Hemangioma
A cherry hemangioma is a vascular lesion made of proliferating small blood vessels that clump together. Infantile hemangiomas are benign tumors that usually don’t require medical treatment unless they bleed, become infected, or form an ulcer. Hemangiomas can occur in any area of the body, may vary in size, are bright red to purple, and present as flat or raised. Treatment options for these birthmarks can include beta-blockers like propranolol, corticosteroids, and laser treatments. It is always advised to consult a board-certified healthcare provider with a pediatric background, such as Dr. Michele Green in NYC, regarding treatment options.
Infantile hemangiomas usually appear at birth or within the first few weeks of life, often going through a rapid growth phase in the first five months of life. After, hemangiomas go through a process called involution, where the lesions shrink in size and fade in color. Most infantile hemangiomas resolve on their own by the time a child is ten years of age. Caucasian females who are born prematurely or at a low birth weight are the most likely to be affected by infantile hemangiomas. If you are concerned about your child’s hemangioma or the residual skin changes that it has caused, schedule a consultation with Dr. Green at her private dermatology office in NYC.
Dr. Michele Green is an internationally renowned board-certified dermatologist with over two and a half decades of experience providing some of the world’s most discerning individuals with the best non-invasive cosmetic treatments, including cherry hemangioma removal. Dr. Green takes a holistic approach and embraces a less-is-more philosophy regarding skin rejuvenation, customizing each patient’s treatment plan to suit their particular skin concerns and aesthetic goals best. She is consistently identified as one of NYC’s best dermatologists by Castle Connolly, New York Magazine, and Super Doctors for her dedication to her patients and expertise.
What is a hemangioma?
Hemangiomas are common benign skin lesions made of proliferating blood vessels. These growths can appear anywhere on your body, especially on the face, chest, and back, as red or purple lumps. Hemangiomas are usually harmless and tend to resolve on their own eventually, usually by the time a child is ten years of age. Superficial hemangiomas are the most common type of hemangioma. Superficial hemangiomas are clumps of small blood vessels that are packed tightly together. Their proximity to the surface of the skin usually causes them to be bright red.
Cavernous hemangiomas are made of larger blood vessels with spaces or “caverns” between them. Cavernous hemangiomas are usually described as deep and may have a blue or purple tint. Although hemangiomas are most common in infants and children, adults can develop them too. While cherry hemangiomas usually don’t require treatment for medical purposes. However, several non-invasive treatment options can be used to remove or reduce the appearance of hemangiomas or the residual skin changes they may cause. Hemangiomas may require medical treatment in particular cases, such as when they affect the mouth or diaper area. Hemangiomas in these areas are prone to bleeding, infection, and ulceration. Dr. Green in NYC is an internationally renowned board-certified dermatologist with a pediatric background and will work with you to select the treatment options best suited to resolving your child’s hemangioma.
What do hemangiomas look like?
Hemangiomas can occur anywhere on the body and are usually bright red to purple. These benign lesions may be smooth and flat against the surface of the skin or raised, even protruding as a nodule. Infantile hemangiomas usually go through a rapid growth phase in the first few months of life before eventually involuting, resulting in their shrinking in size and fading in color. While most infantile hemangiomas will have disappeared by the time a child has reached ten years of age, they can occasionally result in residual skin changes, including a wrinkly texture or red appearance. There are a variety of non-invasive treatment options available for reducing the appearance of hemangioma and any residual skin changes at Dr. Green’s private, boutique dermatology office in Manhattan’s Upper East Side neighborhood.
Cherry angioma vs Cherry hemangioma: What’s the difference between these vascular lesions?
Cherry angiomas and cherry hemangiomas are common, benign skin growths that are very similar in appearance but are made of different cells. While cherry angiomas are made of lymphatic or blood vessels, cherry hemangiomas are made of only blood vessels. Cherry hemangiomas may appear in infancy or childhood, whereas cherry angiomas usually affect adults. The term ‘cherry’ simply refers to the color of these skin growths, which can appear as bright cherry-red to purple. Both types of skin lesions are usually between two and four millimeters and may be smooth and flat or raised and dome-shaped. Cherry angiomas and cherry hemangiomas do not go away on their own. While cherry angiomas and hemangiomas normally don’t require removal for medical purposes, many individuals choose to have them treated for cosmetic reasons. Dr. Michele Green offers a number of treatment options for removing cherry angiomas and hemangiomas without discomfort, downtime, or residual scarring. When you consult with Dr. Green, she will work with you to create a personalized treatment plan for achieving and maintaining a clear, even-toned complexion that lasts.
