Photodynamic Therapy
What is Photodynamic Therapy (PDT)?
Photodynamic therapy (PDT) is a cutting-edge medical procedure that targets skin cancer cells and precancerous skin lesions called actinic keratoses. PDT also treats other medical conditions, such as acne, psoriasis, various head and neck cancers, age-related macular degeneration, and premature antiaging caused by sun damage. Unlike radiation or surgery, treatment with photodynamic therapy is non-invasive, meaning patients can look forward to little to no side effects or downtime following the procedure. In her private New York City dermatology office, Dr. Michele Green utilizes PDT in her patient’s treatment plans to treat skin cancers, precancers, sun damage, and acne.
Photodynamic therapy is a two-step treatment: the first step involves topically administering a photosensitizing agent to the treatment area to be absorbed by the target cells. The second step involves using a distinct wavelength of light to activate the photosensitizing agent to treat the target cells. Blue light treats activin keratoses or skin cancer cells, while other light sources, such as red light, laser light, or light-emitting diode (LED) light, are used to treat other medical or cosmetic concerns. Photodynamic therapy does not harm the surrounding skin or tissues during the procedure, allowing patients to resume their daily activities following treatment. Additionally, no long-term side effects are associated with the treatment, making it a safe and effective treatment option for cancers and other skin concerns. If you want to treat superficial skin cancers, precancerous lesions, or other skin conditions with photodynamic therapy, consult Dr. Michele Green today.
In New York City, experienced, board-certified dermatologist Dr. Michele Green has over two and a half decades of experience treating her patients with non-invasive procedures, including PDT. Castle Connolly, New York Magazine, Super Doctors, and The New York Times consistently identify Dr. Green as one of the best physicians in New York for her expertise and dedication to patient care. Dr. Green has been recognized as an international expert in dermatology, using treatments such as PDT to remove photodamage and precancerous lesions without any unnecessary side effects or long recovery times. After carefully assessing your skin lesions or concerns, Dr. Green will tailor a treatment plan to your needs to help you achieve healthier, clearer, more youthful-looking skin.
What is Photodynamic Therapy (PDT)?
Photodynamic therapy, also called phototherapy, is a unique treatment that uses a combination of light-sensitizing medication and light to treat cancer cells and other skin conditions. Photodynamic therapy may involve blue, red, laser, or light-emitting diode (LED) light, depending on the skin condition or type of cancer being treated. PDT was first FDA-approved for bladder cancer treatment in 1993 and subsequently approved to treat actinic keratoses, or precancerous lesions, in 2004. Variations of PDT are also used to treat different conditions, including age-related macular degeneration, sun damage, acne, and psoriasis. Many patients love PDT as treatment requires little downtime or side effects. Compared with some other cancer treatments, PDT is less likely to result in metastasis and does not damage DNA like some other cancer treatments do. Multiple PDT treatment sessions may be required to achieve the final desired results, depending on the type and variety of the skin concern. When you consult with board-certified dermatologist Dr. Michele Green at her private dermatology office in Manhattan’s Upper East Side neighborhood, she will work with you to create a customized treatment plan that incorporates the procedures best suited to your unique skin condition, including PDT if necessary.
How does photodynamic therapy work?
Photodynamic therapy requires two steps for full and effective treatment: administering and incubating a photosensitizing agent and activating the light. First, the photosensitizing agent is administered to the patient via topical application to the affected skin area. Aminolevulinic acid (ALA or Levulan) and Porfimer sodium (photofrin) are PDT’s two most widely used photosensitizing agents. Levulan is used to treat precancerous actinic keratoses and other forms of skin cancer, while Photofrim is used to treat certain forms of lung and esophageal cancer. Levulan is activated with blue light, while photofrin is activated by red laser light.
Over several hours to 72 hours (depending on the type of photosensitizing agent), the drug will travel through the patient’s body and leave the normal cells. However, the photosensitizing drug remains in the cancerous cells or target cells. During incubation, the photosensitizer drug is non-toxic and does not affect the cells or tissue. The drug only becomes activated when a specific light is shone onto the treatment area. Once activated, the photosensitizing drug produces a particular form of oxygen, known as an oxygen radical, that targets and kills the cells that have absorbed the drug. Activation can also cause damage to the blood vessels in the treatment area, which prevents blood from reaching the cancerous cells.
