Melasma Pregnancy Mask
During pregnancy, the body undergoes many changes as the baby develops and hormone levels fluctuate. One common skin condition that affects as many as 50 to 70% of all pregnant women is melasma. This condition is characterized by skin discoloration and hyperpigmentation in the form of brown patches most commonly found on the forehead, cheeks, chin, and upper lip. While the exact cause of melasma is still unknown, the condition is often triggered by rising estrogen and progesterone levels, unprotected sun exposure, and genetic predisposition. When melasma appears during pregnancy, the condition is sometimes also referred to as “chloasma” or “the mask of pregnancy.” While melasma is common during pregnancy, many people wonder how to prevent the onset of skin pigmentation on the face or whether lightening the dark patches of skin is possible during pregnancy. The best first step in dealing with melasma during pregnancy is to consult your OB-GYN, who can refer you to an expert board-certified dermatologist, such as Dr. Michele Green.
Determining the best melasma treatment during pregnancy can be complicated since not all topical medications, skincare products, chemical peels, light therapies, and laser treatments are safe for use during pregnancy. Topical retinoids containing tretinoin or skin-lightening creams containing hydroquinone may be harmful to the fetus when applied while pregnant or breastfeeding. As such, it is essential to choose gentle treatment options that can lighten the skin, such as azelaic acid creams, and to focus on melasma prevention. As one of the major risk factors for developing melasma during pregnancy is exposure to harmful UVA and UVB rays, patients need to practice strict sun protection by either staying inside when the sun is at its peak intensity, wearing sunscreen of SPF 30 or higher whenever they go outside, or wearing protective clothing, such as a wide-brimmed hat. To figure out the best treatment option for you, schedule your initial consultation with Dr. Michele Green.
Experienced board-certified dermatologist Dr. Michele Green has been expertly treating patients at her Upper East Side New York City dermatology office for more than 25 years. A master at treating a wide range of medical conditions and cosmetic concerns, Dr. Green creates individualized treatment plans for each patient, ensuring that all treatment options will be safe and effective while meeting their specific needs. Dr. Green is also highly experienced in treating patients of all skin tones throughout all stages of pregnancy. Well-known for high patient satisfaction, Dr. Green has been voted one of the best dermatologists by such publications as New York Magazine, Castle Connolly, and Super Doctors.
What is Melasma during pregnancy?
Melasma is a skin condition characterized by the appearance of symmetrical hyperpigmentation on the skin’s surface. The skin pigmentation may be gray, brown, or tan and may appear as small freckle-like spots or larger brown patches. Melasma is particularly common for people who are pregnant, with between 50 and 70% of all pregnant people experiencing melasma at some point. In general, melasma is more common in people assigned female at birth than in people who are assigned male at birth, as only 10% of all patients with melasma are male, according to the American Academy of Dermatology. Additionally, patients with darker skin tones are more likely to develop melasma in general and during pregnancy than patients with lighter skin tones, as patients with darker skin already have more active melanin production. Melasma is difficult to treat and can worsen when treated with the wrong method, which is why it is essential to seek out a board-certified dermatologist if you are experiencing melasma symptoms.
What is the difference between Chloasma, Melasma, and the Mask of Pregnancy?
Melasma is a skin condition caused by the overproduction of melanin, which leads to the formation of areas of skin discoloration, most often on the face. Melasma is very common among pregnant patients, affecting as many as 70% of all pregnant people. As such, melasma is sometimes nicknamed the “mask of pregnancy.” Alternatively, melasma may be called “chloasma” when it affects someone pregnant. When talking about skin pigmentation that arises due to hormonal changes and overproduction of melanin, the terms “melasma,” “chloasma,” and “mask of pregnancy” are interchangeable.