Is a hemangioma dangerous?
Though this form of vascular tumor is typically harmless, painless, and low-risk, hemangiomas can be unsightly and, on occasion, can get in the way of an infant’s respiratory, auditory, digestive, or ocular system. Usually, hemangiomas are not dangerous unless they obstruct vision or airways or turn into wounds. A child’s hemangioma near the mouth or diaper area may be prone to bleeding, infection, or ulceration due to friction. In these cases, it is recommended to have medical treatment with a board-certified healthcare provider with a pediatric background. Dr. Green’s dermatology office is here to help with any concerns related to the diagnosis and treatment of hemangiomas.
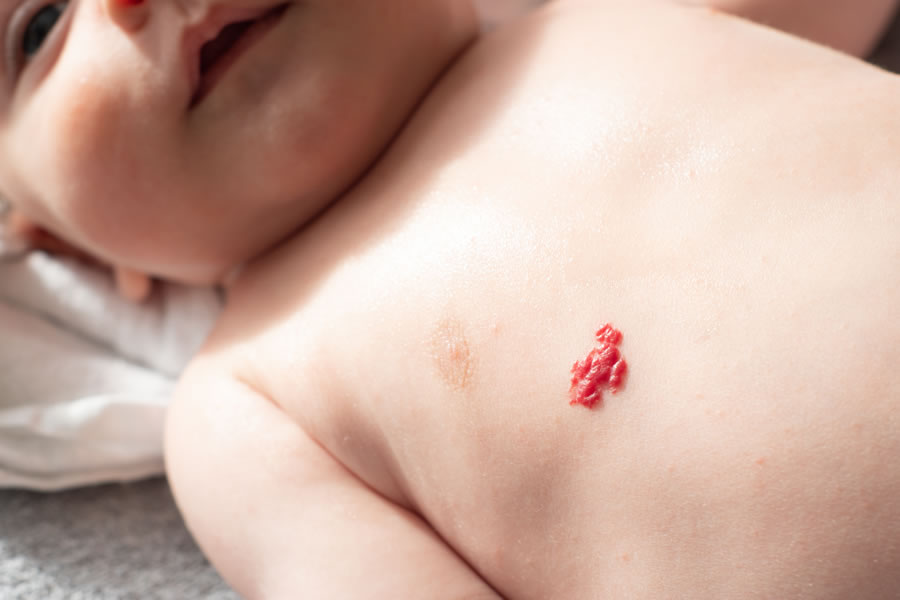
Types of Hemangioma
Infantile Hemangiomas
An infantile hemangioma is a common vascular birthmark that is made of extra blood vessels in the skin. Infantile hemangiomas usually aren’t associated with any medical complications and go away on their own. Infantile hemangiomas are often present at birth or develop within the first few weeks of life; if one is visible at the time a child is born, it is also referred to as a congenital hemangioma. Infantile hemangiomas are typically painless and low-risk, but sometimes, a hemangioma can bleed or form an ulcer, causing pain and discomfort. Infantile hemangioma is also occasionally linked with spine or nervous system abnormalities and, if located on certain sensitive areas (such as the face or neck), can be disfiguring. If your child has a large hemangioma on the face, scalp, or neck, they are at risk for PHACE Syndrome, which links a series of vascular, endocrine, and neural abnormalities and malformations. Your healthcare provider should monitor a large facial hemangioma.
Infantile hemangiomas are categorized as one of the three classifications below:
Strawberry mark (Capillary Hemangioma):
This is the most common type of hemangioma, featuring the classic bright red, rubbery bump or patch. This type of hemangioma can have a textured surface and varies between a specific, acute bump and a milder, broader patch of the skin. Strawberry marks are a type of superficial hemangioma, meaning they form close to the surface of the skin.
Deep hemangioma (Cavernous Hemangioma):
This type of hemangioma varies from the typical red bump, tending to be darker in coloration, usually with a blue or purple tint. If your child’s hemangioma begins to swell, particularly between 2-4 months of age, it may be classified as a deep hemangioma.
