Rosacea Treatment
Many individuals seek rosacea treatment to reduce persistent facial redness, flushing, and visible blood vessels that can be difficult to conceal and become increasingly noticeable over time. A rosacea patient may notice that symptoms fluctuate, making it hard to predict when redness will worsen. Rosacea often affects the central areas of the face and can vary in severity, making skin tone appear uneven and contributing to ongoing sensitivity or discomfort. For some, flare-ups are triggered by environmental or lifestyle factors, while others experience more constant redness that does not fully fade. Rosacea treatments are pursued to improve appearance by reducing the intensity and frequency of visible symptoms, and for many people, this can also support overall quality of life. With appropriate care, many patients notice that their complexion appears more balanced. An experienced board-certified dermatologist, such as Dr. Green in NYC, can evaluate how rosacea presents on your skin and recommend treatment options tailored to your specific concerns.
Rosacea treatment works by addressing the underlying skin factors that contribute to redness, flushing, and visible blood vessels, using a combination of targeted therapies tailored to individual needs. Laser and light-based treatments reduce vascular activity beneath the skin’s surface, while medical-grade facials and topical therapies support the skin barrier and improve tolerance to daily environmental exposure. Because rosacea can present differently from person to person, treatment plans are often customized to reflect symptom patterns, skin sensitivity, and treatment goals. Results typically develop gradually as the skin responds to treatment. A board-certified dermatologist, such as Dr. Michele Green, will determine which rosacea treatment options are most appropriate based on a thorough evaluation of your skin.
Dr. Michele Green is an internationally recognized, board-certified dermatologist with over 25 years of experience delivering advanced, non-invasive treatments for chronic skin conditions, including rosacea. She approaches rosacea treatment with careful attention to skin sensitivity, selecting options suited to the condition’s long-term nature. Recognized frequently as one of New York City’s leading dermatologists by Castle Connolly, New York Magazine, and Super Doctors, she is known for her expertise and dedication to patient care. When you consult with Dr. Green at her private dermatology practice on Manhattan’s Upper East Side, she will work with you to develop a personalized rosacea treatment plan designed to improve skin comfort, appearance, and confidence.
What is rosacea?
Rosacea is a chronic inflammatory skin condition that affects the skin’s blood vessels and immune response, leading to long-term changes in how the skin reacts to internal and external stimuli. It is characterized by an abnormal tendency for facial blood vessels to dilate and remain enlarged, which contributes to ongoing inflammation and heightened skin sensitivity. Unlike temporary flushing, rosacea involves persistent changes in vascular behavior and inflammatory signaling that make the skin more reactive over time. These changes can disrupt the skin barrier and increase sensitivity to heat, sunlight, skincare products, and stress. Rosacea is not contagious and is not caused by poor hygiene; rather, it reflects an underlying imbalance in how the skin regulates inflammation and vascular activity. Although the exact cause is still being studied, rosacea is a long-term condition that tends to progress gradually without management. While it cannot be cured, rosacea can be effectively controlled through appropriate treatment strategies that address inflammation, vascular activity, and skin sensitivity.

Before & After photo: Male VBeam for Rosacea
How common is rosacea?
According to the American Academy of Dermatology, approximately 14 million adults, or 1 in 10 people in the United States, are affected by rosacea. Most people with rosacea are fair-skinned and between the ages of 30 and 50. Many individuals with rosacea also have a family member with a skin condition. Women are more likely than men to develop rosacea, although men tend to experience more severe symptoms.
What causes rosacea?
Rosacea is a complex skin condition whose exact etiology remains unknown. Although the precise cause of rosacea is unknown, several contributing factors are known to play a role in its development. For example, the condition is more common in women than in men. Additionally, it tends to run in families, suggesting a genetic component. Below are a few possible explanations for rosacea that are currently being researched:
Genetic predisposition: Patients with a family history of rosacea have been observed to have an increased risk of developing rosacea
Immune System: Rosacea may also be caused by an overactive immune system. A peripheral blood monoclonal proliferation assay showed that Bacillus oleronius stimulated an immune response in 79% of 22 patients with subtype 2 (papulopustular type) rosacea.
Microscopic mites on the human face, specifically Demodex folliculorum, have been linked to increased susceptibility to rosacea.
Helicobacter pylori (H. pylori) is a bacterium that normally lives in the gut. It is believed that this bacterium can trigger rosacea flares by producing an enzyme that causes facial flushing.
What areas of the body are affected by rosacea?
Rosacea most commonly affects the central areas of the face, including the cheeks, nose, chin, and forehead, where redness and flushing are often most noticeable. These regions are especially prone to visible changes due to increased blood vessel activity near the skin’s surface. In some individuals, rosacea may also extend beyond the face to involve the neck, chest, scalp, or upper back, though this is less common. Eye involvement is also common, with many people experiencing ocular symptoms such as irritation, dryness, or redness, a presentation known as ocular rosacea. The specific areas involved can vary from person to person, and some individuals may notice symptoms confined to one region while others experience a broader distribution. Understanding which areas of the body are affected can help guide evaluation and treatment decisions, as rosacea does not always present in the same pattern for everyone.
What are the symptoms of rosacea?
