the risk of developing fungal acne. The first key factor in preventing fungal acne is maintaining good hygiene. By showering more frequently and promptly changing out of sweaty clothes after a workout, you minimize your exposure to the damp environment where yeast flourishes. During your shower, you can use Nizoral dandruff shampoo to help reduce the amount of yeast on your skin. Other dandruff shampoos that contain selenium sulfide or are designed to treat seborrheic dermatitis can work similarly. When shaving or waxing, it’s crucial to cleanse and hydrate the area to avoid skin irritation, which can create an opportunity for yeast overgrowth and fungal acne. Additionally, wearing loose clothing while exercising and opting for a breathable cotton face mask can be beneficial.
Changing your diet can help reduce fungal acne because yeast and fungi thrive on carbohydrates and sugars. While many foods contain carbohydrates, it’s essential to focus on complex carbohydrates rather than simple ones (those high in sugar). Limit high-sugar breakfast cereals, sodas, baked goods, and fruit juices, and incorporate more fruits, vegetables, legumes, and whole grains. Although these lifestyle changes can help reduce fungal acne, the most effective treatments remain topical and oral antifungal medications. If you suspect you have fungal acne, consult a board-certified dermatologist like Dr. Green for an accurate diagnosis and treatment plan.
What is the best way to get rid of fungal acne?
The best way to get rid of fungal acne starts with an accurate diagnosis, since treating it like traditional acne often delays improvement. Once Malassezia folliculitis is confirmed, management typically combines targeted antifungal therapy with lifestyle changes that limit factors that encourage yeast overgrowth. Topical antifungal creams, such as ketoconazole or similar prescription medications, are commonly used to reduce yeast levels within the hair follicles. In more widespread or stubborn cases, an oral antifungal medication may be recommended to address the condition from within. At the same time, supportive measures such as using gentle, oil-free skincare products, showering promptly after sweating, and avoiding heavy, occlusive creams can help prevent ongoing flare-ups. Addressing both the yeast overgrowth and the external triggers that contribute to it provides the best way to achieve clear skin. Because fungal acne can resemble other types of breakouts, evaluation by a board-certified dermatologist ensures that the treatment plan is appropriate and effective.
Why does fungal acne keep coming back?
Fungal acne tends to recur when the skin’s balance is disrupted. Yeast thrives in warm, moist, and oily environments, so anything that regularly increases heat, friction, or oil on the skin can contribute to repeated episodes. For example, frequent workouts without showering soon afterward, heavy hair products that spread onto the forehead, or thick facial creams that trap moisture can all create an ideal setting for yeast to multiply again. Repeated use of oral antibiotics can decrease certain protective bacteria on the skin, creating an imbalance that allows yeast to overgrow. When these triggers persist, the skin can cycle through periods of clearing and reappearance. Understanding and modifying these patterns is often key to reducing repeated flare-ups over time.
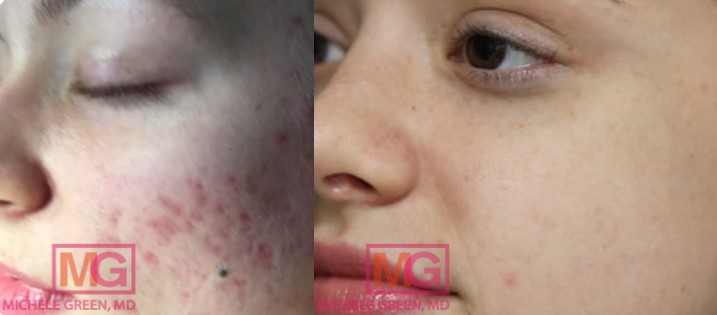
Laser treatment for acne – before and after
FAQs about Fungal Acne
What causes fungal acne?
Fungal acne results from an overgrowth of Malassezia yeast in the hair follicles, and several underlying factors can trigger this imbalance. Malassezia is part of the normal skin microbiome, and the condition arises when the yeast multiplies beyond normal levels. Warm temperatures, excessive sweating, and high humidity create an ideal environment for yeast growth, which is why flare-ups are more common in hot climates or after prolonged physical activity. Oily skin can also contribute, as yeast feeds on sebum, making areas such as the forehead, chest, and upper back more prone to breakouts. Certain medications, particularly oral antibiotics, may disrupt the natural balance between bacteria and yeast on the skin, allowing yeast to overgrow. Wearing tight or non-breathable clothing that traps heat and moisture against the skin can further increase risk. In some individuals, a weakened immune system may also make it easier for yeast-related folliculitis to develop. Fungal acne typically occurs when several of these factors combine, leading to inflammation within the hair follicles and the appearance of small, uniform, often itchy bumps.