Combination / Mixed hemangioma:
In the case of a combination hemangioma, the vascular anomaly is deep within the dermis, and a superficial stain will appear on the surface of the skin. This combination classification is defined based on the amount of soft tissue involved in the hemangioma.
If you think your child may have an infantile hemangioma, it’s best to monitor it with your healthcare provider. Dr. Green is available to examine any infantile hemangiomas and discuss treatment options for unsightly or disfiguring hemangiomas.
Proliferative Hemangiomas
About 80% of children with a hemangioma present with just one vascular malformation, but proliferative hemangiomas (or multiple hemangiomas) remain common. Proliferative hemangiomas develop from a proliferation of the cells that line the blood vessels, known as endothelial cells.
In general, if a patient has six or more hemangiomas, they may be at risk for internal organ issues, particularly with the liver. Infants tend to have a small number of lesions. Still, according to the Boston Children’s Hospital Vascular Anomalies Center, some infants can develop several hundred lesions with this type of hemangioma classification.
Lobular Capillary Hemangiomas
This type of hemangioma presents as small red bumps on the hands, face, and arms. Each lesion has a concentrated amount of blood vessels, which can make the area sensitive to bleeding, even with mild contact. A lobular capillary hemangioma can sometimes be referred to as a “pregnancy tumor” due to its common development in the nose and mouth during pregnancy. They typically are low-risk but can be delicate and should be monitored by your health care provider.
Internal Hemangiomas
In extremely rare cases, internal hemangiomas can develop on the internal organs. If a child presents with six or more infantile hemangiomas, it is common practice to examine the liver and spleen to detect any internal hemangiomas.
An internal hemangioma typically won’t present with symptoms unless it grows large or in a sensitive area. In this case, a patient may develop symptoms such as nausea/vomiting, loss of appetite, and pain/bloating in the abdomen. Internal hemangioma can be confirmed through a computed tomography (CT) scan, Magnetic Resonance Imaging (MRI), or ultrasound. The most common types of internal hemangiomas are in the liver and the intestines.
What is a hepatic hemangioma? When should a liver hemangioma be removed?
Liver hemangiomas, also known as hepatic hemangiomas, occur when the endothelial cells surrounding the liver multiply. Liver hemangiomas can be infantile hemangiomas but sometimes occur unrelated to a hemangioma from infancy. They are thought to grow more rapidly with an increase in estrogen, which can occur through hormone therapy during menopause, during pregnancy, or through the use of oral contraceptives. Liver hemangiomas may require surgical removal if there is a rupture, intratumoral bleeding, progressive abdominal pain in combination with a size of greater than five centimeters, or organ or vessel compression.
Is a spleen hemangioma dangerous? Is a brain hemangioma dangerous?
Splenic hemangiomas are very rare, benign tumors that are not treated unless they are very large or symptomatic. Splenic hemangiomas are usually found incidentally, as the majority are asymptomatic. Brain hemangiomas, or hemangioblastomas, are also noncancerous tumors that are very uncommon. Hemangioblastomas are slow-growing and unlikely to grow back following removal. While hemangioblastomas are noncancerous, it is usually recommended that they are removed to prevent them from pressing against other surrounding tissue.
How is a hemangioma diagnosed?
Typically, a hemangioma on the skin can be diagnosed when a lesion first develops. A Doppler machine will sometimes be used to note any changes in blood flow surrounding the affected area in order to confirm the hemangioma. In some cases, an ultrasound can be used as a tool to understand the depth of the hemangioma. Occasionally, an MRI or CT scan will be used for an imaging test, such as in the case of a potential hemangioma of the liver or another internal organ.