Rosacea can present with a range of symptoms that vary in severity and may change over time, which is why it often looks different from one person to another. One of the most common signs is persistent redness across the central areas of the face, particularly the cheeks, nose, chin, and forehead, which may resemble a constant flush that does not fully fade. Many individuals also notice visible blood vessels beneath the skin, especially around the nose and cheeks, which can become more noticeable as rosacea progresses. In some cases, rosacea causes red, acne-like bumps or pus-filled lesions that may feel tender or inflamed but typically appear without blackheads or whiteheads. The skin may feel unusually sensitive, with sensations such as burning, stinging, dryness, or tightness, especially during flare-ups. Some people experience swelling or thickening of the skin over time, most commonly affecting the nose, where the surface can become uneven or enlarged. Rosacea can also involve the eyes, leading to symptoms such as redness, irritation, dryness, tearing, or a gritty sensation, a condition known as ocular rosacea. Because symptoms can fluctuate and overlap, rosacea often requires careful evaluation to understand how it is affecting the skin at different stages.
What are the common triggers for rosacea symptoms?
For many patients, rosacea can be aggravated or triggered by specific dietary, lifestyle, or environmental factors, such as:
- Stress
- Genetics
- Heat, hot baths, steam rooms, and saunas
- Sunlight or ultraviolet light
- Cold weather or wind exposure
- Caffeine and caffeinated drinks, like coffee
- Dairy products
- Spicy food, spices, and seasonings with such ingredients as cayenne pepper or red pepper
- Foods containing cinnamaldehyde, such as citrus fruits, tomatoes, and chocolate
- Smoking or alcohol
- Intense exercise
- Hormonal or endocrine problems, such as thyroid diseases or menopause
- Hypertension
- Medications that dilate the blood vessels, such as certain blood pressure medications such as blood pressure medications
- Specific skincare or cosmetic products, such as Retin-A cream, or creams that have fragrance or alcohol-based ingredients
It is essential to identify the triggers that can exacerbate rosacea and avoid them to keep it under control and prevent flare-ups.

What does rosacea look like?
Rosacea most often presents as persistent redness in the central face, particularly the cheeks, nose, chin, and forehead. This redness may resemble a constant blush or sunburn that does not fully fade and can become more noticeable over time. Many individuals with rosacea also develop visible blood vessels on the skin’s surface, especially around the nose and cheeks, which can give the skin a flushed or inflamed appearance. In addition to redness, rosacea may cause small red bumps or pus-filled lesions that resemble acne breakouts. Unlike acne vulgaris, these bumps typically appear without blackheads or whiteheads.
In some cases, the skin may feel sensitive, dry, or rough, with burning, stinging, or tightness that worsens during flare-ups. Over time, untreated rosacea can lead to skin thickening, most commonly on the nose, where it may become enlarged, uneven, and bulbous, a condition known as rhinophyma. Rosacea can also involve the eyes, causing symptoms such as redness, irritation, dryness, tearing, or a gritty sensation, a condition referred to as ocular rosacea. The appearance and severity of rosacea vary widely from person to person, and symptoms may come and go in response to triggers such as sun exposure, heat, stress, or certain foods. A board-certified dermatologist can evaluate these visible signs and symptoms to determine whether rosacea is present and recommend appropriate treatment options to help manage its appearance and progression.
What are the types of rosacea?
Because rosacea is a complex condition, it has been categorized into four subtypes based on skin appearance. This classification helps categorize rosacea. However, patients may have symptoms of more than one subtype simultaneously.
Subtype 1 – Erythematotelangiectatic Rosacea
Subtype 1 is characterized by persistent facial redness (erythema). Patients with this type of rosacea often experience facial flushing, especially after exposure to rosacea triggers. Broken blood vessels, called telangiectasias, may be present, and the skin may feel irritated, sensitive, and uncomfortable, similar to a sunburn.
Subtype 2 – Papulopustular Rosacea
Subtype 2 is characterized by facial redness and acne-like papules and pustules. The lesions often contain fluid or pus, resembling acne papules and pustules. Patients with this type of rosacea frequently experience an oilier skin texture and raised skin patches.
Subtype 3 – Phymatous Rosacea
Subtype 3, known as phymatous rosacea, is characterized by skin thickening and swelling, or edema, particularly around the nose. When the nose is affected in this way, it is termed rhinophyma.
Subtype 4 – Ocular Rosacea
Subtype 4 is characterized by eye symptoms, including watery eyes, red eyes, a foreign-body sensation, eye burning, dry eyes, styes, and blurred vision. A board-certified ophthalmologist can effectively manage and treat ocular rosacea. Ocular rosacea is defined by pruritic, dry, irritated, and red eyes. In some cases, the eyes can also be photophobic—almost half of patients with rosacea experience ocular rosacea. Many patients complain of eyelid irritation, also called blepharitis or eyelid swelling, which can lead to severe vision problems if left untreated. Ocular rosacea can be associated with conjunctivitis, which can cause redness and inflammation of the eye itself. Steroid eye drops, such as Blephamide, may be prescribed. Styes are also common with ocular rosacea. Mild cases of ocular rosacea can be managed by applying warm compresses to the area, using artificial tears, and practicing good eyelid hygiene, including cleansing the lids and lashes with watered-down baby shampoo or a gentle eyelid cleanser.
What treatments are good for rosacea?
Effective rosacea treatment typically combines medical therapies and lifestyle adjustments tailored to the individual’s symptom pattern. Many patients benefit from prescription topical medications that reduce inflammation, calm redness, and help control acne-like breakouts, especially in milder cases. Oral medications may be prescribed when rosacea presents with persistent bumps or pustules that do not improve with topical care alone. In-office procedures are often used to address symptoms that topical treatments cannot adequately control, such as widespread redness or visible blood vessels. Gentle skincare, daily sun protection, and avoidance of known triggers are essential for supporting medical treatments and maintaining long-term improvement. A comprehensive plan designed by a board-certified dermatologist allows multiple treatments to work together and keep rosacea symptoms under control.
Will laser treatment help rosacea?