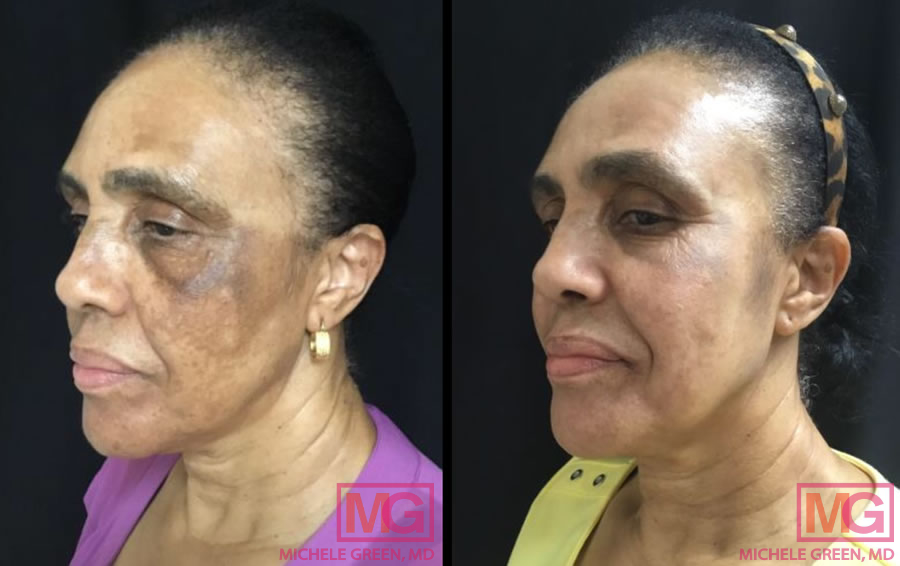
What are the causes of Melasma?
Melasma arises when the overproduction of melanin, which is the naturally occurring pigment in the body that determines skin tone, occurs in the melanocytes. Melasma occurs more commonly in patients with darker skin tones due to the fact that these patients already have active melanin-producing melanocytes. While researchers believe that the occurrence of melasma may be genetic, the exact underlying cause of melasma has not yet been discovered. Yet several risk factors are known to trigger melasma in some patients, including hormonal changes — particularly the rise of estrogen and progesterone that can happen during pregnancy and while taking contraceptives like birth control pills — sun exposure, the use of certain skincare products, thyroid disease, and family history of the condition. Suppose you begin to notice symptoms of melasma. In that case, the best first step is to schedule an appointment with a board-certified dermatologist, such as Dr. Green, who will perform the Wood’s Lamp examination to determine if the hyperpigmentation on your skin is, in fact, melasma.
What causes Melasma during pregnancy?
One of the major risk factors for developing melasma is changing hormone levels during pregnancy. As estrogen and progesterone levels rise throughout the pregnancy, the risk of developing chloasma increases. Additionally, patients who are pregnant may notice skin pigmentation on other areas of the body, including the nipples, armpits, and genitals, as well as the linea nigra, which is a dark line that stretches from the genital area to the stomach. Symptoms of melasma may be worsened due to unprotected sun exposure, irritating skincare products, or already existing hormonal imbalances.
When does Melasma appear in pregnancy?
Many patients wonder, “When does Melasma start in pregnancy?” and the answer is that melasma can appear at any time during one’s pregnancy but is most common during the second or third trimester. Since melasma can be triggered or worsened by the sun’s harmful UVA and UVB rays, patients who are pregnant during the summer months are also more likely to experience melasma, especially in areas of the body that are exposed to the sun without sun protection.
Where does Melasma appear?
Melasma is characterized by brown patches or spots on the skin’s surface that are often symmetrical. The condition appears most commonly on the face, including the forehead, cheeks, chin, upper lip, and around the mouth, but it can also appear on the back and neck. The more these areas of the body are exposed to the sun, the more prominent the discoloration on the skin is likely to be. While melasma causes areas of skin discoloration, the brown patches do not itch or feel uncomfortable. If you notice new or changing dark spots on the skin’s surface, it is best to consult a dermatologist to determine if these areas of hyperpigmentation are harmless or a symptom of skin cancer.

Is Melasma treatment for pregnancy mask possible?
Melasma treatment during pregnancy is more difficult, as many treatment options for melasma are not safe for patients who are pregnant or breastfeeding. That is why it is essential to consult with your OB-GYN and a board-certified dermatologist, such as Dr. Green, before attempting any treatments for melasma on your own. Dr. Green is well-versed in all of the treatment options for melasma that are safe and effective for pregnant patients. However, since many treatment options cannot be used during pregnancy, the best way to minimize the effects of melasma is to engage in prevention practices, consistently applying sunscreen and avoiding unnecessary sun exposure to avoid worsening the melasma. After pregnancy and breastfeeding have finished, some patients may find that their pregnancy mask has disappeared. For others, office treatments such as Cosmelan can be used to treat the pregnancy mask.