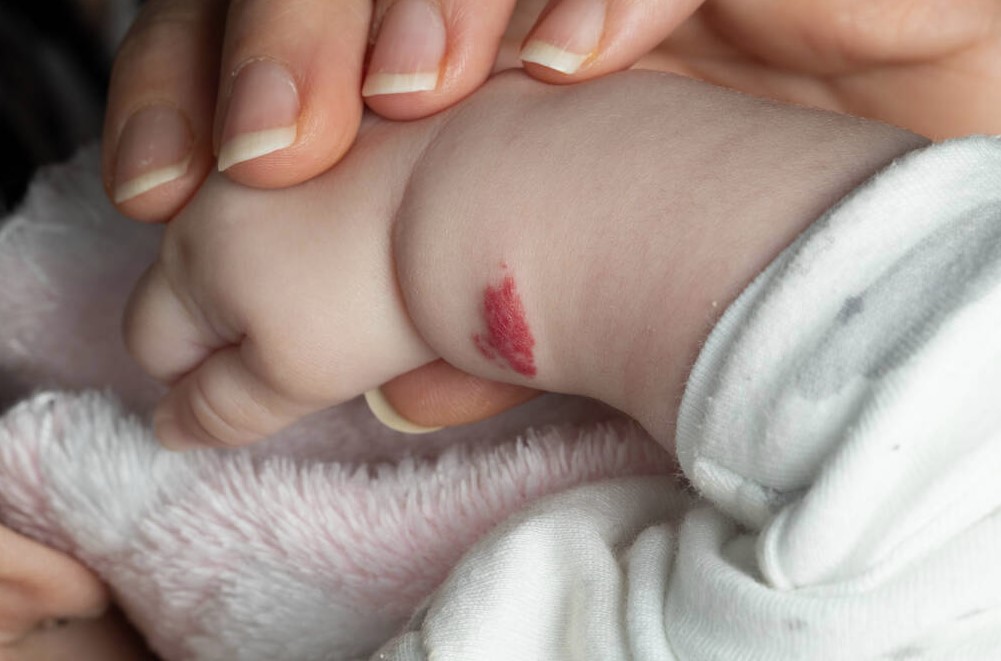
Can a hemangioma be removed?
In the case of an unsightly, disfiguring, or potentially hazardous hemangioma, the lesion can be removed through a variety of treatment options, discussed in the following section.
Hemangioma Treatment Options
Treatment for a hemangioma will depend on a variety of factors, including the size, location, and rate of growth or involution of the hemangioma, as well as any ulceration of the lesion(s) and the age of the patient. Often, hemangiomas will go away without treatment, but when a hemangioma is located on the face, eyes, or along the spine, removal or reduction treatment options may be recommended.
The following treatment options are available to treat a variety of hemangiomas:
- Laser therapy can be used to treat ulcerated hemangiomas, as well as abnormal skin on the affected area of the hemangioma. The Vbeam laser treatment is the gold standard for removing vascular lesions, especially hemangioma. Dr. Green is an expert in the Vbeam laser and has been using it for over a decade in her private NYC dermatology office.
- Surgical removal is typically used with smaller hemangiomas that can be completely removed through minimally invasive surgery.
- Topical beta-blockers, such as timolol, can be applied to small, superficial hemangiomas, as well as to ulcerative (open and bleeding) hemangiomas.
- Oral beta-blockers, such as oral propranolol, which is a non-invasive hemangioma therapy.
- Corticosteroids are sometimes used in the event beta-blockers are ineffective. Side effects can occur in young children with this treatment, such as irritability or trouble sleeping.
- Embolization, in which the blood flow to the hemangioma is cut off, eventually eliminating the development of the vascular anomaly
Are hemangiomas genetic?
The exact cause of hemangioma formation is unknown. Usually, hemangiomas develop by chance, although in some cases, they may be inherited in a family through autosomal dominant traits. Infantile hemangiomas are most common among premature babies at a low birth weight or in twins/ triplets. These kinds of hemangiomas typically appear at birth or within the first few weeks of life. Most infantile hemangiomas go through a rapid growth phase within the first few months of life, which ceases around five months old. Infantile hemangiomas then remain unchanged for several months before going through a process called involution. Involution is where the hemangioma shrinks in size and disappears, which is usually complete by the time a child is ten years of age. Although hemangiomas are most common in infants and children, adults can develop them too. In fact, about 75% of people aged 75 and older have cherry hemangiomas. While cherry hemangiomas usually don’t require treatment for medical purposes, many choose to have them removed for cosmetic reasons.
Do hemangiomas grow?
Many hemangiomas go through phases of growth. Infantile hemangiomas usually grow quickly within the first few months of life. However, around 80% of hemangiomas stop growing at five months old. Once hemangiomas stop growing, they remain unchanged for several months before involuting. Involution is the process by which hemangiomas shrink in size and eventually disappear. Most hemangiomas will be completely gone by the time a child is ten years of age. Sometimes, an involuted hemangioma can leave behind areas of skin that are wrinkly and soft or red. If hemangioma involution has caused skin changes, there are non-invasive cosmetic treatment options available at Dr. Green’s private dermatology office in NYC for reducing their appearance without discomfort or downtime.