Laser treatment can be an effective long-term strategy for improving rosacea symptoms. However, because rosacea is a chronic inflammatory skin condition, laser therapy does not eliminate the underlying tendency toward redness. Instead, it helps reduce visible flare-ups, such as redness and enlarged blood vessels, which can otherwise become more pronounced over time. Many patients notice gradual improvement after a series of laser sessions, with maintenance treatments helping to preserve results, as new blood vessels may form. The degree of improvement varies by rosacea subtype, skin sensitivity, and trigger exposure, which is why laser therapy is often combined with topical treatments, gentle skincare, and lifestyle adjustments. A board-certified dermatologist can determine whether laser treatment is appropriate and how it fits into a comprehensive plan to keep symptoms controlled and skin calm and balanced.

Before & After photo: VBeam laser to treat Rosacea
What laser treatment is best for rosacea?
VBeam Laser Treatment
The VBeam pulsed dye laser (PDL) is the gold standard for eliminating facial redness associated with rosacea. The V-Beam laser operates at 595 nm, specifically targeting the red pigment in the skin while leaving surrounding tissue untouched. This makes it an ideal treatment for reducing facial redness associated with flushing and visible blood vessels in rosacea. The pigment within blood vessels absorbs the laser energy, destroying them. Because the laser targets red pigment, the V-Beam not only effectively treats rosacea but also diminishes the appearance of stretch marks, post-inflammatory hyperpigmentation, acne scars, broken capillaries, surgical scars, and more. Patients appreciate that the V-Beam laser treatment involves no downtime and can be completed in minutes, allowing them to resume their usual daily activities immediately after the procedure. Additionally, the laser is equipped with a patented Dynamic Cooling Device that emits a burst of cool air before each laser pulse, thereby enhancing patient comfort during the treatment.
Most patients do not require numbing cream for V-Beam laser treatment. Patients with very sensitive skin or those treating a larger body area may choose to use numbing cream. In that case, Dr. Green can send a prescription for topical numbing cream to your preferred pharmacy. Apply the cream to the entire treatment area in a thick layer one hour before your laser treatment. When you arrive at Dr. Green’s private dermatology office on Manhattan’s Upper East Side, the numbing cream will be removed and the skin sterilized to prepare you for the laser treatment.
Typically, patients need between four and six treatment sessions to reduce the appearance of rosacea and achieve their ideal cosmetic results. Staying consistent with the treatment schedule helps support the best results. The American Academy of Dermatology reports that most patients see a 50–75% reduction in visible blood vessels after the first three laser treatments, and many achieve a 100% reduction. Because rosacea is a chronic skin condition with symptoms that may come and go, patients may require additional treatments for future flare-ups.
Intense Pulsed Light (IPL) Therapy
IPL treatment, also known as photo rejuvenation or a photo facial, is an anti-aging procedure that uses various wavelengths of light to address a range of skin conditions, including facial redness and broken blood vessels related to rosacea. When the IPL device is applied to the skin, it emits light that is absorbed by the red pigmentation, helping reduce rosacea symptoms. Patients with recurrent rosacea symptoms generally need an average of 4 to 6 IPL treatment sessions, each scheduled approximately four weeks apart, to achieve the desired final results. Most patients also undergo an annual maintenance treatment session to maintain optimal results.
Photodynamic Therapy for Rosacea
Photodynamic therapy (PDT) is a non-invasive treatment for conditions such as rosacea, skin cancer, precancerous lesions, psoriasis, and age-related macular degeneration. The PDT process consists of two parts: first, a topical photosensitizer—a chemical sensitive to a specific wavelength of light—is applied to the treatment area. In the second part, the targeted wavelength of light activates the photosensitizer at the treatment site. Once the photosensitizer is activated by light, it generates oxygen radicals that destroy the targeted cells that have absorbed it. Various sources of PDT light are available, including lasers, intense pulsed light, blue light, red light, and visible light, such as natural sunlight. It is highly recommended to avoid direct sunlight or other direct light in the treatment area for 24 to 72 hours after your Photodynamic Therapy procedure. Typically, a series of three to five Photodynamic Therapy treatments is conducted at four-week intervals. Dr. Green will determine the number of sessions needed during your consultation, based on the severity of your rosacea.
Red and Blue Light Therapy with HydraFacials for Rosacea
A HydraFacial is a three-step, medical-grade facial that improves skin health and appearance while being gentle enough for patients with sensitive skin, including those with rosacea. HydraFacial infuses specialized skincare serums into the skin using innovative vortex technology while cleansing and extracting impurities. The treatment first deeply cleanses the skin, then gently exfoliates it. During exfoliation, dirt, debris, and dead cells are removed from pores, helping minimize acne and keep pores clear. The final step infuses the skin with beneficial antioxidants and peptides to nourish, hydrate, and protect it. The Rozatrol Booster is specifically designed to complement your HydraFacial and enhance the appearance of facial rosacea. Red/Blue Light Therapy, in the form of LED light therapy, helps reduce facial redness and pustules by improving blood circulation in the treatment area and eliminating acne-causing bacteria on the skin. Dr. Green incorporates this light therapy into the medical-grade HydraFacial for rosacea. Not only do HydraFacials treat acne, rosacea, and facial redness, but they also effectively address uneven skin tone and texture. HydraFacials are recommended monthly treatments to improve facial tone and texture, reduce red and brown spots, and reduce enlarged pores.

VBeam for Rosacea – 4 months
Which laser treatment is best for rosacea?