What is photodynamic therapy used to treat?
According to the National Cancer Institute, photodynamic therapy (PDT) can be used in cancer care to treat advanced cutaneous T-cell lymphoma, Barrett’s esophagus, throat cancer (also known as esophageal cancer), and non-small cell lung cancer. PDT can also treat non-melanoma skin cancers such as basal cell carcinoma or stage 0 squamous cell carcinoma (also known as Bowen’s disease) and precancerous lesions called actinic keratoses. Certain cancer symptoms can also be relieved with the help of PDT treatment, including reducing throat blockage that occurs as a result of esophageal cancer and blocked airways that result from non-small cell lung cancer. In addition to cancer treatment, PDT can address several other conditions affecting the skin, including psoriasis, acne vulgaris, age-related macular degeneration, and warts.
What is blue light photodynamic therapy?
Blue light photodynamic therapy is a specific kind of PDT primarily used to treat sun damage and early stages of skin cancer. These pre-cancerous skin lesions, called actinic keratoses, develop due to excess or cumulative sun exposure and can take the form of red, pink, or flesh-colored scaly patches on the skin. Many of these lesions developing on the skin’s surface may not be uncomfortable, although they can be unsightly and potentially develop into skin cancer if left untreated. Blue light photodynamic therapy works like other forms of PDT, using the photosensitizing agent known as Levulan (aminolevulinic acid or ALA) and blue light to destroy actinic keratoses. After approximately one week, the actinic keratoses legions will fade from the skin.
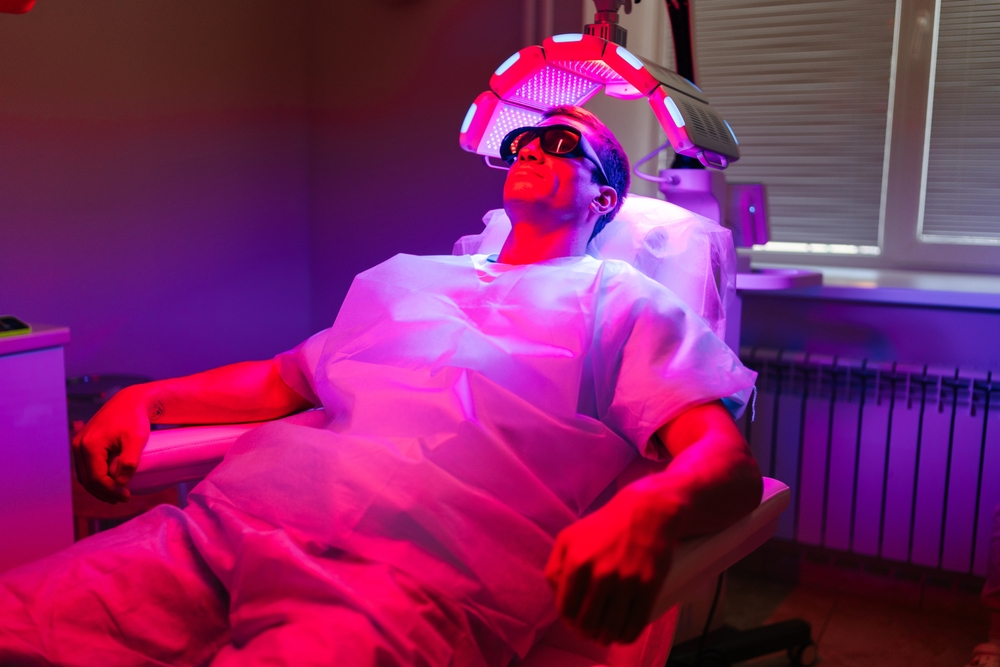
How does photodynamic therapy work for skin cancer?