When do hemangiomas stop growing?
Infantile hemangiomas appear at birth or within the first few weeks of life and usually go through several phases. The early rapid growth phase of infantile hemangiomas usually occurs during the first few months of life. At around five months, during phase two, the growth slows down. In phase three, the hemangioma does not change for several months. In phase four, hemangiomas begin involuting, meaning they start to shrink in size and fade in color. Many infantile hemangiomas will go away completely by the time a child is five years of age, with most being gone by the time a child is ten years of age. If a hemangioma produces residual skin changes after involution, such as a wrinkly texture or red appearance, Dr. Green can resolve them with a variety of non-invasive treatment options available at her private dermatology office in NYC.
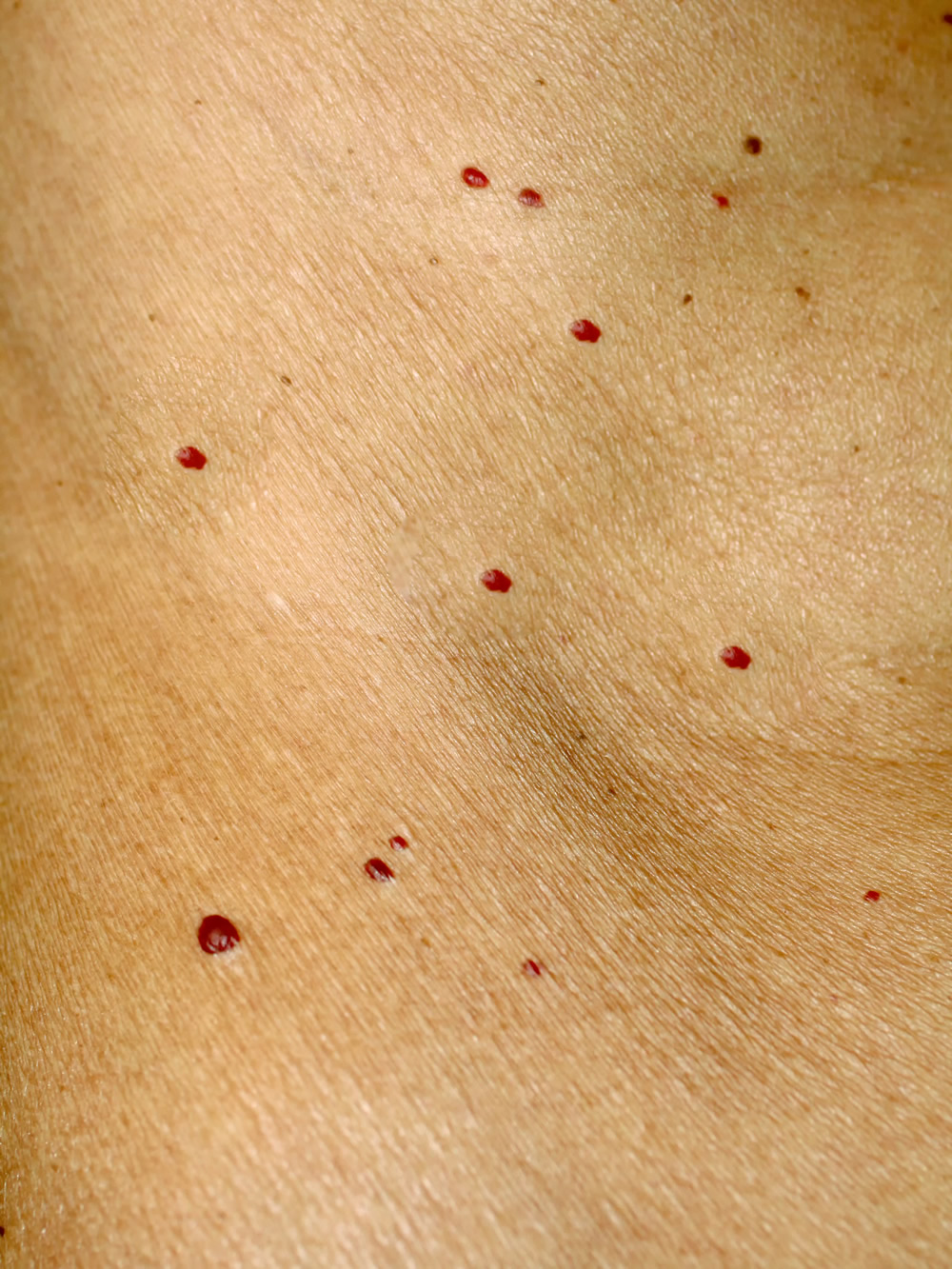
What is hemangioma in adults? How to treat hemangioma in adults
Although hemangiomas are most common in infants and children, adults can develop them too. In fact, about 75% of people aged 75 and older have cherry hemangiomas. While cherry hemangiomas usually don’t require treatment for medical purposes, many choose to have them removed for cosmetic reasons. Treatment options for hemangiomas in adults are similar to treating a child’s hemangioma. Topical beta-blockers may help lighten the hemangioma and slow its growth. This works best on small, superficial hemangiomas. Topical antibiotics are prescribed for hemangiomas that have become ulcers and open sores that may become infected.