The most effective laser treatments for rosacea target the blood vessels responsible for persistent redness and flushing. Vascular lasers deliver energy to hemoglobin within dilated blood vessels, allowing those vessels to fade gradually while leaving the surrounding skin unharmed. This makes these lasers particularly well-suited for patients whose rosacea presents with visible capillaries or diffuse facial redness that does not respond fully to topical medications. The best laser choice depends on factors such as the severity of redness, the depth of the blood vessels, skin sensitivity, and overall skin tone. A board-certified dermatologist evaluates these characteristics during a consultation to select the laser technology that will provide the most reliable improvement while minimizing irritation and downtime. In certain cases, a YAG laser may be considered for treating deeper or more prominent blood vessels. The most appropriate type of laser treatment depends on how redness and blood vessels appear on the skin.
Which medication is most effective in treating rosacea?
Oral medications, including antibiotics and Isotretinoin, are typically reserved for moderate-to-severe rosacea. These treatments may also be recommended when symptoms include bumps or pimple-like breakouts. Dr. Green often prescribes an oral antibiotic such as doxycycline, Oracea, or Flagyl (Metronidazole) to manage rosacea and clear pimple-like breakouts for her patients. Once the pimple-like breakouts associated with rosacea have resolved, patients may be able to discontinue oral antibiotics and manage other rosacea symptoms with topical treatments. Oral antibiotics are not considered a long-term solution for rosacea due to potential side effects associated with prolonged use. The main side effects of chronic oral antibiotic use include yeast infections, gastrointestinal upset, and photosensitivity. Notify the prescribing healthcare provider of any side effects you may experience while taking oral antibiotics. Ocular rosacea, a type of rosacea that affects the eyes, can be treated with oral antibiotics, eye washes, and antibiotic eye drops. In more severe cases of ocular rosacea, Dr. Green will refer you for a consultation with a board-certified ophthalmologist.
In some cases, Dr. Green may recommend Isotretinoin (Accutane) to treat chronic papules or pustules caused by rosacea. Isotretinoin is not an oral antibiotic but an oral medication derived from vitamin A. Although Isotretinoin is typically used to treat traditional acne vulgaris, it can also effectively treat rosacea pustules. Isotretinoin works by accelerating skin cell turnover and reducing the size and activity of the skin’s oil glands. Most patients require a five-month course to clear their pimples, and the majority do not experience a recurrence of breakouts. The most common side effect of Isotretinoin is dry skin. To determine whether you would benefit more from oral antibiotics, Isotretinoin, or another alternative, Dr. Green will review your medical history and physically assess your skin condition.
What is the best topical treatment for rosacea?
To treat rosacea symptoms and prevent future flare-ups, the best dermatologists, such as Dr. Michele Green in NYC, will review your skincare regimen. Because patients with rosacea have some of the most sensitive skin, Dr. Green will always recommend gentle skincare products, including cleansers and non-comedogenic, oil-free moisturizers to nourish and soothe the skin. Recommendations are adjusted based on skin type, as sensitivity and tolerance can vary significantly from person to person. The topical treatments listed below are typically prescribed first, especially if rosacea symptoms are mild. Her personalized recommendations for topical treatments and skincare products will depend on her in-person evaluation of your skin condition and a discussion of your medical and family history. Some of the best prescription topicals for rosacea skincare include:
- Metrogel, also known as Metronidazole cream, is a classic topical medication that prevents and treats facial rosacea and its associated redness by reducing inflammation and inhibiting bacterial growth on the skin.
- Soolantra (Ivermectin) is an excellent choice for reducing inflammation and facial redness characteristic of rosacea.
- Mirvaso (Brimonidine) gel is a topical cream that reduces the appearance of visible blood vessels associated with rosacea and is applied once daily.
- Rhofade (Oxymetazoline) is a topical cream similar to Mirvaso because it constricts blood vessels, thereby reducing facial redness. Rhofade should be used only once a day, too.
Best skincare products for rosacea
Patients with rosacea can greatly benefit from a skincare regimen that includes the right active ingredients to minimize their symptoms. Internationally renowned board-certified dermatologist Dr. Michele Green has developed a line of topical skincare products that effectively reduce redness and help maintain a clear complexion. Three essential skincare products for patients with rosacea include Vitamin C, sunscreen, and a moisturizer.
Vitamin C Serum is an excellent antioxidant that offers many benefits, including reducing facial redness and rejuvenating the skin by stimulating new collagen production and accelerating skin cell turnover. Dr. Green’s best-selling Vita-C-Serum from her proprietary line, MGSKINLABs, is ideal for patients seeking to minimize facial redness, hyperpigmentation, and discoloration.
Sun exposure can worsen rosacea symptoms, so limiting sun exposure and using proper sun protection is essential. Dr. Green’s number one rosacea skin care tip is to use a fragrance-free, non-comedogenic, broad-spectrum sunscreen with a minimum SPF of 30 to protect the skin without irritating it. When sunscreen is labeled broad-spectrum, it indicates protection against both UVA and UVB rays. Dr. Green has specially formulated the Hydrating Sunscreen with SPF 50 from her MGSKINLABs line of skincare products, which provides broad-spectrum coverage and a silky finish to ensure sun protection and comfort.
Moisturizer is a crucial step in any skincare regimen, especially for patients with rosacea. It helps strengthen and repair the skin’s natural barrier. A healthy skin barrier retains moisture and protects against external irritants and environmental triggers that can worsen rosacea symptoms. Many patients with rosacea who experience acne-like breakouts prefer a lightweight, oil-free moisturizer that won’t clog pores. MGSKINLABs Ultimate Sheer Hydrating Lotion is ideal for sensitive skin because it is rich in aloe and rosewater, instantly hydrating the skin without feeling heavy or clogging pores.
When you consult with Dr. Green, you will have the opportunity to discuss a proper skincare routine, including which products should be part of your regimen. She will work with you to create a customized skincare protocol that incorporates the right topical medications and products to give you a healthy, clear, smooth complexion that lasts.