The Cosmelan mask is a medical-grade mask used to treat various types of hyperpigmentation, including melasma, sunspots, acne scarring, and post-inflammatory hyperpigmentation. Cosmelan treatment cannot make melasma worse and is the best depigmentation treatment for melasma, as laser treatments can make melasma worse. The mask is applied in the office by Dr. Green and left for a number of hours, depending on your skin type, skin tone, and severity of melasma. Once removed at home with a gentle facial cleanser, patients may experience a slight “peeling” of the skin that will decrease facial hyperpigmentation and leave the skin feeling smooth. For weeks later, a second application of the mask may be necessary depending on the skin’s response to the mask. During Cosmelan treatment, it is essential to use a series of gentle creams and sunscreen to maintain the effects of the procedure and keep the skin clear. Patients must avoid sun exposure, and Dr. Green recommends layering a chemical-based and physical-based sunscreen for maximum protection to avoid the recurrence of melasma.
How to treat melasma during pregnancy
To treat melasma, Dr. Green would typically turn to such treatments as Mesopeels, chemical peels, microdermabrasion, the Cosmelan Peel, or the VBeam laser. However, these treatment options are not available during pregnancy. Instead, Dr. Green may recommend that patients apply a vitamin C solution, which can be used to lighten the skin and boost collagen production. Alternatively, Dr. Green sometimes prescribes azelaic acid cream, which is another skin-lightening solution to treat hyperpigmentation. While azelaic acid is safe for use during pregnancy, it will only be prescribed if it is essential.
What helps Melasma during pregnancy?
One of the best ways to help keep symptoms of melasma at bay during pregnancy is to practice strict sun protection by wearing sunscreen of SPF 30 or higher and protective clothing. In terms of treatment options for melasma during pregnancy, there are not many that are deemed safe for use during pregnancy. While pregnant, patients should avoid topical retinoids with ingredients like tretinoin, creams with hydroquinone, chemical peels, and laser therapy.
Does Melasma go away after pregnancy?
After pregnancy, most patients find that the symptoms of melasma will fade over time without any medical intervention. However, it can take months for the pigmentation to fully fade after giving birth. Once patients have given birth and stopped breastfeeding, more treatment options are available for reducing the appearance of melasma, including mesopeels, Cosmelan Peels, chemical peels, VBeam Laser Treatment, and microdermabrasion.
How to avoid pigmentation during pregnancy
The best way to avoid pigmentation during pregnancy is to protect yourself from sun exposure. Exposing the skin to the sun’s harmful UVA and UVB rays can trigger the incidence of melasma and worsen any already existing pigmentation, so patients should take great care to maximize sun protection. To do so, Dr. Green recommends wearing sunscreen of SPF 30 or higher whenever you go outside and reapply every two hours. It is best to turn to a physical sunscreen — rather than a chemical sunscreen — containing ingredients such as zinc oxide or titanium dioxide. If you can, avoid being outside between the hours of 10 am and 2 pm when the sun is at its most intense. Additionally, patients can wear protective clothing, such as loose, long-sleeved shirts, long pants, and a wide-brimmed hat.
How to prevent melasma during pregnancy
Patients often wonder, “How to prevent pregnancy mask,” and the answer is to practice strict sun avoidance, use gentle skincare products, and engage in a healthy lifestyle. In addition to always applying sunscreen before going outside, patients should choose gentle skincare products that will not irritate the skin. Harsh products can also worsen the appearance of melasma. Instead, patients should look for skincare products that are fragrance-free and non-comedogenic, such as cleansers, moisturizers, foundations, and concealers. Additionally, patients can help prevent the appearance of melasma by eating a healthy diet, resting well, having a regular exercise routine, and taking supplements containing such ingredients as omega-3 fatty acids.
When does pregnancy Melasma start?
Melasma can occur at any time during pregnancy but appears most commonly during the second and third trimesters. Additionally, because melasma is often triggered by direct sunlight, pregnancy melasma is often worse during the summer months when exposure to the sun’s UVA and UVB rays is more frequent. Patients can help prevent the appearance and worsening of melasma by always wearing sunscreen when going outside, staying in the shade, and wearing clothing that covers the skin.