Photodynamic therapy for skin cancers and precancers is a straightforward two-part process. The photosensitizing agent aminolevulinic acid, commonly known as Levulan or ALA, is applied directly to the skin in the treatment area and left for one hour. Since the normal skin barrier is not present at the sites of the actinic keratoses, the photosensitizing molecules are absorbed by pre-cancer and cancerous cells. The treatment area is then exposed to a particular wavelength of blue light, which activates the aminolevulinic acid. The activated drug then produces a chemical reaction using oxygen radicals to destroy the target cells while leaving the surrounding normal cells unaffected. The precancerous actinic keratoses will “light up,” get redder after treatment, and disappear in several days.
If you notice new or irregular skin lesions, it is always best to consult a board-certified dermatologist, such as Dr. Michele Green in NYC. A shave biopsy may be taken to send a sample of the lesion for further examination. If the lesion results in an actinic keratosis, Dr. Green can perform PDT for treatment. PDT is the optimal treatment for patients with many actinic keratosis lesions, as the procedure can treat all lesions in one area. PDT can be performed on multiple body areas, including the face, scalp, arms, legs, and chest. Multiple treatments may be required based on the amount and severity of your precancerous lesions.
How is photodynamic therapy used to treat non-skin cancers?
Photodynamic therapy (PDT) is an excellent treatment for other types of cancer unrelated to the skin, including lung and esophageal cancers. During PDT, a photosensitizing agent is absorbed into target cells and activated by specific wavelengths of light to destroy and eliminate cancerous cells. PDT can also destroy blood vessels that supply nutrients to cancer cells and alert the body’s immune system to destroy the cells further.
Porfimer sodium (photofrin) and red laser light are typically used for certain lung or esophageal cancer forms. When treating cancers inside the body, the healthcare provider will inject the photofrin intravenously — after a specific incubation time, the provider will then use an endoscope to visualize the target area and deliver laser light, activating the photofrin and destroying the cancerous cells. If you want to learn more about cancer treatment with PDT, consult with your treating physician and care team to see if PDT is right for you.
What is photodynamic therapy for acne?
While the FDA originally approved PDT for treating actinic keratoses and various types of cancers, after various clinical trials, it was determined that PDT is a safe and effective way of treating acne vulgaris, cystic acne, acne scars, and severe acne. PDT’s mechanism of action causes phototoxic damage to sebaceous glands and hair follicles, shrinking the skin’s oil glands and reducing sebum production. PDT for acne vulgaris has been proven to be a safe and effective treatment for patients with severe acne who do not respond to traditional topical acne treatments. ALA-PDT (5-aminolevulinic acid with PDT) has also been used for patients who have severe acne for whom isotretinoin (Accutane) is not an option. In addition, ALA-PDT has been proven to kill the bacteria P.acnes, which causes acne. Photodynamic therapy reduces the acne and improves the skin’s overall texture and the appearance of acne scars.
Photodynamic therapy for acne usually begins with microdermabrasion to remove the dead skin cells on the skin’s surface. Microdermabrasion before the Levulan application allows the medication to penetrate better. The Levulan is applied to the skin for 15 to 60 minutes and then removed thoroughly with water. The patient is positioned to sit in front of a blue light source for approximately 16 minutes. A series of three to five PDT treatments are typically performed in four-week intervals for acne treatment. Most patients see improvement in acne after a single treatment, with full results visible with the full treatment.

What are the possible side effects of photodynamic therapy (PDT)?
Most side effects potentially associated with PDT are minor and resolve independently within a couple of days post-treatment. The possible side effects of photodynamic therapy include:
- Redness
- Swelling
- Peeling
- Crusting
- Burning
- Sunburn
- Temporary hyperpigmentation
- Stinging
- Blisters
After treatment, patients should avoid direct sunlight and use gentle, non-irritating skincare products to reduce skin irritation. In very rare cases, depending on the part of the body and type of cancer being treated, more serious side effects may occur, including:
- Cough
- Difficulty swallowing
- Shortness of breath
- Stomach pain
Following the aftercare instructions is essential to ensure proper site healing. If you experience any side effects from PDT treatment, consult Dr. Michele Green’s office.
Who is the ideal patient for photodynamic therapy?