Will fungal acne go away by itself?
Fungal acne is unlikely to resolve on its own because it is not simply a surface-level breakout but a form of folliculitis caused by an overgrowth of yeast within the hair follicles. Many patients assume that if they stop using active products or simplify their skincare routine, their skin will naturally rebalance. While reducing irritation can help the skin feel calmer, it does not eliminate the yeast causing the breakout. Without directly addressing that imbalance, the bumps usually persist. This is why fungal acne often persists despite efforts to calm the skin or avoid harsh ingredients. For the condition to fully clear, the yeast overgrowth must be properly managed, which typically requires guidance from a board-certified dermatologist.
Where does fungal acne appear on the face?
Fungal acne most often appears on the face in areas with higher natural oil production or where hair products and sweat accumulate. The forehead is a common site, particularly near the hairline, where styling products or natural scalp oils may transfer onto the skin. It can also develop along the sides of the nose, around the temples, or occasionally on the chin. Facial fungal acne tends to present as small, uniform bumps that cluster together rather than as isolated pimples. Because the face is more delicate and frequently exposed to cosmetics, sunscreen, and moisturizers, buildup from certain products may contribute to breakouts in these areas.
What helps fungal acne on the face?
When fungal acne appears on the face, treatment must be approached carefully, since facial skin is more delicate and often more reactive than the skin on the body. The goal is to reduce the overgrowth of Malassezia yeast while protecting the skin barrier and avoiding unnecessary irritation. On the face, lightweight antifungal creams, such as ketoconazole, or other prescription topical medications are commonly applied in thin layers to calm inflammation within the hair follicles. Harsh scrubs and aggressive exfoliation should be avoided, as they can disrupt the protective barrier of the facial skin and increase redness or sensitivity. Gentle cleansing twice daily helps remove excess oil and sweat that may contribute to flare-ups, especially along the hairline, forehead, and sides of the nose, where fungal acne is frequently seen. Oil-free, non-comedogenic moisturizers are also important, since facial skin still requires hydration even during treatment. Using heavy creams or oily makeup on the face can trap heat and sebum, which may worsen breakouts. Because facial skin is often more sensitive, evaluation by a board-certified dermatologist is especially important to confirm the diagnosis and create a treatment plan that clears the breakout while maintaining healthy, balanced skin.
Is benzoyl peroxide good for fungal acne?
When treating fungal acne, it is important to address the overgrowth of Malassezia yeast on the skin to reduce the outbreak. Benzoyl peroxide is an antibacterial treatment and is not typically prescribed to address yeast overgrowth. However, it can help unclog pores and exfoliate skin cells, reducing the amount of sebum, or oil, on the skin’s surface. The yeast responsible for fungal acne feeds on excess oil, so exfoliating the skin and reducing oil in the affected area, along with benzoyl peroxide, can be useful. If you are wondering which products will work best to address your fungal acne, it is best to consult a board-certified dermatologist, such as Dr. Michele Green in New York City.
Does salicylic acid remove fungal acne?
Salicylic acid is a beta-hydroxy acid that gently exfoliates the skin, removing dead skin cells, excess sebum, and other impurities from clogged pores. While it is excellent for treating typical acne, it is not intended for fungal acne, as it does not reduce yeast production on the skin.
Which shampoo is good for fungal acne?
Dandruff shampoos are highly effective at treating fungal acne on the body because of their antifungal properties. Nizoral shampoo contains ketoconazole, which disrupts and prevents yeast growth. Selsun Blue shampoo contains selenium sulfide, which produces pentathionic acid that kills yeast. Dandruff shampoos containing zinc pyrithione also inhibit yeast growth on the skin. These shampoos can be used as a body wash to control yeast production in areas affected by fungal acne.
What can cure fungal acne?