Oral medications like propranolol and prednisone may be prescribed, which reduce the amount of blood flow to the hemangiomas, reducing their size. Surgical removal may be recommended if other treatment options have failed. If the hemangioma has resolved aside from redness, Dr. Green recommends the V-Beam laser treatment. The V-Beam operates on a wavelength that targets exclusively red pigment, leaving surrounding skin cells untouched. Dr. Green also uses the V-Beam to treat rosacea, acne, post-inflammatory hyperpigmentation, stretch marks, post-surgical scars, and broken capillaries, among other skin conditions. When you consult with Dr. Green at her private, boutique dermatology office in NYC, she will work with you to determine which treatment options are best suited to your needs and goals.
When does hemangioma go away?
Hemangiomas usually go away by the time a child reaches ten years of age. About 80 percent of hemangiomas stop growing by about five months. Once the initial growth phase is complete, the hemangioma remains unchanged for some time. Once involution begins, the hemangiomas shrink in size and fade in color. Many hemangiomas will be resolved by the time a child is five years of age. Sometimes, infantile hemangiomas that have gone through involution can cause residual skin changes, including a wrinkly skin texture or a red appearance. Dr. Green can treat hemangiomas and resolve any residual skin changes to reveal a clear, even-toned complexion that lasts.
What is a hemangioma on the spine? Are hemangiomas on the spine dangerous?
Spinal hemangiomas are the most common tumors of the spine, usually found incidentally with imaging tests. These vascular lesions form due to the proliferation of blood vessels. Usually, spinal hemangiomas are benign and asymptomatic. Healthcare providers typically do not recommend removing spinal hemangiomas unless you have symptoms, such as pain or affected movement.
Is hemangioma a tumor?
Yes, a hemangioma is a type of tumor. However, not all tumors are cancerous. A tumor is a medical term referring to the growth of tissue that forms when abnormal cells clump together. Noncancerous tumors commonly affect the skin, bones, organs, glands, and tissues. They don’t spread to other parts of your body and aren’t life-threatening. Hemangiomas are a type of common, noncancerous tumor made of proliferating blood vessels that can often be removed without downtime or discomfort.
Can hemangioma be cancerous?
Cherry hemangiomas are usually benign, harmless, and of little concern. These cutaneous vascular proliferations typically do not require any treatment; however, if you develop new lesions or red spots or notice a change in the appearance of a red mole, you should consult a dermatologist to determine if the growth is, in fact, a cherry angioma or another type of lesion or skin cancer. An expert dermatologist such as Dr. Michele Green will be able to confirm if the new growth or clinical changes in appearance warrant further evaluation and treatment. If necessary, a biopsy of the lesion may be performed and sent to a laboratory for histological review to rule out skin cancer or other dermatological conditions.
What is cavernous hemangioma?
A cavernous hemangioma is made of larger dilated blood vessels. These hemangiomas can occur throughout the body, may vary in size, and are usually described as ‘deep.’ Compared to capillary hemangiomas, the blood vessels that make up cavernous hemangiomas are not packed as closely. The spaces, or ‘caverns,’ in between the vessels are filled with blood. Cavernous hemangiomas are less common than capillary hemangiomas. Capillary hemangiomas are the most common type of hemangioma, consisting of numerous blood vessels that are normal in diameter and size and tightly packed. Capillary hemangiomas are also referred to as superficial hemangiomas, and their proximity to the skin’s surface often causes them to be bright red. Superficial hemangiomas, like cavernous hemangiomas, can occur anywhere on the body and may vary in size. Superficial hemangiomas may be flat and smooth or raised, sometimes even protruding as a nodule.