Is Melasma a sign of pregnancy?
Melasma is a common skin condition among pregnant people, affecting as many as 70% of all people who are pregnant. Hormonal changes during pregnancy, such as the rising levels of progesterone and estrogen, can trigger the symptoms of melasma. While melasma is often called “the mask of pregnancy,” it is not necessarily a sign of pregnancy. Patients who are not pregnant can still develop melasma, as it can also be triggered by unprotected sun exposure, thyroid problems, hormonal changes associated with contraceptives, and a family history of the skin condition. Suppose you have started to develop symptoms of melasma. In that case, the best first step is to schedule an appointment with Dr. Green, who will test the affected area to determine if the hyperpigmentation is, in fact, melasma.
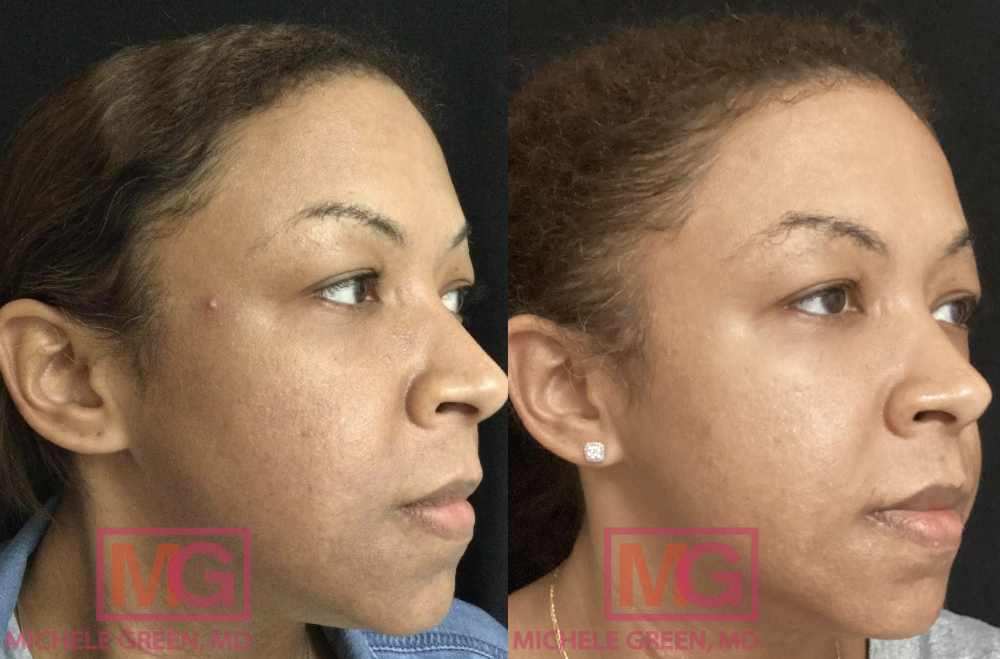
How to get started with Melasma treatment during pregnancy today
Melasma is a common skin condition characterized by gray or brown dark spots that often appear on the face, specifically the nose, cheeks, chin, forehead, and jawline. The skin condition is particularly common during pregnancy, with as many as 70% of all pregnant people experiencing symptoms of melasma. While melasma is benign, the dark spots are tricky to remove, particularly during pregnancy, and can cause many patients psychological distress. Many melasma patients report feeling uncomfortable with their appearance and even depressed following the onset of melasma symptoms. Luckily, board-certified dermatologist Dr. Michele Green is an expert at treating all forms of hyperpigmentation, including melasma, on all skin types and knows which treatment options are safe and effective for use during pregnancy.
Dr. Michele Green is an internationally renowned board-certified dermatologist with over two and a half decades of experience providing her patients with the best non-invasive treatment options. Dr. Green takes a holistic approach and embraces a less-is-more philosophy, creating customized skincare routines and treatment plans that cater to the unique concerns and aesthetic goals of her patients. She is consistently identified as one of New York’s best dermatologists by Castle Connolly, New York Magazine, and Super Doctors for her dedication to her patients and expertise. Please call us at 212-535-3088 or email our New York City-based office today to schedule a consultation with Dr. Michele Green and find out how to address your pregnancy melasma today.
 212-535-3088
212-535-3088 