Fungal acne can be cleared with treatments that directly reduce the overgrowth of Malassezia yeast in the hair follicles. Because the condition is caused by yeast rather than bacteria, therapy must specifically target the yeast. Topical antifungal medications, such as ketoconazole or other prescription creams, are commonly used to reduce yeast levels on the skin and calm inflammation. When breakouts are more widespread or do not respond fully to topical therapy alone, an oral antifungal medication may be prescribed to address the condition more comprehensively. Medicated cleansers with antifungal ingredients can also be incorporated into a treatment plan, particularly for areas such as the chest or back. Successful treatment involves not only clearing active lesions but also maintaining a skincare routine that supports balance in the skin microbiome, including the use of lightweight, oil-free products and proper hygiene after sweating. With accurate diagnosis and targeted therapy guided by a board-certified dermatologist, fungal acne can be effectively resolved, and the skin can return to a clear, healthy appearance.
Will fungal acne keep coming back?
Fungal acne can recur in some individuals, especially when the factors that initially triggered the breakout persist. Because Malassezia yeast naturally lives on the skin, treatment should control its overgrowth. For many patients, once the active flare-up clears, the skin may remain clear for long periods. However, factors such as sweating, increased oil production, frequent gym activity without prompt cleansing, or extended time in hot, humid climates can make the skin more prone to another flare-up. Recurrence does not mean the original treatment failed. The yeast is part of the normal skin biome and can become overactive again under certain conditions. With consistent skincare habits and early treatment of new bumps, many people can keep flare-ups infrequent and manageable.
Can you pop fungal acne?
No, you should never pop a fungal acne lesion. Doing so can introduce bacteria into the area, increasing inflammation and irritation. It can also spread the infection to other areas and worsen the breakout. Additionally, popping or squeezing a lesion can cause permanent damage to the underlying tissue and result in scarring. If you are experiencing fungal acne, it is best to consult with board-certified dermatologist Dr. Green, who can eliminate your acne with targeted antifungal treatments and help you achieve clear, radiant skin.
Where is fungal acne located?
Fungal acne can develop wherever hair follicles are present, so it is not limited to one specific part of the body. While it often affects the torso, it may also appear along the neck, hairline, or near the scalp. In some individuals, it can appear in areas where backpacks, sports equipment, or tight garments create repeated friction against the skin. The bumps often cluster in a specific area. Where they appear can sometimes point to everyday factors, such as tight clothing, frequent sweating, or friction from straps and equipment, that may be contributing.
Will fungal acne go away without treatment?
Fungal acne typically does not resolve completely without proper treatment, especially when the yeast imbalance has already caused inflammation within the hair follicles. Even if the breakout appears stable and not worsening, it is not necessarily healing. Unlike minor skin irritation that may calm down with time, fungal acne often remains unchanged when left untreated. Patients frequently notice that the bumps stay relatively consistent in size and pattern. Fungal acne can be frustrating to treat because it may look less severe than inflammatory acne. In many cases, the condition persists until the yeast overgrowth is specifically addressed, which is why waiting it out is usually not enough to achieve full resolution.
Which treatment is best for fungal acne?
The best treatment for fungal acne depends on the severity of the breakout and the areas involved. For mild to moderate cases, a topical antifungal medication is often sufficient to reduce inflammation and clear the small, uniform bumps associated with yeast overgrowth. Medicated cleansers or shampoos with antifungal ingredients may also be used when larger areas are affected. If the condition is more extensive or does not respond to topical therapy alone, an oral antifungal prescription may be considered under medical supervision. The most appropriate treatment is individualized, taking into account factors such as skin type, medical history, and the location of the breakout. A tailored approach guided by a board-certified dermatologist allows for targeted therapy while minimizing unnecessary irritation and reducing the likelihood of recurrence.
Why is my fungal acne getting worse?
Fungal acne may appear to worsen when the skin is repeatedly exposed to heat, moisture, and friction, which allow yeast to multiply more rapidly. Extended workouts without showering soon afterward, tight clothing that traps sweat, or prolonged time in hot, humid environments can all intensify flare-ups. Applying thick or occlusive skincare products may also trap oil and heat against the skin, increasing inflammation and making the bumps more noticeable. In some individuals, increased oil production during periods of stress or hormonal shifts can further contribute to progression. When the number of bumps increases or itching becomes more intense, it often suggests the yeast is still overgrowing on the skin. Identifying and addressing these triggers is often key to preventing the breakout from escalating.