Photodynamic therapy (PDT) is an excellent option for patients who have had chronic sun damage throughout the years and want to treat and remove actinic keratoses or precancers. PDT allows patients to treat all precancerous lesions in an area at once without the risk of scarring, hypopigmentation, or hyperpigmentation. It is also a great option for patients with acne vulgaris who are not responding to topical or oral antibiotics. Before your procedure, you should inform Dr. Green if you have any pre-existing photosensitive conditions, such as lupus erythematous or porphyria. If you have an active herpetic or bacterial infection, Dr. Green may defer treatment until the condition resolves. When you consult with Dr. Green in her private New York City dermatology office, she will assess your medical history and skin concerns to confirm if you are an ideal candidate for treatment with photodynamic therapy.

35-44-year-old man treated with photodynamic therapy to remove red spots
What is the process of Photodynamic therapy (PDT)?
If you are interested in treatment with photodynamic therapy, please schedule a consultation with Dr. Green in her private Upper East Side dermatology office. She will first assess your medical history, skin concerns, and goals to determine if PDT is right for you. If warranted, Dr. Green may take a shave biopsy of any suspicious skin growths to receive a proper diagnosis. If PDT is recommended, Dr. Green will schedule you for the procedure later.
The first step of PDT involves applying and incubating the photosensitizing drug Levulan. First, the treatment area is cleaned of any moisturizers or sunscreens. The Levulan topical solution is applied topically to the area and allowed to air dry for a few minutes. Patients wait in the office for roughly one hour to allow the Levulan to incubate. During incubation, patients experience no discomfort. Once the incubation time has elapsed, the Levulan is removed completely with water.
The second step of PDT involves using BLU-U, or blue light. The BLU-U light source is set up six inches from the treatment area and turned on for approximately 17 minutes to activate the Levulan. Most patients prefer to sit in a comfortable chair facing the BLU-U light when treating the face. When treating other areas, such as the legs, you can lie on the exam table to complete your treatment. Eye shields are worn during the procedure to help protect your eyes from the UV blue light. Approximately 50% of patients experience stinging or burning during treatments. This burning usually plateaus within 5 to 6 minutes of treatment. A fan can be applied to cool the area during the treatment to improve patient comfort. Once the procedure is completed, SPF 50 will be applied to the treated area. Twenty-four hours after treatment, Dr. Green will have you send a photo of the treated area to confirm that the area is healing properly. Dr. Green will also schedule a follow-up appointment to reassess the treated area several weeks after your first PDT session to determine whether a subsequent session is necessary.
Avoiding sunlight, direct light, or bright indoor light in the treatment area for 24-72 hours post-treatment is essential, as Levulan increases the skin’s photosensitivity. If treating the face, sunglasses and a wide-brimmed hat should be used. If treating an area of the body, protective clothing can be used to shield the area from sun exposure. After the treatment, sunscreen is also essential to prevent future sun damage and pre-cancers. Patients should continue using broad-spectrum sunscreen with a minimum SPF of 50 to protect against UVA and UVB rays. Patients should also avoid sitting or standing near windows, as UV rays can penetrate window glass. When you have photodynamic therapy with Dr. Green, she will provide you with all the pertinent aftercare information required to achieve and maintain the best results.
How long does it take to recover from photodynamic therapy?
Patients are thrilled with this procedure, as it has minimal downtime and is an outpatient procedure, meaning patients may return home immediately after the treatment. Some common side effects of PDT treatment include a sunburn-like quality to the skin in the treatment area, including redness, itchiness, swelling, and, in some more severe cases, blistering. Any unwanted side effects from the BLU Light procedure should resolve within 2-3 days. Certain photosensitizing agents may also cause increased sensitivity to light for some time after receiving treatment. One type of photosensitizer drug, called porfimer sodium, which is used to treat some forms of lung and esophageal cancer, can be associated with sensitivity to light for as much as six weeks post-treatment. Patients should avoid direct sunlight, bright indoor lights, and reflective surfaces for the time specified by their healthcare provider.
Patients are advised not to go into saunas or steam rooms for the first few days, as heat exposure can cause skin irritation in the treated area. It is also recommended to avoid using any exfoliating skincare products, including retinoids or alpha hydroxy acid creams, until the area has healed completely. Dr. Green recommends applying a fragrance-free, non-comedogenic moisturizer to the treated area for at least one week to promote healing. It is advised not to pick or scrub the skin after the procedure as this could lead to scarring or infection. Patients can take acetaminophen (Tylenol) or another mild pain reliever if any discomfort occurs after the procedure. When you have photodynamic therapy with Dr. Green at her private dermatology office in Manhattan’s Upper East Side neighborhood, she will provide the pertinent aftercare information required for achieving and maintaining the best results.