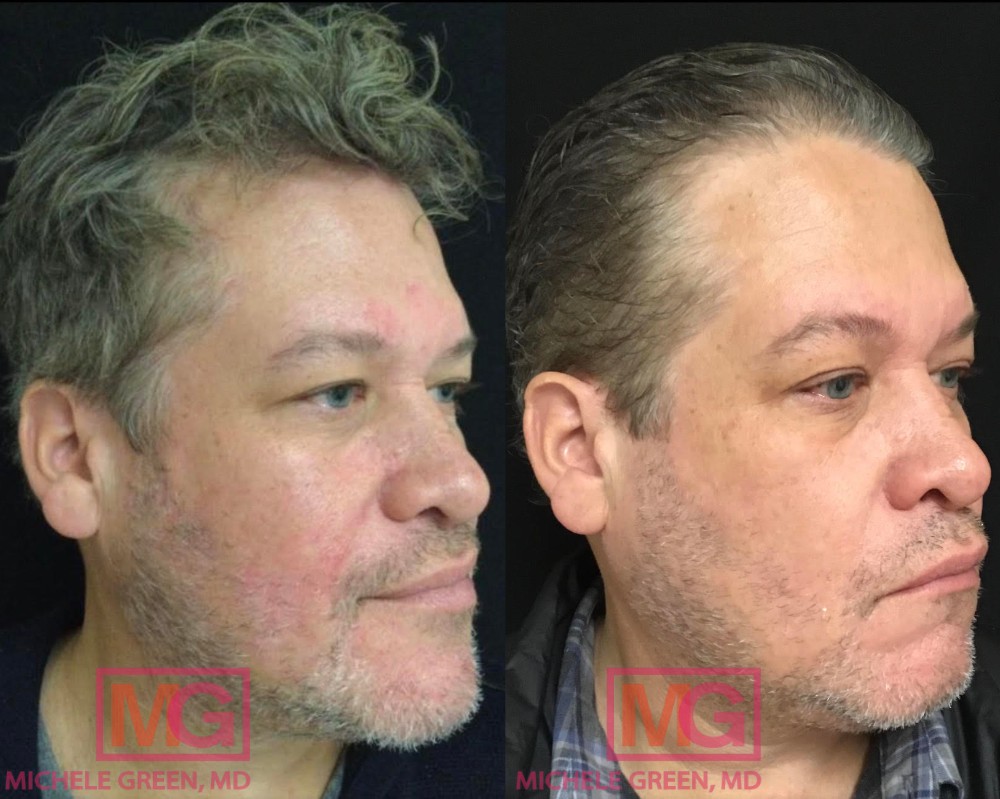
What are the best treatments for rosacea?
Rosacea has no cure, but several treatment options can help manage its symptoms and improve the skin’s appearance and feel. Treatment aims to control visible skin changes and reduce the disruption caused by flare-ups. Different therapies are used depending on how rosacea appears, such as redness, visible blood vessels, or inflammatory breakouts. Some approaches target changes beneath the skin’s surface, while others work at the surface. Many patients benefit from using multiple treatments over time, as rosacea can change in intensity and appearance. The most effective results are typically achieved when treatments are selected based on individual symptoms and adjusted as the condition evolves, allowing patients to manage their rosacea.
Rhinophyma and treatment options
Rhinophyma is characterized by large, red bumps on the nose that grow larger and become bulbous. It is believed to develop gradually over many years when rosacea is poorly treated or left untreated. The large masses that form at the tip of the nose result from thickened, firm skin, and for many, this presents a serious cosmetic concern. Rhinophyma affects men more often than women, and the condition tends to worsen with age. As rhinophyma advances clinically, there is typically an increase in facial redness, skin thickening, a rough, waxy epidermal appearance, enlarged facial pores, and a rise in the number and size of sebaceous glands. Treating rhinophyma is challenging because it generally responds poorly to oral or topical antibiotics once it has developed. Isotretinoin (Accutane) can help reduce sebum overproduction and inflammation.
Typically, surgery is the most effective treatment for rhinophyma, as the overgrowth of blood vessels and tissue often causes facial disfigurement around the nose. The primary therapeutic and surgical approaches to rhinophyma include traditional surgery, CO2 laser resurfacing, and cryosurgery. Using these surgical and laser modalities, the shape of the nose can be restored, and tissue overgrowth can be cosmetically improved.
How many laser treatments for rosacea?
The number of laser treatments needed for rosacea varies depending on how redness and visible vessels are present on the skin, and there is no single fixed number that applies to everyone. Many patients notice meaningful improvement after a short series of sessions, and many physicians recommend a course of treatments spaced several weeks apart so that changes in the skin can be assessed progressively. In general, a typical range is 4 to 6 treatments. Treatment plans are often adjusted based on how the skin responds and the persistence of the redness. Some individuals see noticeable changes early in their series and choose to reduce frequency, while others continue with a fuller course to maximize improvement. Some patients choose to return for occasional maintenance treatments over time, as rosacea is a chronic condition and new blood vessels can gradually develop even after successful initial laser sessions.
How much are laser treatments for rosacea?
The cost of laser treatments for rosacea varies widely depending on the treatment plan and the provider. Pricing is influenced by the practice’s geographic location, with treatment costs in major metropolitan areas often higher than in smaller cities or suburban areas. The total cost is also affected by the type of laser or light-based technology used and the number of sessions recommended to achieve the desired level of improvement, as a series of treatments is often required. The experience and training of the provider performing the laser treatment can also play a role, as care delivered in a medical setting by a board-certified dermatologist may differ in cost from treatment offered in non-medical environments. Since laser treatments for rosacea are typically considered cosmetic, they are not usually covered by insurance. During a consultation, patients can discuss their goals and receive a personalized estimate based on their skin concerns and the type of treatment needed.