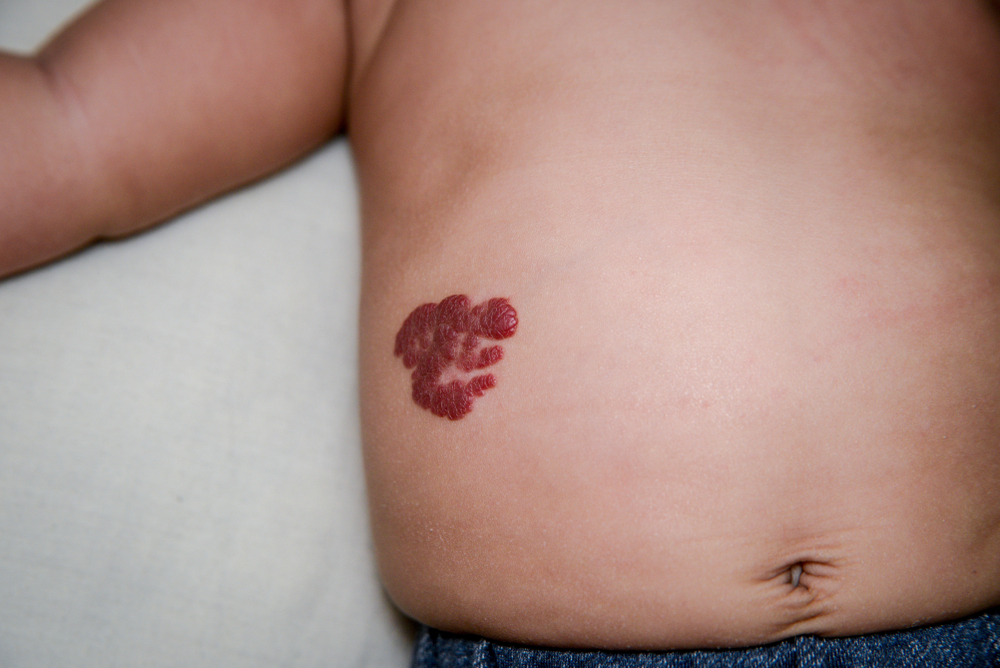
Will hemangioma go away? How to get rid of hemangioma
Infantile hemangiomas usually go away by age 10, with many going away by age 5. Infantile hemangiomas are benign, vascular birthmarks that are made of proliferating blood vessels. Caucasian females who are born prematurely at a low birth weight are the most likely to be affected by infantile hemangiomas. Hemangiomas usually go away on their own by involuting, resulting in their shrinking in size and fading in color.
How to get started with Hemangioma treatment today
A hemangioma is a vascular birthmark that’s made of proliferating blood vessels that usually don’t require medical treatment and eventually resolve on their own. Most hemangiomas will involute, shrinking in size and fading in color, by the time a child is ten years of age. Sometimes, hemangiomas can result in residual skin changes, such as a wrinkly skin texture or a red appearance. Consulting a board-certified healthcare provider with a pediatric background, such as Dr. Green in NYC, is the best way to remove a hemangioma and resolve any residual effects. Dr. Green offers a variety of non-invasive treatment options at her private, boutique dermatology office in Manhattan’s Upper East Side neighborhood.
Dr. Michele Green is an internationally renowned board-certified dermatologist with over two and a half decades of experience providing some of the world’s most discerning individuals with the best non-invasive cosmetic treatments, including cherry hemangioma removal. Dr. Green takes a holistic approach and embraces a less-is-more philosophy regarding skin rejuvenation, customizing each patient’s treatment plan to suit their particular skin concerns and aesthetic goals best. She is consistently identified as one of NYC’s best dermatologists by Castle Connolly, New York Magazine, and Super Doctors for her dedication to her patients and expertise. If either you or a family member has a hemangioma, contact Dr. Green in her NYC office to learn about the best treatment options. You can also contact us online for further information and to help with your personalized treatment plan, or call 212-535-3088 today.
 212-535-3088
212-535-3088 