Is photodynamic therapy safe?
Absolutely! Photodynamic therapy is a safe and effective treatment for various cancers and skin conditions. The treatment’s side effects are usually fairly mild, including redness, swelling, and skin surface irritation, and they resolve quickly following the treatment. The noninvasive treatment means no surgery is necessary, so it is much lower risk and does not cause scarring. Further, unlike other common cancer therapies, PDT therapy does not damage healthy, normal cells.
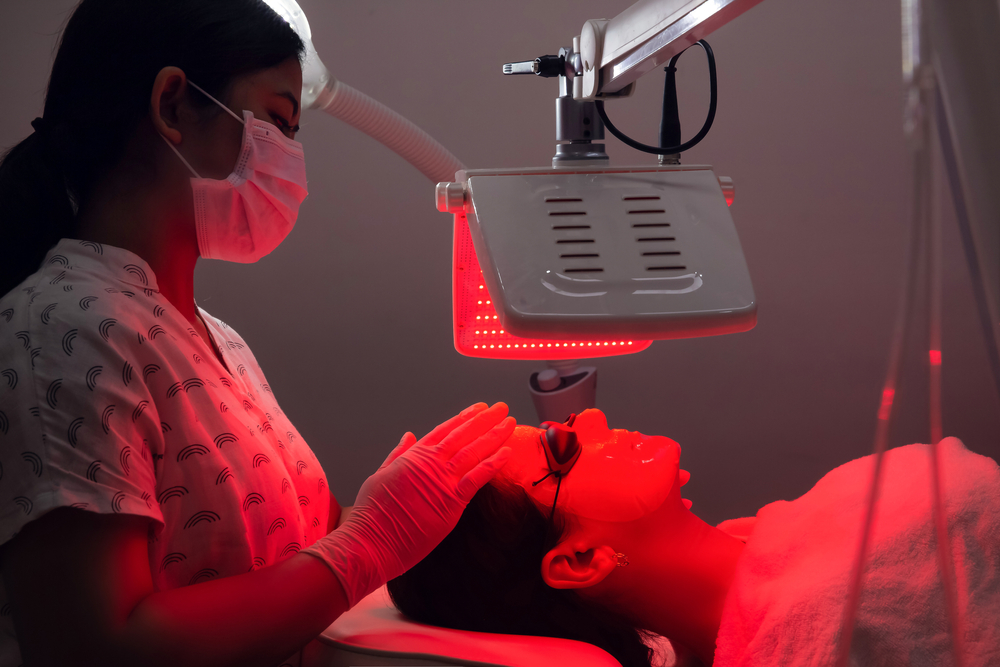
How effective is photodynamic therapy?
Many patients want to know, “Does photodynamic therapy work?” The answer is yes! The FDA has approved it to treat a variety of lung and esophageal cancers, which means it has undergone a rigorous testing process and is very effective. The procedure destroys tumor cells of various forms of cancer, manages symptoms of certain skin conditions, and treats acne breakouts by reducing sebum production. Studies have shown that photodynamic therapy works just as well to reduce the prevalence of cancerous cells as radiation therapy and surgery for certain forms of cancer or pre-cancer. Another benefit of the treatment is that it does not cause damage to normal cells and tissue in the treatment area. After the treatment, there may be redness, swelling, and irritation on the skin’s surface, but PDT is much less disruptive to the body as a whole than radiation therapy is, and it is non-invasive. The procedure is also outpatient, meaning patients can go home after the treatment rather than stay in the hospital or healthcare facility.
Frequently Asked Questions (FAQ’s) about Photodynamic Therapy
What is photodynamic therapy primarily used to treat?
Photodynamic therapy has a range of uses, from treating a wide variety of oncologic cancers to cosmetic concerns such as severe acne vulgaris and fine lines and wrinkles. The treatment’s collagen—and elastin-producing effects also make it effective in addressing signs of aging, such as fine lines and wrinkles and rough or pigmented patches of skin. However, its primary use is treating various types of cancers, including lung cancers, esophageal cancers, neck cancers, superficial non-melanoma skin cancers, and skin precancers.