VBeam, 2 sessions, 2 months before and after
Frequently Asked Questions (FAQs) about Rosacea
Who treats rosacea?
Rosacea is typically managed by a healthcare professional who determines the best treatment plan and monitors changes in the skin over time. Care often begins with a medical evaluation, especially when symptoms are persistent, worsening, or affecting daily comfort. In cases where rosacea involves the eyes, additional care may be provided by an ophthalmologist to address irritation or visual symptoms. Treatment decisions are based on the location of rosacea, the severity of redness, and the response to treatment. Medical oversight ensures appropriate monitoring and that care is adjusted throughout the entire treatment process.
Can you get rid of rosacea permanently?
Visible broken blood vessels treated with laser therapy will not return, although new ones may develop. Unfortunately, no treatment for rosacea yields permanent results, as it is a chronic skin condition with symptoms that continually progress.
Unfortunately, there is no cure for rosacea. Rosacea is a chronic skin condition, and its symptoms may come and go. It is possible to manage and treat rosacea symptoms with various treatment options, including oral antibiotics, Isotretinoin, light or laser treatments, and topical medications. Limiting exposure to common rosacea triggers can also be helpful. The first step in developing a safe and effective rosacea treatment plan is to schedule a consultation with an experienced, board-certified dermatologist, such as Dr. Michele Green.
Can laser treatment help rosacea?
Laser treatment can play an important role in managing many visible symptoms of rosacea, particularly persistent facial redness and visible blood vessels. Vascular lasers, such as the VBeam pulsed dye laser, target hemoglobin in dilated blood vessels, allowing the laser energy to reduce redness while selectively leaving the surrounding skin intact. This approach can significantly improve background redness, flushing, and broken capillaries that do not respond well to topical medications alone. Laser treatment is especially helpful for patients whose rosacea presents primarily as diffuse redness or visible vessels, as these symptoms are driven by vascular changes in the skin rather than surface inflammation. When performed as part of a customized treatment plan, laser therapy can lead to clearer, more even-looking skin and fewer visible signs of rosacea over time.
Why is there no cure for rosacea?
There is no cure for rosacea because it is a chronic condition influenced by a combination of factors rather than a single cause. Rosacea is a chronic skin condition with symptoms that may fluctuate. However, various treatment options are available to manage symptoms, prevent flare-ups, and minimize their appearance on the skin’s surface. Light therapies and laser treatments are excellent choices for patients looking to reduce the risk of broken blood vessels and promote skin healing during and after a flare-up. The key to successfully treating rosacea is maintaining proper skin care, using adequate sun protection, following a healthy, anti-inflammatory diet, and avoiding known triggers. Many patients with rosacea may be sensitive to certain skincare products, including sunscreens. If sunscreens are too irritating for topical application, pure zinc oxide can shield the skin from sun exposure and help prevent rosacea flares. Additionally, many topical prescription creams, gels, and lotions can be safely used alongside other treatments to alleviate rosacea symptoms effectively.
Will rosacea go away on its own?
Rosacea is a chronic skin condition that does not go away and has no cure. It can flare intermittently. Fortunately, a range of treatment options and lifestyle modifications can help manage symptoms and prevent flare-ups. Common triggers for rosacea flare-ups include caffeine, alcohol, sun exposure, hot or cold weather, spicy foods, strenuous exercise, wind exposure, and stress. Because it can worsen if left untreated, it is essential to consult an expert dermatologist for monitoring and treatment of rosacea. Dr. Green is a board-certified dermatologist with over 25 years of experience diagnosing and treating all types of rosacea. She works with patients experiencing rosacea symptoms for the first time and those who have dealt with flare-ups for years, and she can develop a sustainable treatment plan that best fits your current needs.
Do laser treatments help rosacea?
Laser treatments can help improve many visible signs of rosacea, particularly persistent facial redness and prominent blood vessels that do not respond well to topical care alone. These treatments work by delivering targeted energy into the skin to reduce dilated blood vessels and calm vascular activity, thereby lessening the flushed appearance that often develops with repeated flare-ups. Many patients notice gradual improvement over a series of sessions, as redness becomes lighter and less noticeable, and the overall complexion appears more even. Laser treatments are not a cure for rosacea, but they can play an important role in long-term management. When used as part of a comprehensive treatment plan and supported by appropriate skincare and follow-up care, laser treatments can help keep rosacea symptoms better controlled and reduce the frequency of visible flare-ups.
What is the most effective rosacea treatment?
The most effective rosacea treatment is tailored to how the condition presents on an individual’s skin. Rosacea can involve redness, flushing, acne-like breakouts, skin thickening, or eye irritation, and each feature responds best to different treatments. Inflammatory bumps may improve most with prescription medications, while persistent redness and visible blood vessels are often best managed with laser or light-based treatments. Long-term effectiveness also depends on maintaining results through appropriate skincare and sun protection. The most effective treatment approach addresses both active symptoms and the factors that contribute to flare-ups over time.
Does insurance cover laser treatment for rosacea?
Most oral antibiotics and topical treatments prescribed by a healthcare provider, such as a board-certified dermatologist, to treat rosacea are covered by insurance. Laser treatments for rosacea, such as the VBeam laser and IPL, are usually considered cosmetic procedures by insurance companies and are typically not covered. The best way to determine whether your insurance will cover rosacea treatment is to call the phone number on your insurance card.
How long does it take for rosacea to clear up?