Why is fungal acne so hard to get rid of?
Fungal acne can feel difficult to get rid of because it does not always respond quickly, even with the correct treatment. Unlike a single pimple that may shrink within a few days, fungal acne often appears as clusters of small, similar-looking bumps that take time to calm down. The skin in the affected area may also remain slightly textured or uneven for a while, which can make it seem as though nothing is improving, even when inflammation is gradually decreasing. In addition, flare-ups may overlap, meaning new bumps can form before older ones have completely faded, creating the impression that the condition is not going away. Patience is often required, as visible improvement may take a few weeks to show. This slower response can make fungal acne feel more stubborn than other breakouts, even though it can be successfully managed with the right approach.
Why did I suddenly get fungal acne?
Fungal acne can seem to appear suddenly when a recent change disrupts the skin’s balance. Although Malassezia yeast normally lives on the surface of healthy skin, certain imbalances can allow it to multiply more rapidly and trigger inflammation within the hair follicles. A new workout routine that increases sweating, a vacation in a hot or humid climate, switching to heavier skincare products, or starting a course of oral antibiotics can all alter the skin’s environment. In some cases, increased oil production during periods of stress or hormonal fluctuation may also create conditions that favor yeast growth. Because these changes can happen quickly, the breakout may feel sudden and unexpected.
Why is my fungal acne not going away?
If fungal acne is not going away, one of the most common reasons is that it has been mistaken for regular acne and treated with products that do not address yeast overgrowth. Many standard acne treatments target bacteria or unclog pores, so they may have little effect on Malassezia-related breakouts. As a result, the bumps can remain visible even with a consistent skincare routine. In other cases, certain facial products, such as heavy creams, thick sunscreens, or oily hair products that come into contact with the forehead, may unintentionally contribute to ongoing breakouts. Even diligent cleansing may not fully resolve the issue if the yeast imbalance has not been specifically addressed. If fungal acne is not improving despite consistent efforts, it may mean that the treatment being used is not addressing the underlying cause.
What is the fastest way to get rid of fungal acne?
The fastest way to improve fungal acne is to confirm the diagnosis and start treatment that specifically targets yeast overgrowth. Because fungal acne does not behave like typical acne, using the wrong products can delay visible improvement. Once the appropriate treatment is started, many patients notice a reduction in redness and itching within the first couple of weeks, though full clearing may take longer depending on the severity of the breakout. Acting early, avoiding heavy or oil-rich skincare products, and keeping the affected area clean and dry can help speed recovery. Prompt treatment is important, as waiting too long gives the yeast more time to multiply and spread to nearby areas.

How can I get rid of fungal acne?
Fungal acne treatment focuses on reducing the overgrowth of Malassezia yeast in the hair follicles while restoring skin balance. Because fungal acne does not respond to traditional acne medications, therapy is tailored to target yeast and calm inflammation. Treatment may include topical antifungal medications, medicated cleansers, and, in certain cases, oral prescriptions when breakouts are more widespread. In addition to addressing active bumps, careful attention is given to skincare selection to avoid heavy or oil-based products that may aggravate the condition. With the right approach, fungal acne can be effectively cleared, leaving the skin smoother and visibly more even in tone and texture. An experienced board-certified dermatologist, such as Dr. Green in NYC, can accurately diagnose fungal acne and create a personalized treatment plan designed to restore clear, healthy skin.
Dr. Michele Green is an internationally acclaimed, board-certified dermatologist with more than 25 years of experience treating medical and cosmetic skin conditions, including stubborn and recurrent fungal acne. She is consistently recognized as one of New York City’s leading dermatologists by Castle Connolly, Super Doctors, New York Magazine, and The New York Times for her expertise and dedication to patient care. Dr. Green takes a thorough, individualized approach to evaluation and treatment. By carefully assessing each patient’s skin type, lifestyle factors, and previous treatments, she develops a plan tailored to eliminate fungal acne and maintain long-term skin health. When you schedule a consultation at her private boutique dermatology office on Manhattan’s Upper East Side, Dr. Green will work closely with you to achieve clear, balanced, and radiant skin. Please call (212) 535-3088 or contact the office online to schedule your consultation today.
 212-535-3088
212-535-3088 