Who can perform photodynamic therapy?
Only medical professionals like board-certified dermatologist Dr. Michele Green in New York City can perform photodynamic therapy.
What is photodynamic therapy for the face?
Photodynamic therapy can be used on the face to treat actinic keratoses and superficial non-melanoma skin cancers. The photosensitizing agent Levulan is applied to the face and left on for one hour to be absorbed by the pre-cancer and cancerous cells. A blue light is then applied to the treatment area to kill the harmful cells while leaving the surrounding cells unaffected. Photodynamic therapy can also treat acne vulgaris on the face, especially in patients who have not responded well to traditional topical or oral medications or Accutane. Sebaceous glands and hair follicles are damaged during treatment, reducing sebum production and shrinking the skin’s oil glands. Photodynamic therapy is a proven safe and effective method for treating skin precancers, cancers, and acne vulgaris with minimal downtime.
While photodynamic therapy is best known for cancer and pre-cancer treatments, research has begun to show that it can also be used for cosmetic purposes. According to a study by researchers in Germany (available on PubMed.gov, DOI: 10.1111/j.1610-0387.2012.08046.x), PDT treatment also eliminates fine lines and wrinkles in the treatment area and improves skin texture. The implications suggest that PDT could be useful in the lineup of treatments to reverse signs of the natural aging process. Dr. Green is an expert in cosmetic dermatology, helping her patients reduce the appearance of fine lines and wrinkles using the most innovative, non-invasive cosmetic procedures. When you consult with Dr. Green in her private NYC dermatology office, she will assess your skin concerns and devise a unique treatment plan to eliminate wrinkles for clearer, younger-looking skin.
What is photodynamic therapy for the eyes?
Photodynamic therapy for eyes treats age-related macular degeneration, a disease that impacts one’s central vision. PDT might be recommended for this disease if injections are ineffective or can’t be used. During PDT for the eyes, Verteporfin, a light-sensitizing medication, is injected into the bloodstream. The medicine collects in the abnormal blood vessels under the macula and is activated by laser light when it is shone into the eye, causing blood clots to form, which seal the blood vessels, slowing down central vision loss. PDT does not resolve any damage that has already occurred to the eyes. Side effects of photodynamic therapy for age-related macular degeneration can include temporary vision changes for several days, although any such side effects tend to resolve independently within 1-2 weeks. Photodynamic therapy for age-related macular degeneration takes about 20 minutes and may be done in an ophthalmologist’s office. Most patients require several treatment sessions to see optimal results.
How painful is photodynamic therapy?
Photodynamic therapy is a noninvasive treatment, but it may be painful or cause discomfort to some patients. Approximately half of patients report feeling stinging or burning during treatment, which typically resolves within a few minutes. During treatment, a fan can keep the skin cool. A cold compress can also be applied after treatment to reduce heat or stinging.
How long does photodynamic therapy take?
An appointment for photodynamic therapy typically takes approximately 90 minutes. When treating skin precancers, the photosensitizing agent Levulan must be applied to the entire treatment area and left on for one hour. Afterward, the skin is cleaned with water to remove any excess Levulan, and the treatment area is placed under the blue light for 16 minutes and 40 seconds. The incubation period of the photosensitizing agent and the time spent under the light source may differ depending on the exact concern being treated.

45-54 year old man treated with BLU-U light (2 weeks post treatment)
How long does photodynamic therapy last?
The length of time that photodynamic therapy lasts depends on various factors, including the concern being treated, the severity of the concern, and lifestyle factors. PDT can permanently eliminate actinic keratoses or precancers of the skin and superficial basal cell carcinomas. It has also been shown to treat superficial stage 0 squamous cell carcinomas, although reoccurrence is possible. PDT can be just as effective when treating lung or esophageal cancers, although repeat sessions may be required depending on the size and location of the cancer and the patient’s response to treatment.
Can I apply makeup after photodynamic therapy?