Rosacea does not clear up on a fixed timeline because the condition varies widely in symptom pattern, severity, and treatment adherence. Some patients notice improvement in redness, irritation, or breakouts within several weeks of starting treatment, while others may require a few months before changes become more noticeable. In-office treatments such as laser therapy often produce gradual improvement over a series of sessions, with results continuing to develop as the skin heals. Long-term control usually takes time, as rosacea is a chronic condition that responds best to consistent care. With a personalized treatment plan and regular follow-ups, many patients reach a point where their symptoms are well-controlled and stable. Although rosacea itself does not fully resolve, seeking treatment with a board-certified dermatologist can lead to a more even appearance over time.
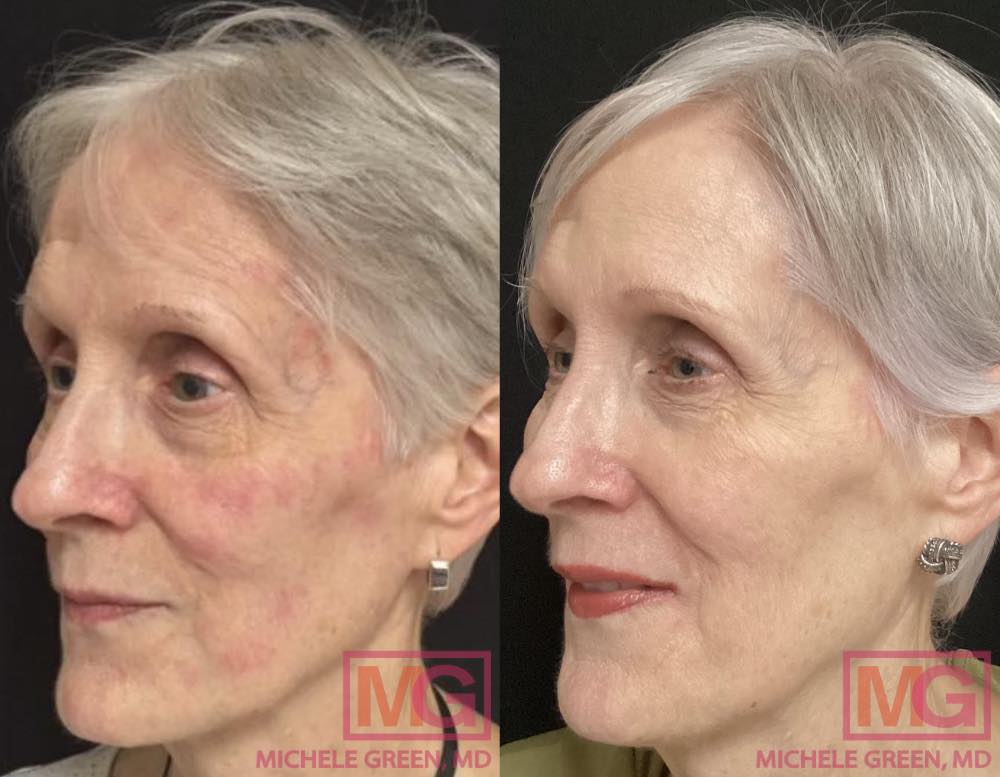
What facial treatments are good for rosacea?
Facial treatments appropriate for rosacea focus on soothing the skin and supporting barrier function without irritating it. Medical-grade facials designed for sensitive or reactive skin cleanse and hydrate the skin while avoiding aggressive exfoliation or harsh ingredients that may worsen redness. Treatments such as HydraFacial can be used for rosacea-prone skin because they gently cleanse and hydrate the skin while infusing calming serums that support skin comfort. During a HydraFacial, a targeted serum such as the Rozatrol Booster may be added to help reduce the appearance of facial redness and support skin balance without overstimulating sensitive skin. LED light therapy, particularly red and blue light treatments, may also be incorporated into facial care to help calm visible redness and improve the overall appearance of inflamed skin. These treatments may also support skin rejuvenation by improving overall tone and texture. The most effective facial treatments for rosacea are those carefully selected based on how the skin responds, as overly stimulating procedures can increase sensitivity and prolong flare-ups.
What happens if you don’t treat rosacea?
If rosacea is left untreated, it often becomes more persistent and noticeable over time. Early flushing and redness that come and go can gradually become constant redness that is harder to improve and easier to trigger. Visible blood vessels may become more pronounced as repeated inflammation keeps them enlarged rather than returning to their normal size. In some individuals, untreated rosacea can lead to thickened skin, particularly on the nose, where gradual tissue changes may alter facial contours. Eye-related symptoms can also worsen without treatment, leading to ongoing irritation, dryness, or discomfort that may interfere with daily activities. While rosacea is not dangerous, allowing it to progress without care can make symptoms more difficult to manage later on and increase the likelihood that visible changes become long-lasting.
What is best for rosacea treatment?
The best rosacea treatment plan is customized and responsive to how the condition presents on a person’s skin over time. Rosacea can involve facial redness, flushing, visible blood vessels, acne-like breakouts, skin sensitivity, and, in some cases, eye irritation. No single treatment works for everyone. Some patients benefit most from prescription topical medications that calm inflammation and reduce flare-ups. In contrast, others require in-office procedures to address persistent redness and vascular changes that do not improve with creams alone. Long-term success also depends on proper skincare, consistent sun protection, and avoiding personal triggers that worsen symptoms. A comprehensive treatment plan guided by a board-certified dermatologist allows therapies to be adjusted as rosacea evolves, helping maintain clearer, calmer skin and prevent symptoms from becoming more pronounced over time.
How to treat rosacea naturally?
Managing rosacea naturally involves gentle skincare and lifestyle changes that reduce inflammation and minimize triggers. Skincare products should be free of irritating ingredients such as fragrance and alcohol, which can cause redness, dryness, and worsen rosacea. Before starting any new skincare products, individuals with rosacea should perform a small patch test to ensure there is no irritation. Additionally, using a broad-spectrum sunscreen with an SPF of 30 or higher can help minimize sun damage, which can exacerbate rosacea symptoms. Patients should aim to eat a well-balanced diet and avoid common triggers such as spicy foods, alcohol, and caffeinated beverages like coffee. Stress is another significant trigger for rosacea, so managing it through various techniques can help lessen rosacea symptoms.
Will rosacea go away with treatment?
Rosacea does not go away completely with treatment, but appropriate care can significantly reduce its appearance and help keep symptoms under control for extended periods. Treatment works by calming chronic skin inflammation and minimizing the underlying processes that cause persistent redness and flare-ups, allowing the skin to appear more even over time. Many patients notice that once treatment starts, their rosacea behaves more consistently, with fewer unexpected flares and less sensitivity to everyday environmental factors. Consistency is important, as stopping treatment or neglecting ongoing care can allow symptoms to return gradually. With a well-managed approach and regular monitoring, treatment can help maintain long-term improvement and prevent rosacea from worsening.
Does rosacea need to be treated?
Rosacea does not always require immediate treatment in mild cases, but leaving it unmanaged can make symptoms more persistent and harder to control over time. Early signs, such as occasional flushing or mild redness, may seem manageable at first, but rosacea often progresses gradually. Over time, redness lasts longer, flare-ups occur more frequently, and changes become more visible. Treating rosacea not only improves appearance but also maintains skin comfort and prevents worsening. When rosacea is addressed early, symptoms are often easier to manage. Although rosacea is not dangerous, treating it can reduce symptoms and help individuals feel more comfortable and confident in their appearance.
What laser treatment for rosacea?
Laser treatment for rosacea includes several light-based technologies used to improve persistent redness and visible blood vessels that develop over time. One commonly discussed option is pulsed-dye laser treatment, often referred to as VBeam, which targets red pigment in dilated blood vessels and gradually reduces their appearance, helping the skin look more even and less flushed. Intense pulsed light therapy is another option that may be used to address more diffuse redness across broader areas of the face, particularly when flushing is widespread. In certain situations, photodynamic therapy may also be considered to help reduce inflammation while improving overall skin tone. Each of these treatments works in a slightly different way, with differences in wavelength, depth of penetration, and the precision with which energy is delivered to the skin. The most appropriate laser or light-based treatment depends on how rosacea presents, including the pattern of redness, the presence of visible vessels, and overall skin sensitivity, which is why a consultation is important to determine which approach is best suited to achieving clearer-looking skin.
What is the best treatment for rosacea on the face?
The best treatment for facial rosacea focuses on calming visible inflammation while protecting the delicate facial skin, which is often more reactive than skin on other parts of the body. Facial rosacea is especially sensitive to environmental exposure, temperature changes, and daily skincare habits, making targeted management essential. Treatment is most effective when it improves skin tone, reduces persistent redness, and prevents future flare-ups that can develop over time if rosacea is left unmanaged. Maintaining comfort and preventing irritation is also important, as facial skin with rosacea can easily become inflamed. A carefully guided approach helps keep facial rosacea controlled, helping the complexion look more even while reducing the likelihood of visible flares returning.
What type of doctor treats rosacea?
A board-certified dermatologist is best suited to treat rosacea, a specialist focused on conditions of the skin, hair, and nails. Dermatologists are trained to recognize subtle differences between rosacea and other skin conditions that may look similar, such as acne or eczema, which is important for accurate diagnosis. They also understand how rosacea can change over time and how different subtypes may respond to different approaches. A dermatologist evaluates the pattern and severity of the rosacea on the skin and determines the best treatment plan to target redness. They are also trained to monitor progression and adjust care as symptoms evolve, helping prevent rosacea from becoming more persistent or noticeable over the long term.
How to get started with rosacea treatment today
Rosacea laser treatment offers a non-invasive way to reduce persistent facial redness, visible blood vessels, and flushing, which can become more noticeable over time. Laser technology targets vascular changes beneath the skin’s surface, allowing redness to fade gradually and the complexion to appear more even. These treatments are commonly used by individuals who find that topical care alone does not adequately address redness or dilated capillaries. Laser therapy can be performed with minimal downtime and is often incorporated into a broader rosacea treatment plan. Many rosacea treatment options fall within cosmetic dermatology, where the focus is on improving visible redness and skin tone. Results develop gradually as the skin responds and heals after treatment. An experienced board-certified dermatologist, such as Dr. Green in NYC, will evaluate your skin and create a personalized approach to rosacea that supports long-term improvement and skin comfort.
Dr. Michele Green is an internationally acclaimed, board-certified dermatologist with over 25 years of experience providing advanced, non-invasive treatments for chronic skin conditions, including rosacea. She takes a personalized approach to rosacea, carefully selecting procedures that calm inflammation, reduce visible redness, and support overall skin balance, even for those with sensitive skin. Frequently recognized as one of New York City’s leading dermatologists by Super Doctors, Castle Connolly, and New York Magazine, she is known for her expertise and dedication to patient care. When you schedule a consultation with Dr. Green at her private boutique on Manhattan’s Upper East Side, she will work with you to develop a personalized rosacea treatment plan tailored to your skin concerns and goals. Please call Dr. Michele Green’s NYC office at (212) 535-3088 to book a consultation or contact us online today.
 212-535-3088
212-535-3088 