After photodynamic therapy, patients may experience mild skin redness, swelling, or irritation for several days. Dr. Green advises that you wait to wear makeup until the side effects have been resolved. When you come for the treatment, Dr. Green also suggests not wearing makeup, which must be removed before the photosensitizing agent is applied.
Can I exercise after photodynamic therapy?
Patients should avoid strenuous physical activity and excessive heat, including avoiding saunas, hot tubs, and jacuzzis, for 48 hours after treatment. Once the 48 hours have passed, patients can return to their regular exercise routines.
How much does photodynamic therapy cost?
The cost of PDT depends on several factors, including your geographic location, the type of institution you are receiving treatment from, and the size and scope of the treatment area. Photodynamic therapy is a very specialized treatment requiring specific equipment, which limits the number of dermatology offices that offer this special treatment, like Dr. Green’s New York dermatology office. PDT can be performed on several areas of the body that range in size, and the number of treatment areas or size of the treatment area can impact the price.
Does insurance cover photodynamic therapy?
If you are wondering if your insurance company covers photodynamic therapy, it is best to contact them directly. Different insurance companies have varying policies, so it is best to consult with your insurance company before coming in for treatment.
Does Medicare cover photodynamic therapy?
It is best to contact your insurance provider to determine if your health insurance covers the photodynamic therapy procedure.
What is the drawback of photodynamic therapy?
There are not many drawbacks associated with photodynamic therapy (PDT). PDT cannot treat melanoma skin cancers or invasive non-melanoma skin cancers. However, it is an excellent treatment for eliminating precancers and superficial non-melanoma skin cancers without invasive incisions or downtime. PDT treatment can result in side effects such as redness, swelling, and irritation, though these often resolve on their own within days of treatment. PDT can cause light sensitivity for several days or weeks following treatment, and it is essential to avoid direct light for the length of time designated by your healthcare provider. Compared to other aggressive forms of treatment, such as radiation or surgery, PDT is an excellent treatment for eliminating precancers, superficial non-melanoma skin cancers, certain lung or esophageal cancers, and acne vulgaris. PDT allows for full treatment of these conditions without harming the surrounding skin, allowing patients ease in scheduling their treatments.
Is photodynamic therapy worth it?
Yes! Photodynamic therapy treats several forms of head, neck, lung, and skin cancer, acne vulgaris, and other skin conditions. There is very little recovery time and limited risk of side effects. PDT is just as effective as radiation or surgical treatments for cancer cells without the recovery time needed for those treatments. Furthermore, while radiation therapy must be performed in moderation to limit damage to the treatment area, photodynamic therapy can be performed multiple times in the same location since there is no risk to the surrounding skin. With high precision, strong results, no downtime, and few side effects, therapy often finds photodynamic therapy to be a safe and highly effective treatment.
How do I get started with photodynamic therapy today?
Photodynamic therapy (PDT) is an excellent treatment option for patients with actinic keratoses, superficial non-melanoma skin cancers, acne vulgaris, photodamage, age-related macular degeneration, and certain head, neck, and throat cancers. PDT involves using a photosensitizing agent and a light source to kill harmful cells while leaving the surrounding skin unaffected. Depending on the concern being treated, one or multiple treatment sessions may be needed to achieve optimal results. Compared to other cancer treatments, photodynamic therapy has few mild side effects, and patients can look to returning to their daily activities soon following treatment. If you are interested in photodynamic therapy, Dr. Green will work with you to create a treatment plan that best suits your skin condition and leaves you with a healthy, radiant complexion that lasts.
Dr. Green is an internationally renowned expert in the field of dermatology with over 25 years of experience treating some of the world’s most discerning individuals for a myriad of skin conditions, including skin cancers, acne, and sun damage. Dr. Green is consistently voted one of New York City’s best dermatologists by Castle Connolly, New York Magazine, The New York Times, and Super Doctors for her dedication to her patients and expertise. When you consult with Dr. Green in her private Upper East Side dermatology office, Dr. Green will work with you to develop a customized treatment plan to address your specific skin concerns. To schedule a consultation with Dr. Green, learn more about various non-invasive skin rejuvenation treatment options, and get started with photodynamic therapy today, call the NYC-based office at 212-535-3088 or contact us online today.
 212-535-3088
212-535-3088 



